Barriers and facilitators in the provision of palliative care in adult intensive care units: a scoping review
Article information
Abstract
The provision of palliative care in the intensive care unit (ICU) is increasing. While some scholars have suggested the goals of palliative care to not be aligned with the ICU, some evidence show benefits of the integration. This review aimed to explore and synthesize research that identified barriers and facilitators in the provision of palliative care in the ICU. This review utilized Preferred Reporting Items for Systematic Reviews and Meta-Analyses Scoping Review guidelines based on population, concept, and context. We searched for eligible studies in five electronic databases (Scopus, PubMed, ProQuest, Science Direct, and Sage) and included studies on the provision of palliative care (concept) in the ICU (context) that were published in English between 2005–2021. We describe the provision of palliative care in terms of barriers and facilitators. We also describe the study design and context. A total of 14 papers was included. Several barriers and facilitators in providing palliative care in the ICU were identified and include lack of capabilities, family boundaries, practical issues, cultural differences. Facilitators of the provision of palliative care in an ICU include greater experience and supportive behaviors, i.e., collaborations between health care professionals. This scoping review demonstrates the breadth of barriers and facilitators of palliative care in the ICU. Hospital management can consider findings of the current review to better integrate palliative care in the ICU.
INTRODUCTION
Palliative care (PC) is an interprofessional approach to care for patients with serious and complex illness aimed to optimize their quality of life by anticipating, preventing, and treating suffering when the patients are no longer responsive to curative therapies [1]. The provision of PC has shown many benefits including improved quality of life and reduced hospital admission and hospital stays [2]. Due to its benefits, the provision of PC is encouraged to be integrated into a health system, including in the intensive care unit (ICU) [3-5]. The provision of PC in the ICU is increasing, and all patients admitted to ICU should receive PC, which includes symptom management, patient-centered care, and shared-decision making [1,6,7].
Initially, provision of PC in the ICU aimed to improve end-of-life (EOL) care, which includes symptom management and shared decision-making [8]. A previous study showed that up to 20% of patients in an ICU were eligible for PC consultation [9]. Such a PC consultation is available to patients with the following conditions: (1) multisystem organ failure, (2) stage IV malignancy, (3) a stay 10 days or longer in the ICU, (4) intracerebral hemorrhage that requires ventilation, or (5) post cardiac arrest [9]. Thus, ICU-based PC could support patients and families and can provide a more comfortable environment, better healing, and increased awareness of EOL care [10]. It has been shown that PC can be an important component of care for all patients with life-limiting illness [11]. In addition, a current systematic review identified positive outcomes of PC provision in the ICU that include reduced length of hospital stay and reduced time on life-sustaining treatment [12].
The literature search found limited studies focusing on the barriers and facilitators of PC integration in the ICU. Therefore, this scoping review aimed to explore and map barriers and facilitators experienced by health care providers in addressing PC provision in the ICU.
MATERIALS AND METHODS
This scoping review was conducted and reported in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Review (PRISMA-ScR) guidelines [13]. We followed Arksey and O’Malley’s steps for conducting a scoping review: (1) identifying the research questions, (2) identifying relevant studies, (3) study selection, (4) charting data, (5) collating, summarizing, and reporting results, and (6) consultation with the experts [14].
Identifying the Research Questions
In a scoping review, it is fundamental to have a well-defined research question that includes the scope of the study, because it will allow researchers to conduct a more practical and efficient review [15]. There were two research questions for the present review: (1) What are barriers of PC provision in the ICU? and (2) What are facilitators of PC provision in the ICU?
Identifying Relevant Studies
We searched the five electronic databases PubMed (Medline), Science Direct, ProQuest, Scopus, and Sage to identify published studies that met the inclusion criteria. We searched using keywords that were developed based on our questions: “palliative care,” “end-of-life care,” “terminal care,” “intensive care,” “ICU,” and “critical care.” We exported all identified records to Endnote 20 Software (Clarivate Analytics, Philadelphia, PA, USA) and used it to remove duplicates automatically.
