Clinical characteristics and outcomes of obstetric patients transferred directly to intensive care units
Article information
Abstract
Background
Medical complications in peripartum patients are uncommon are uncommon. Often, these patients are transferred to tertiary care centers, but their conditions and outcomes are not well understood. Our study examined peripartum patients transferred to an intensive care unit (ICU) at an academic quaternary center.
Methods
We reviewed charts of adult, non-trauma, interhospital transfer (IHT) peripartum patients sent to an academic quaternary ICU between January 2017 and December 2021. We conducted a descriptive analysis and used multivariable ordinal regression to examine associations of demographic and clinical factors with ICU length of stay (LOS) and hospital length of stay (HLOS).
Results
Of 1,794 IHT peripartum patients, 60 (3.2%) were directly transferred to an ICU. The average age was 32 years, with a median Sequential Organ Failure Assessment (SOFA) score of 3 (1–4.25) and Acute Physiology and Chronic Health Evaluation (APACHE) II score of 8 (7–12). Respiratory failure was most common (32%), followed by postpartum hemorrhage (15%) and sepsis (14%). Intubation was required for 24 (41%), and 4 (7%) needed extracorporeal membrane oxygenation. Only 1 (1.7%) died, while 45 (76.3%) were discharged. Median ICU LOS and HLOS were 5 days (2–12) and 8 days (5–17). High SOFA score was linked to longer HLOS, as was APACHE II.
Conclusions
Transfers of critically ill peripartum patients between hospitals were rare but involved severe medical conditions. Despite this, their outcomes were generally positive. Larger studies are needed to confirm our findings.
INTRODUCTION
Although medical complications among peripartum patients are uncommon, serious conditions may develop and necessitate greater resources and expertise for treatment [1]. Therefore, when these patients’ medical care may exceed the capability of the nearby hospitals they present first, they often require an interhospital transfer (IHT) to tertiary care medical centers. The prevalence of IHT of peripartum patients is uncommon, as only 0.6% of all IHT patients are pregnant [2]. Therefore, the disease states and associated outcomes of IHT peripartum patients transferred directly to an intensive care unit (ICU) are not well described in the literature. Among the current research on peripartum patient interhospital transport, most studies cover medical management during transport rather than the factors contributing to outcomes after transport [1,3-6].
Most peripartum IHT patients were transferred for either fetus or delivery-related care, and they were mostly transferred to a labor and delivery (L&D) unit. There was a very small number of patients who were subsequently upgraded to ICU-level of care and their demographics and clinical outcomes were described [7]. However, characteristics of patients who were transferred directly from other hospitals to an ICU at a tertiary care center has not been described. This information is of particular importance during the coronavirus disease 2019 (COVID-19) pandemic due to the strained resources and limited capacity in ICUs. Therefore, the need to triage peripartum patients who directly transferred to ICUs is important for both referring and accepting physicians to provide the best care for patients while optimize resource allocation during this current time of strained resources.
The purpose of this study was to describe clinical characteristics and outcomes of peripartum patients directly transferred to ICUs at a large academic quaternary medical center. Furthermore, we sought to explore the characteristics that might have been associated with their outcomes.
MATERIALS AND METHODS
Study Setting and Patient Selection
We performed a retrospective analysis of all adult peripartum patients whose ages were >18 years, and were transferred directly from any unit at other hospitals to any ICU at the University of Maryland Medical Center (UMMC). The study period was January 01, 2017 to December 31, 2021. Adult peripartum patients who were first transferred to our L&D unit followed by ICU admission due to clinical deterioration were excluded. Peripartum patients who were transferred for gynecologic conditions (pelvic mass, ovarian torsions, etc.) were also excluded.
The UMMC is an academic quaternary care medical center with a L&D unit and six specialized adult ICUs (coronary care unit, cardiac surgical ICU, critical care resuscitation unit, medical ICU, neurocritical care unit, surgical ICU). The L&D unit is staffed around the clock by the obstetrics and gynecology (OBGYN) team. Most of the adult specialized ICUs at UMMC are staffed by fellow physicians between 7 pm and 7 am, while the critical care resuscitation unit is staffed around the clock by an attending physician and an advanced practice practitioner [8]. The on-call OBGYN team can also consult the maternal fetal medicine (MFM) fellow physician for critically ill patients. During a transfer request, the MFM physician and the ICU attending physicians would decide whether patients can be directly admitted to the ICU or patients can go to our institution’s L&D unit. During a peripartum patients’ stay at any ICU at UMMC, the patients’ care is directed by the primary ICU team, with the MFM and OBGYN teams serving as consultants. Once the patient no longer requires ICU level care, they are transferred to the L&D unit for continuation of care by the OBGYN team.
