Articles
- Page Path
- HOME > Acute Crit Care > Volume 29(1); 2014 > Article
- Original Article The Effect of Positive End-Expiratory Pressure on Air Leakage: Comparison of Cuff Designs
- Junyong In, M.D., Gyung Serk Shim, M.D., Seunghyun Chung, M.D.
-
The Korean Journal of Critical Care Medicine 2014;29(1):3-6.
DOI: https://doi.org/10.4266/kjccm.2014.29.1.3
Published online: February 28, 2014
Department of Anesthesia and Pain Medicine, Dongguk University Ilsan Hospital, Goyang, Korea
- Correspondence to: Seunghyun Chung, Department of Anesthesia and Pain Medicine, Dongguk University Ilsan Hospital, 27 Dongguk-ro, Ilsandong-gu, Goyang 410-773, Korea, Tel: +82-31-961-7876, Fax: +82-31-961-7864, E-mail: jsh@dumc.or.kr
• Received: November 8, 2013 • Revised: November 25, 2013 • Accepted: November 25, 2013
Copyright © 2014 The Korean Society of Critical Care Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/3.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 4,823 Views
- 161 Download
- 2 Crossref
Abstract
-
Background:
- Recently developed taper-shaped cuffs (TG cuffs) of endotracheal tubes (ETTs) are known to have a more potent sealing effect than cylindrical high-volume low-pressure cuffs (HL cuffs) of conventional ETTs. The aim of this study was to compare TG cuffs with HL cuffs of ETTs in a bench-top model with regard to air leakage under various positive end-expiratory pressures (PEEP).
-
Methods:
- HL cuffs and TG cuffs made from PVC were included (HL group vs. TG group). A model trachea with an internal diameter (ID) of 22 mm was attached to a test lung. The test lung was ventilated using an anesthesia respirator with volume controlled mode and PEEPs of 0, 5, 10, or 15 cm H2O. Using spirometry, percentages of expired to inspired tidal volumes (TVe/i) were calculated as a measure of air leakage.
-
Results:
- With regard to PEEPs, the HL group showed significantly higher air leakage compared to the TG group (p < 0.0001), and a higher PEEP resulted in greater air leakage (p < 0.0001). Air leakage with higher PEEP was greater in the HL group than in the TG group at ID 7.0 mm and 7.5 mm (p = 0.0467, p = 0.0045)
-
Conclusions:
- This study shows the superior sealing ability of the TG cuff during ventilation at various PEEPs.
INTRODUCTION
METERIALS AND METHODS
RESULTS
DISCUSSION
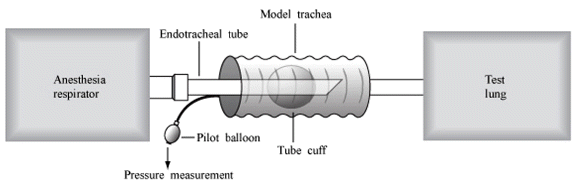
Fig. 1.The benchtop model. The model trachea was connected to a test lung. Anaesthesia respirator was connected to the proximal end of endotracheal tube (ETT), allowing for ventilation with recording of spirometry. In order to measure the cuff pressure manometer was attached to the pilot balloon of ETT.
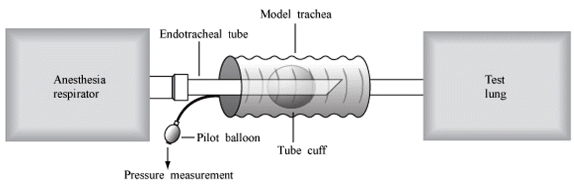

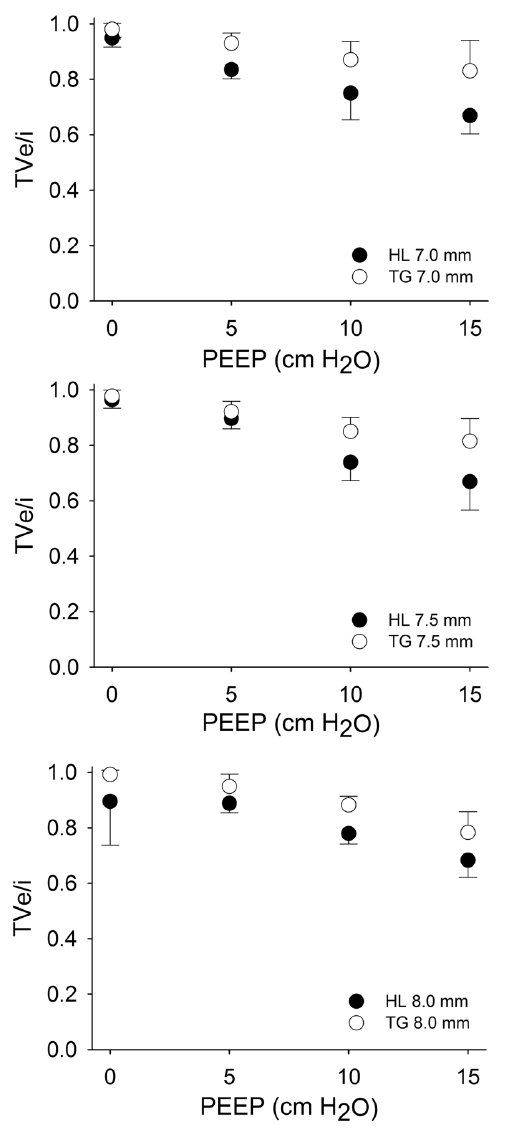
Fig. 2.The air leakage under various positive end-expiratory pressures (PEEPs). There are the differences in TVe/i (percentages of expired to inspired tidal volumes as a measure for air leakage) during ventilation with various PEEPs. For each size of tube, the Mallinckrodt Hi-LoTM tube (HL) group shows significantly higher air leakage compared with the Mallinckrodt TaperGuardTM (TG) group (p < 0.0001) and higher positive end-expiratory pressure (PEEP) triggered greater Tve/i (p < 0.0001). There are also some significant differences between the groups regarding interaction of cuff type and PEEP (two-way analysis of variance), which means that the TVe/i with higher PEEP are greater in TG tubes than in HL tubes (p = 0.0467 for IDs 7.0 mm and p = 0.0045 for IDs 7.5 mm).