Study Selection
Each title and abstract of the retrieved articles were screened independently by two reviewers (ER and SA) to assess adherence to the inclusion criteria. Inclusion criteria were (1) studies about PC or EOL care in adult ICU, (2) studies with quantitative, qualitative, or mixed method designs, (3) publication year 2005–2021, and (4) published in English. Review articles and protocols were excluded. Full-text articles were reviewed independently and then discussed to confirm if the full-text articles met the inclusion criteria. Any discrepancies between the two reviewers at any stage of the selection process were discussed and settled with a third reviewer.
Charting the data
The fourth step was charting the data. A table for extracting details, characteristics, and results of studies based on the Joanna Briggs model was developed [16]. Each of the 14 included studies was read several times by four reviewers (CE, YO, SA, and ER) to ensure that all information was included. We developed a table to chart and capture all relevant important information. Categories included in the charting data stage were: (1) author and publication year, (2) aim of the study, (3) context of the study (country, type of ICU), (4) study design, and (5) respondents (number of participants, characteristics) and study findings.
Consultation to Expert
The consultants’ roles were to provide additional references on potential studies for inclusion in the review, as well as valuable insights into the issues identified. In this study, the process involved an experienced critical care nurse and an anesthetic doctor who served in the ICU as a consultant; both were asked for their opinions regarding the study findings. Both experts agreed with the findings and highlighted the importance of hospital policy related to the provision of PC in an ICU.
RESULTS
Search Results
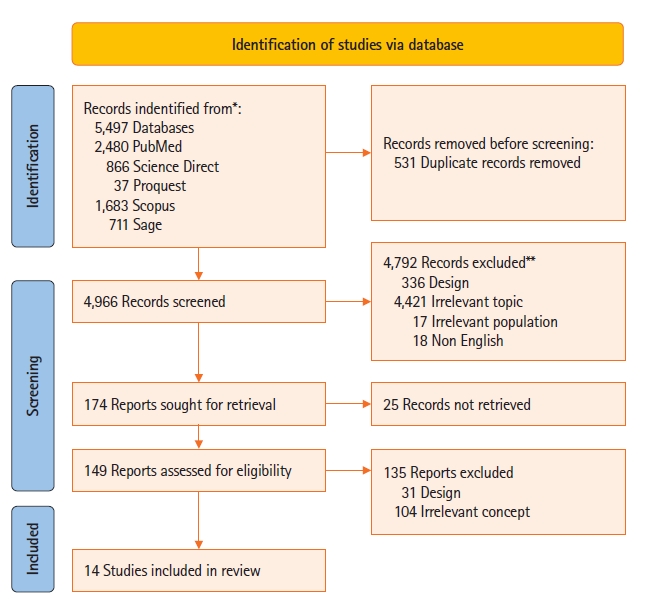
We found 5,499 studies during the literature search. After removing 531 duplicate articles, the remaining 4,985 articles were further examined based on inclusion criteria by titles and abstracts. In the title and abstract screening, articles that did not meet the inclusion criteria were removed. A total of 149 full text articles was screened independently and discussed to determine relevance. The research flow of articles through identification of final papers is represented in Figure 1.