This investigation was approved by the Institutional Review Board of University of Maryland, Baltimore (No. HP-00084554), and formal consent was waived by the Institutional Review Board.
Outcome Measures
The primary outcome of this study was hospital length of stay (HLOS) of these critically ill peripartum patients. The secondary outcome was the ICU length of stay (ICU LOS) for these patients. Prior literature suggests low mortality among peripartum patients [1], therefore, mortality was not selected as an outcome for analysis in this study.
Data Extraction
Patients’ demographics, maternal medical history, and clinical factors were collected from our institution’s electronic medical records and were entered into a standardized Excel spreadsheet (Microsoft). Clinical factors included components to calculate APACHE II score, the Sequential Organ Failure Assessment (SOFA) score, white blood cell count, serum lactate levels and interventions during ICU stay. Missing data was inputted as normal values. Prior to data collection, investigators who were not blinded to the study hypothesis were trained with sets of five patients' charts until data accuracy reached 90% between the investigators.
Statistical Analysis
Data was presented using descriptive analyses, using mean (±standard deviation [SD]), median (interquartile range [IQR]), and percentages when appropriate. For continuous variables, their histograms were visually inspected for patterns of distributions, and they were described with mean or median accordingly. Ordinal logistic regressions were performed to measure the association of clinical factors and patients’ HLOS or ICU LOS. We used the histograms to determine the distributions of length of stay and ranked the order according to their frequencies. The order for hospital length of stay was ranked from 0 days (0–5), 1 days (5.1–10), 2 days (10.1–15), to 3 days (≥15). The order for ICU length of stay, due to its histogram, was ranked from 0 days (0–2), 1 days (2.1–4), 2 days (4.1–12), to 3 days (≥12). Results from the ordinal logistic regression were expressed as correlation coefficient (r-value), odds ratio (OR), 95% confidence interval (95% CI), and P-value. A positive coefficient would make the event associated with rank 0 (shortest HLOS, ICU LOS) most likely and the event next to it less likely. A negative coefficient would make the event associated with the last rank (longest HLOS, ICU LOS) most likely. The predictive ability of the model was assessed by the Somers’ D, Goodman-Kruskal gamma tests. Models with Somers’ D and Goodman-Kruskal gamma approaching –1 or 1 would have a very good predictive ability. All independent variables considered important for patients’ outcome were determined a priori. In the final analysis, we also removed independent variables with a wide 95% CI to improve our models’ performance. Descriptive analyses and multivariable ordinal logistic regressions were performed by Minitab ver. 20 (https://www.minitab.com). All analyses with P-value <0.05 were considered statistically significant.