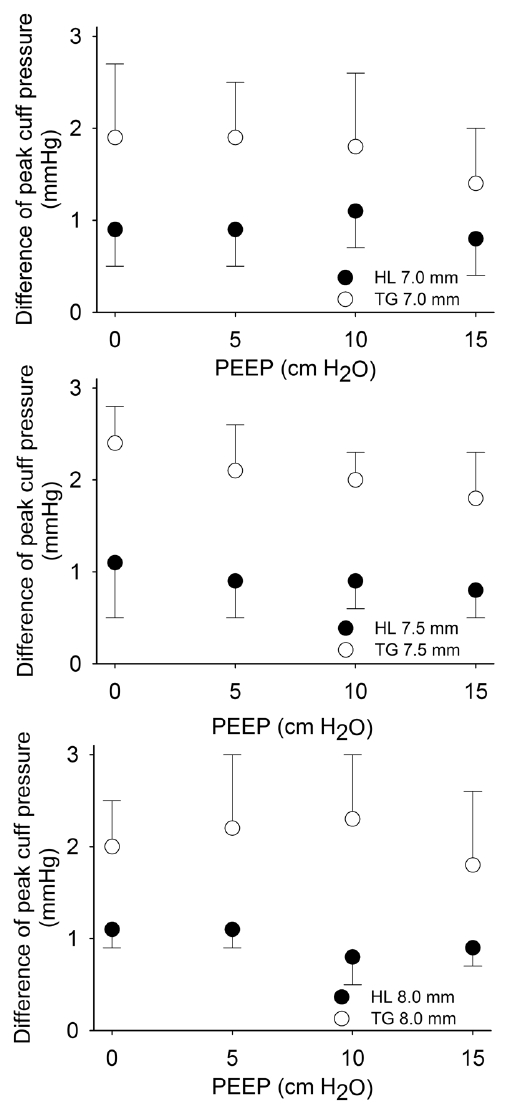
Fig. 3.The change in peak cuff pressures (Pcuff) during ventilation with positive end-expiratory pressures (PEEPs). The change of Pcuff in the TG group showed significantly higher than those in the HL group (p < 0.0001, respectively), but the level of PEEP does not have any significant effects on the change of Pcuff (p = 0.2552, 0.0573, and 0.3955, respectively). Two-way analysis of variance was applied with Pcuff and PEEP.


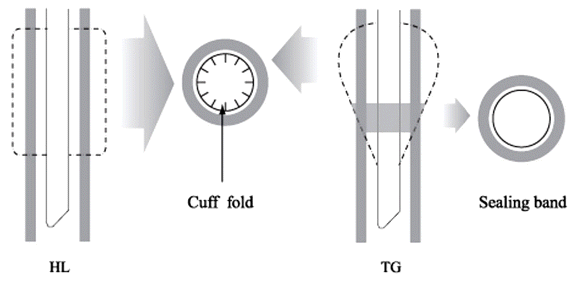
Fig. 4.Hi-LoTM tube (HL), TaperGuardTM tube (TG), and transaxial views. The diameter of HL cuff is larger than the tracheal diameter in the whole length of the cuff. Therefore longitudinal folds develop and act as a channel. But the tapering diameter of TG cuff fits into the exact tracheal diameter somewhere in the length, forming sealing band with minimal folds.
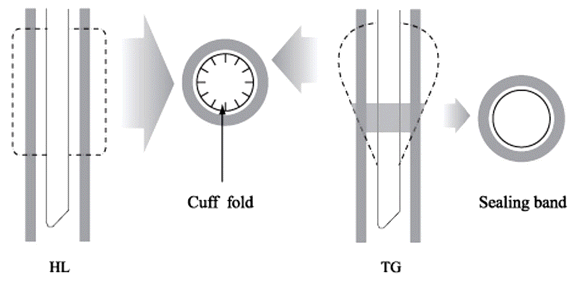