Characteristics of the Included Studies
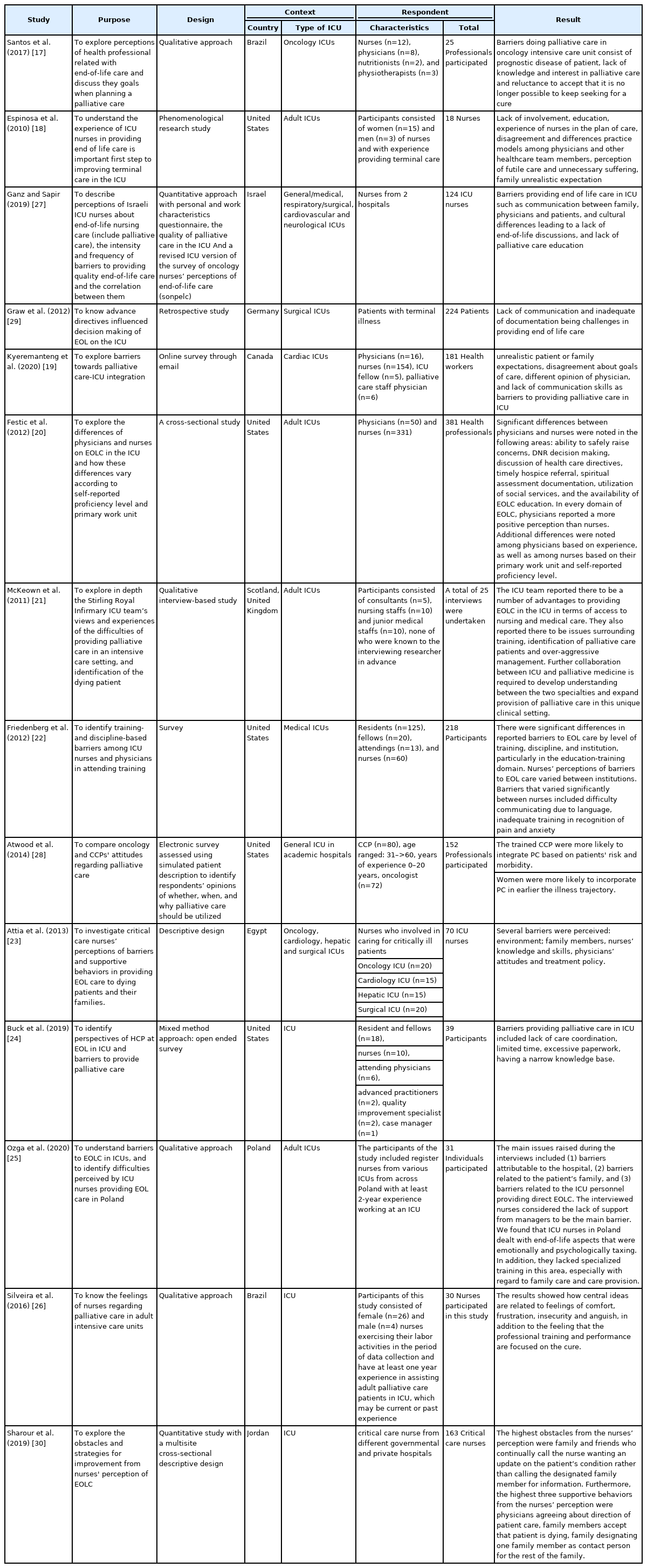
A total of 14 papers was reviewed in the current scoping review (Table 1) [17-30]. The included studies were performed in nine countries: Egypt (n=1), United States (n=5), Brazil (n=2), Israel (n=1), Germany (n=1), Canada (n=1), Poland (n=1), Scotland (n=1), and Jordan (n=1). The total number of participants was 2,015, comprising patients and relatives (n=324) and health care professionals (HCPs) that included nurses (n=1.499), physicians (n=159), and other HCPs (n=33). The papers explored the provision of EOL care (n=10) in intensive and critical care (n=4) units.
Barriers on the Provision of PC in the ICU
After reviewing the literature, barriers and facilitators were identified. The barriers were lack of capabilities, family boundaries, practical issues, and cultural differences. Further analysis of each barrier found in this review is described below.
Lack of capabilities
There are several barriers to the provision of PC in an ICU. The limited capabilities of HCPs were the most significant barrier [17-28], due in part to shortcomings in PC training [17,28]. In addition, a study conducted by Ozga et al. [25] highlighted the absence of hospital management support in providing training on EOL care. This hinders nurses from acquiring a better understanding of PC, particularly in EOL care. The inadequacy of educational and training for EOL care was perceived as a barrier to integrate PC into the ICU, dealing with death and dying issues, and lack of communication. A study conducted by McKeown et al. [21] stated that education could equip an ICU team to deal with issues surrounding PC as well as death and dying. Four studies found insufficient communication between medical teams and family members [17-19,23]. Evidence from included studies showed lack of communication with patients and families related to decision-making by HCPs [18,19,29].
Family boundaries
Another barrier is family boundaries, an enduring problem in the integration of PC into ICU protocols [18,19,24,27,29-31]. Many families in such situations have unrealistic expectations, which can lead to difficulties for HCPs in applying PC principles based on comfort care and may lead to aggressive treatment for the patients [18,19,23]. A study conducted by Kyeremanteng et al. [19] found unrealistic patient or family expectations as a barrier in providing EOL care in the ICU. This is because the family lacked the necessary medical knowledge and did not fully understand the condition of the dying patient. Unrealistic expectations also were found by Espinosa et al. [18], who identified unrealistic expectations as barriers to PC, particularly during EOL care.
Practical issues
Practical issues are also a considerable barrier to PC delivery in the ICU [18-20,23,29,32]. These issues include limited time for administrative tasks and documentation, disagreement about goals of care between HCPs, differences in nursing and medical approaches, and administrative policy treatment. During providing PC in the ICU there are often agreements and disagreements between HCPs. For example, agreement between HCP was found in Festic et al.’s study [20] that both physicians and nurses agree if patient’s death was not the result of treatment failure. In addition, they thought that providing EOL care for dying patients and their families is a rewarding experience. Meanwhile, disagreement among physicians and nurses is common when providing EOL care in the ICU. Nurses often feel uninvolved in the treatment plan for dying patients, simply carrying out actions discussed and decided only by doctors and families [18,19]. Inadequate policies and practices were identified as barriers to EOL care in the ICU [20].
Differences between medical and nursing models, which were reported as barriers, showed that medical models are focused more on disease or dysfunction, while most nurses are trained in a holistic model to consider all aspects of the patient. The difference between these two models can create difficulty when nurses try to implement physician directions, resulting in nurse frustration, especially in providing EOL care [18]. Practical issues also can be caused by lack of documentation; a study conducted by Graw et al. [29] found that lack of documentation related to advance directives was a significant barrier for health workers in providing care as desired by patients. In addition, barriers including lack of coordination, limited time and staff, and ethical issues were identified [31].
Cultural differences
Cultural difference is another barrier in the provision of PC in the ICU. In this review, only one paper highlighted cultural differences [27]. Ganz and Sapir [27] state that doctors in Asia are more aggressive in their treatment than those in the West. This finding may be due to cultural differences, as death is often not openly discussed in Asia, which can lead to lack of discussion about EOL decisions.
Facilitators in the Provision of PC in ICU
Several facilitators have been identified and include experiences and supportive behavior. Further analysis of each facilitator found in this study is described below.
Supportive behaviors
Sharour et al. [30] identified some supportive behaviors in providing EOL care, including collaboration among physicians and other HCPs to stop aggressive treatment and start EOL care, thereby improving family acceptance. In addition, family acceptance regarding patient death can reduce suffering and psychosocial distress and improve the quality of life for families and their time with patients. Another helpful behavior is appointing one of the family members to communicate with the nurse. This can make it easier for nurses to explain the patient’s condition and EOL care, possibly increasing the effectiveness of treatment and reducing the nurses’ workload.
Previous experiences
Another facilitator is experience, which was identified in a previous study. Festic et al. [20] found that nurses and attending physicians who have longer working experience state have higher agreement on conducting EOL discussion than fellow physicians. Experience is influenced by length of working and the context where the HCP works Experience can lead HCPs in providing EOL care, and ample experience could result in better quality of EOL care [20].
DISCUSSION
This study provides a comprehensive review of the research evidence on the barriers and facilitators in PC provision in the ICU. Further, this review highlights barriers to such provision, including lack of capabilities (knowledge, skills, communications), family boundaries, practical issues, and cultural differences. Facilitators of previous experience and supportive behavior also were identified from the included studies. While, in theory, the ICU and PC principles and practices may seem to be opposites, the two share a similar fundamental goal to provide quality care to patients [1]. PC is increasingly accepted as an essential component of comprehensive care for critically ill patients, regardless of age, diagnosis, and prognosis [33]. The provision of PC has grown exponentially during the last decade. In this regard, data regarding implementation of PC in the ICU setting is lacking due to the common practice of referring PC patients to hospice care, which is commonly offered in a non-hospital setting [1]. In the coming decades, evidence and knowledge translation in PC, intensive care, and their integration will expand further [34].
Barriers in the Provision of PC
Ongoing barriers for optimal integration of PC in the ICU setting have been identified. The provision of a high quality of care for patients who are nearing their EOL is the professional responsibility of health care workers [35]. Therefore, it is crucial for health professionals who work in the hospital to be competent in basic PC and EOL care. However, physicians and nurses continue to lack knowledge in the necessary communication skills, including communicating with family and patients about outcomes and managing clinical aspects of poor outcomes [36]. This limitation may be caused by limited availability of training and education [37]. A study found that a lack of knowledge was more prevalent in female compared to male healthcare professionals and less frequently in physicians [38]. In addition, knowledge deficits were more prevalent in healthcare professionals who had little contact with dying patients [38]. Healthcare professionals who worked with seriously ill or dying patients had higher motivation for quality care compared to those who did not have such contact [38]. However, one study found that critical care nurses felt inadequate and unprepared to provide quality EOL care in the ICU [39]. Regarding EOL decision making skills, a study found that European physicians had no difficulty in making EOL decisions in 81%–93% of cases. In contrast, such decisions were perceived to be difficult by Indian physicians due to barriers of lack of awareness of ethical issues, culture of heroic “fighting till the end,” and lack of PC orientation [40].
Another study supported our findings that the main obstacles of EOL care by doctors and nurses in critical care units were lack of education and training regarding family grieving and quality of EOL care [41]. Training on implementation of PC in the ICU could improve the capabilities of nurses and physicians. For example, two studies reported that training can improve PC knowledge and skills, particularly in symptom management and communication [42,43].
Another barrier in EOL care is cultural differences. Our study confirmed previous findings from Asia that physicians in ICUs frequently withheld but rarely withdrew life-sustaining treatment [44,45]. A study from Asia reported an ethical dilemma involved in withholding and withdrawal of treatment among Asian nurses, where withholding is considered more ethical than withdrawing treatment [46].
While there were several barriers identified, we found previous experiences of HCPs facilitate the provision of PC in the ICU. This finding aligns with a previous study among ICU nurses in which the respondents were classified into two groups based on work experience. Jang et al. [47] reported that the more experienced group tended to consider EOL care.
In addition to experience, supportive behaviors also facilitate the provision of PC. Supportive behaviors such as transformational leadership and supportive inquiry conditions were also reported in two previous studies. For example, the application of transformational leadership was able to create good daily working environments including adequate staffing and has been suggested as contributing to successful implementation. Moreover, facilitation, in the sense of individuals or strategies that make change easier, has recently been strengthened as a crucial component for implementation of EOL care. Another study reported that peer emotional support has a facilitating role for EOL care in the ICU [31].
This literature review applied the six steps of Arksey and O’Malley guidelines, including the sixth step of consulting experts. The experts validated that all articles met the criteria and examined both clinical and practical related contexts. The keywords used were broader compared to PC articles in the ICU setting and included PC, end of life care, and terminal care. This resulted in a large number of identified articles.
CONCLUSIONS
Implementing PC in the ICU is increasingly recognized. However, the implementation of this PC care in the ICU settings has faced some barriers such as lack of capabilities among doctors and nurses, family boundaries, and cultural differences. The facilitators in implementing PC in the ICU setting include health care provider experience and supportive behavior within the organization.
KEY MESSAGES
▪ The provision of palliative care in intensive care units (ICUs) is advocated to improve end-of-life care and patient’ quality of life, and to reduce hospital admission and hospital stays.
▪ This review maps a lack of capabilities and family boundaries as barriers in the integration of palliative care in the ICU
▪ Experiences and supportive behaviors are identified as facilitators in the provision of palliative care in ICUs.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
FUNDING
None.
AUTHOR CONTRIBUTIONS
Conceptualization: CE, YY, ER, Data curation: ER, SA. Formal analysis: ER, SA. Funding acquisition: ER. Methodology: CE, YY, ER. Project administration: SA. Writing–original draft: all authors. Writing–review & editing: all authors.
Acknowledgements
This was part of a larger study funded by the Institute of Research and Innovation, Universitas Muhammadiyah Yogyakarta. The authors thank the Institute of Research and Innovation, Universitas Muhammadiyah Yogyakarta.