RESULTS
Patient Demographics and Clinical Characteristics
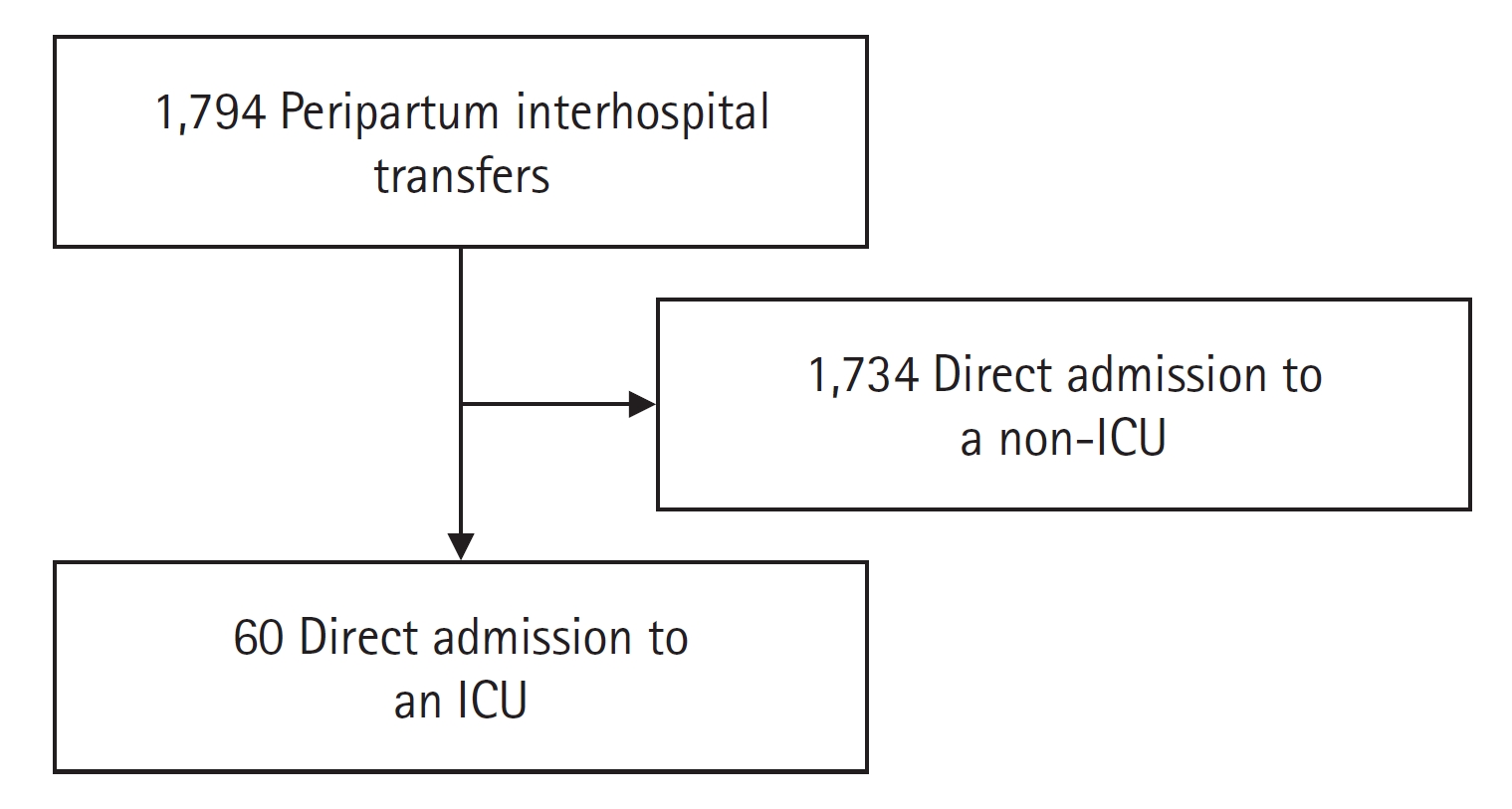
During the study period, there were a total of 1,794 peripartum patients being transferred to our institution. Sixty patients (3.2%) were transferred directly to an ICU and their charts were analyzed (Figure 1). The mean of the patients’ age was 32 years (SD, 6) and 29 (48%) were postpartum (Table 1). The most common diagnosis for ICU admission was COVID-19 related respiratory complications (n=16, 26.7%), postpartum hemorrhage (n=9, 15%) and pregnancy-induced hypertensive disorders (n=8, 13.3%) (Table 1).

Demographic factors of peripartum patients transferred to any ICU at an academic quaternary medical center (n=60)
The median (IQR) values for SOFA scores and APACHE II score at ICU admission were 3 (1–4.25) and 10 (7–12). These 24-hour physiologic scores were significantly lower after admission to ICU: 24-hour SOFA score was 2 (0.75–4) and APACHE II score 5.5 (3–9), respectively (Table 1). Although 24 patients (40%) received surgical intervention after being transferred to the ICU (Table 1), the most common ICU interventions for these patients were intubation (n=24, 40%), transfusion of blood products (n=20, 33.3%) and initiation of a continuous antihypertensive infusion (n=10, 16.7%) (Table 2).
Primary Outcome: Hospital Length of Stay
Among the 60 patients transferred directly to any ICU at UMMC, only 1 (1.7%) died, one patient was discharged to a skilled nursing facility, while 54 (90%) were discharged home directly, three were discharged to a rehabilitation facility (Table 1). The median hospital length of stay for these critically ill patients was 8.8 days (4.4–15.6 days).
Multivariable ordinal logistic regression showed that COVID-19 positivity (r=–1.92; OR, 0.15; 95% CI, 0.03–0.78; P=0.02), higher SOFA score (r=–0.40; OR, 0.67; 95% CI, 0.50–0.91; P=0.01) upon ICU admission were associated with longer hospital stay (>15 days) (Table 3). This multivariable ordinal logistic regression demonstrated good predictive ability with good Somers’ D and Goodman-Kruskal Gamma values both at 0.74.
Secondary Outcome: ICU Length of Stay
The median (IQR) ICU length of stay was 4.4 days (2.1–11.2 days). Again, COVID-19 positivity (r=–1.85; OR, 0.16; 95% CI, 0.03–0.77; P=0.02) was associated with longer ICU stay (Table 4). However, high APACHE II, but not SOFA score at ICU admission was associated with longer ICU stay (r=–0.16; OR, 0.85; 95% CI, 0.74–0.99; P=0.04). This multivariable ordinal logistic regression only has acceptable predictive ability, as its Somers’ D and Goodman-Kruskal Gamma values were 0.63.
DISCUSSION
The study demonstrated a number of medical complications, interventions and risk factors for ICU and hospital length of stay for a group of peripartum patients. Our study highlights a variety of clinically significant factors and outcomes among peripartum patients directly transferred to ICUs from inpatient units at other hospitals. A rising trend among peripartum patients is the greater number of comorbidities of these patients, such as obesity [9]. Additionally, the common comorbidities among our small patient population were hypertension and asthma. This trend of more peripartum with comorbidity results in the requirement for more advanced resources and expertise that are only available at tertiary and quaternary care centers. Due to this increasing frequency of the transfer of critically ill peripartum patients from nearby hospitals, especially during the COVID-19 pandemic, the need to characterize patient disease states and outcomes is also rising. Although previous studies have described clinical characteristics of peripartum patients admitted to the ICU [10], there is a paucity of studies exploring clinical factors and outcomes of peripartum patients transported from nearby hospitals to an ICU at a quaternary care center.
Previous research has indicated that the most common diagnoses for peripartum patients requiring ICU admission include obstetric hemorrhage and hypertensive disorders [11]. Similarly, our findings indicate that while the three most common diagnoses include respiratory complications, postpartum hemorrhage, and pregnancy-induced hypertensive disorders, respiratory failure was the most common indication for transfer to our institution’s ICU. Additionally, another notable diagnosis in our cohort was preeclampsia/eclampsia, a common diagnosis for peripartum ICU patients in the literature [12]. The increased frequency of respiratory complications most likely arose from the COVID-19 pandemic due to the timeline of our research study. COVID-19 pneumonia greatly contributed to the incidence of acute respiratory distress syndrome (ARDS), among peripartum patients [13]. However, it was interesting to note that only one patient from the number of peripartum patients within our study required extracorporeal membrane oxygenation (ECMO) support. This information would indicate that, while peripartum patients are high risk, they may still have enough physiologic reserves. Thus, with proper support, these high-risk patients would have good outcomes. Overall, besides COVID-19 related respiratory complications, our cohort’s primary diagnoses are largely similar to those of ICU peripartum patients in general, indicating concordance between IHT ICU peripartum diagnoses and ICU peripartum patients in general.
On average, patients in this study had improved physiological indices, including reduction in both APACHE II and SOFA score, 24 hours after admission to the ICU indicating efficient interventions and improved disease severity. A large proportion of our cohort had a primary diagnosis of respiratory failure, largely induced by COVID-19. Prior research has illustrated that COVID-19 mortality for patients admitted to the ICU was significantly predicted by SOFA score and APACHE II score [14]. Although the SOFA and APACHE II scores have not been validated among peripartum patients, our study suggested that these physiologic indices may also be applicable for this high-risk patient population, although further studies will be necessary to confirm this.
Additionally, previous research has indicated that the best predictor for outcomes for pregnant women with sepsis is SOFA score [15], and outcomes for patients with postpartum hemorrhage are strongly predicted by both the SOFA and APACHE II scores [16]. Findings from this study were in agreement with these results as higher SOFA and APACHE II scores upon admission at our institution’s ICU were significantly associated with either longer ICU length of stay or longer hospital length of stay. It is also intuitive to observe that COVID-19 positivity is associated with both longer ICU and hospital length of stay because COVID-19 infection had been described as earlier contributes to the exacerbation of ARDS which is resource-intensive and historically leads to greater HLOS and ICU LOS [17].
Given that our study uniquely examines IHT peripartum patients who are admitted directly to an ICU rather than the sparse literature on peripartum ICU patients which include all ICU admits and are not specific to IHTs, we compared our cohort’s HLOS with those of samples in the literature. Our findings largely agree with the literature; specifically, one study found that peripartum patients admitted to ICUs had a median HLOS of 9 days (7–16 days) [18], whereas our cohort had a median HLOS of 8.8 days (4.4–15.6 days). Given the similar median and overlapping IQR’s, our findings suggest a non-significant difference in HLOS between IHT ICU peripartum patients and ICU peripartum patients overall.
Although patients in this study were associated with improvement of their physiologic indices within 24 hours. Our analysis did not show an association whether this improvement was associated with outcomes although a previous study suggested that an improvement of SOFA score, even during a short period of time, would be associated with patient’s increased odds of hospital survival [19]. The discrepancies could be multifactorial. Our study did not use mortality as an outcome, as there was only one death in this study. Another factor would probably be due to the smaller sample size of the study, which would not be able to detect the signals in this study.
Our study did have a number of limitations. This study only represents a single academic center which has its own policies and procedures for transport criteria. Thus, our findings may not be generalizable. Next, peripartum patients make up a very small number of IHTs, limiting our sample size and limited our ability to perform more advanced statistical analyses to further characterize our cohort. Additionally, this study timeline overlaps with the COVID-19 pandemic, overrepresenting the number of patients transferred to due to respiratory conditions. Our study did not take into account any management during the transport process because of the paucity of the transport team’s documentation. This study may also be limited in its ability to provide comprehensive conclusions due to the lack of a control population. Peripartum admits to an ICU is a very rare occurrence, with some institutions having less than 80 over the course of a decade [18]. Furthermore, our study further stratifies this already uncommon population by specifically examining peripartum patients who are IHTs to an ICU. However, given that clinicians have a very low threshold to admit or transfer peripartum patients to the ICU, such comparisons are very limited, since there are a very limited number of comparable non-ICU peripartum patients who would have similar clinical characteristics but are not in the ICU. Therefore, the scope of the analysis is limited to adding an understanding to the literature on the clinical characteristics, interventions, and outcome of this unique population rather than attempt to provide predictors for which peripartum patients should or should not be admitted to the ICU. We do, however, implore future research to include such comparisons to enhance the complexity of conclusions that can be made on this unique patient population.
This study demonstrated that a wide range of medical complications prompted the IHT of a small number of peripartum patients who were transferred directly to an ICU at an academic quaternary medical center. These high risk peripartum patients also underwent a number of clinical interventions ranging from invasive mechanical ventilation to ECMO cannulation. However, the outcomes for these high-risk patients are generally good, as there was only one death, and most patients were discharged home directly from the hospital.
KEY MESSAGES
▪ Although the transfer of critically ill peripartum patients was uncommon between hospitals, these patients often had severe medical conditions.
▪ Despite this, the outcomes of these interhospital transfer peripartum patients were generally good.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
FUNDING
None.
AUTHOR CONTRIBUTIONS
Conceptualization: KB, AL, EE, QT. Data curation: SP, SA, FA. Formal analysis: JY. Methodology: KB, AT, AL, EE, QT. Project administration: AL, QT. Writing–original draft: SP, KB, QT. Writing–review & editing: LB, QT.
Acknowledgements
None.
SUPPLEMENTARY MATERIALS
Supplementary materials can be found via https://doi.org/10.4266/acc.2023.01375.
Diagnosis of peripartum patients transferred to any ICU (n=60)
acc-2023-01375-Supplementary-Table-1.pdf