Table 1.Tested endotracheal tubes with cylindrical-shaped cuffs (Mallinckrodt Hi-LoTM) and tapered-shaped cuffs (Mallinckrodt TaperGuardTM)
Table 2.Differences in mean ratio of air leakages between the Hi-LoTM tube group with cylindrical-shaped cuff and the TaperGuardTM tube group with tapered-shaped cuff at 10 cmH2O of positive end-expiratory pressure
| Tube size ID (mm) | Difference | 95% CI | p value | |
|---|---|---|---|---|
| 7.0 | −0.120 | −0.210 | −0.031 | 0.0111 |
| 7.5 | −0.111 | −0.174 | −0.047 | 0.0021 |
| 8.0 | −0.103 | −0.140 | −0.066 | < 0.0001 |
- 1). Dullenkopf A, Gerber A, Weiss M. Fluid leakage past tracheal tube cuffs: evaluation of the new Microcuff endotracheal tube. Intensive Care Med 2003;29:1849-53.ArticlePubMed
- 2). Madjdpour C, Mauch J, Dave MH, Spielmann N, Weiss M. Comparison of air-sealing characteristics of tapered- vs. cylindrical-shaped high-volume, low-pressure tube cuffs. Acta Anaesthesiol Scand 2012;56:230-5.ArticlePubMed
- 3). Zanella A, Scaravilli V, Isgrò S, Milan M, Cressoni M, Patroniti N, et al. Fluid leakage across tracheal tube cuff, effect of different cuff material, shape, and positive expiratory pressure: a bench-top study. Intensive Care Med 2011;37:343-7.ArticlePubMed
- 4). Dave MH, Frotzler A, Spielmann N, Madjdpour C, Weiss M. Effect of tracheal tube cuff shape on fluid leakage across the cuff: an in vitro study. Br J Anaesth 2010;105:538-43.ArticlePubMed
- 5). Dullenkopf A, Schmitz A, Frei M, Gerber AC, Weiss M. Air leakage around endotracheal tube cuffs. Eur J Anaesthesiol 2004;21:448-53.ArticlePubMed
- 6). Main E, Castle R, Stocks J, James I, Hatch D. The influence of endotracheal tube leak on the assessment of respiratory function in ventilated children. Intensive Care Med 2001;27:1788-97.ArticlePubMed
- 7). Pitts R, Fisher D, Sulemanji D, Kratohvil J, Jiang Y, Kacmarek R. Variables affecting leakage past endotracheal tube cuffs: a bench study. Intensive Care Med 2010;36:2066-73.ArticlePubMed
- 8). Ouanes I, Lyazidi A, Danin PE, Rana N, Di Bari A, Abroug F, et al. Mechanical influences on fluid leakage past the tracheal tube cuff in a benchtop model. Intensive Care Med 2011;37:695-700.ArticlePubMed
- 9). Young PJ, Blunt MC. Improving the shape and compliance characteristics of a high-volume, low-pressure cuff improves tracheal seal. Br J Anaesth 1999;83:887-9.ArticlePubMed
- 10). Young PJ, Pakeerathan S, Blunt MC, Subramanya S. A low-volume, low-pressure tracheal tube cuff reduces pulmonary aspiration. Crit Care Med 2006;34:632-9.ArticlePubMed
- 11). Hwang JY, Park SH, Han SH, Park SJ, Park SK, Kim JH. The effect of tracheal tube size on air leak around the cuffs. Korean J Anesthesiol 2011;61:24-9.ArticlePubMedPMC
- 12). Guyton D, Banner MJ, Kirby RR. High-volume, low-pressure cuffs. Are they always low pressure? Chest 1991;100:1076-81.ArticlePubMed
- 13). Manzano F, Fernández-Mondéjar E, Colmenero M, Poyatos ME, Rivera R, Machado J, et al. Positive-end expiratory pressure reduces incidence of ventilator-associated pneumonia in nonhypoxemic patients. Crit Care Med 2008;36:2225-31.ArticlePubMed
- 14). Griscom NT, Wohl ME. Tracheal size and shape: effects of change in intraluminal pressure. Radiology 1983;149:27-30.ArticlePubMed
References
Figure & Data
References
Citations
Citations to this article as recorded by 

- Impact of Low‐Volume, Low‐Pressure Tracheostomy Cuffs on Acute Mucosal Injury in Swine
Alexandra J. Berges, Ioan A. Lina, Rafael Ospino, Hsiu‐Wen Tsai, Dacheng Ding, Jessica M. Izzi, Alexander T. Hillel
Otolaryngology–Head and Neck Surgery.2022; 167(4): 716. CrossRef - Tidal Volume Delivery and Endotracheal Tube Leak during Cardiopulmonary Resuscitation in Intubated Newborn Piglets with Hypoxic Cardiac Arrest Exposed to Different Modes of Ventilatory Support
Marc R. Mendler, Claudia Weber, Mohammad A. Hassan, Li Huang, Benjamin Mayer, Helmut D. Hummler
Neonatology.2017; 111(2): 100. CrossRef

 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite