Abstract
- We herein describe a 70-year-old woman who presented with respiratory failure due to extensive lung adenocarcinoma. Despite advanced disease, care in the intensive care unit with ventilator support was performed because she was a newly diagnosed patient and was considered to have the potential to recover after cancer treatment. Because prompt control of the cancer was needed to treat the respiratory failure, empirical treatment with an oral epidermal growth factor receptor (EGFR) tyrosine kinase inhibitor was initiated before confirmation of EGFR-mutant adenocarcinoma, and the patient was successfully treated. Later, EGFR-mutant adenocarcinoma was confirmed.
-
Keywords: erlotinib; mechanical ventilation; non-small-cell lung cancer; respiratory failure
Lung cancer is the leading cause of cancer mortality worldwide.[1] Patients with lung cancer often require care in the intensive care unit (ICU) for cancer- or treatment-related complications.[2] Despite recent improvement in the intensive care of patients with lung cancer, the treatment outcome, especially with mechanical ventilator support, remains extremely poor.[3] Therefore, aggressive care for patients with advanced lung cancer is controversial.[4] However, a recent study advocated that ICU trials should include patients with newly diagnosed cancers, but with a life expectancy of less than 1 year, because they may have a chance to recover after cancer treatment.[5]
Erlotinib, a reversible and specific tyrosine kinase inhibitor (TKI), is effective in tumors with gene mutations that activate the epidermal growth factor receptor (EGFR).[6] Previous studies have shown that lung adenocarcinoma among East Asian female never-smokers or former light smokers was associated with a higher probability of having an EGFR mutation.[7,8] About 80% of lung adenocarcinoma from East Asian never-smokers harbored an EGFR kinase mutation.[9,10] Sex, ethnic origin, smoking status, and histologic findings help to identify patients who have a high likelihood of responding to EGFR-TKI treatment.[7]
We recently encountered a patient with extensive lung adenocarcinoma causing respiratory failure. Despite advanced disease, care in the ICU with ventilator support was performed because she was a newly diagnosed patient and EGFR mutation was highly suspected. Empirical erlotinib treatment resulted in an improvement in the disease and allowed ventilator weaning.
Case Report
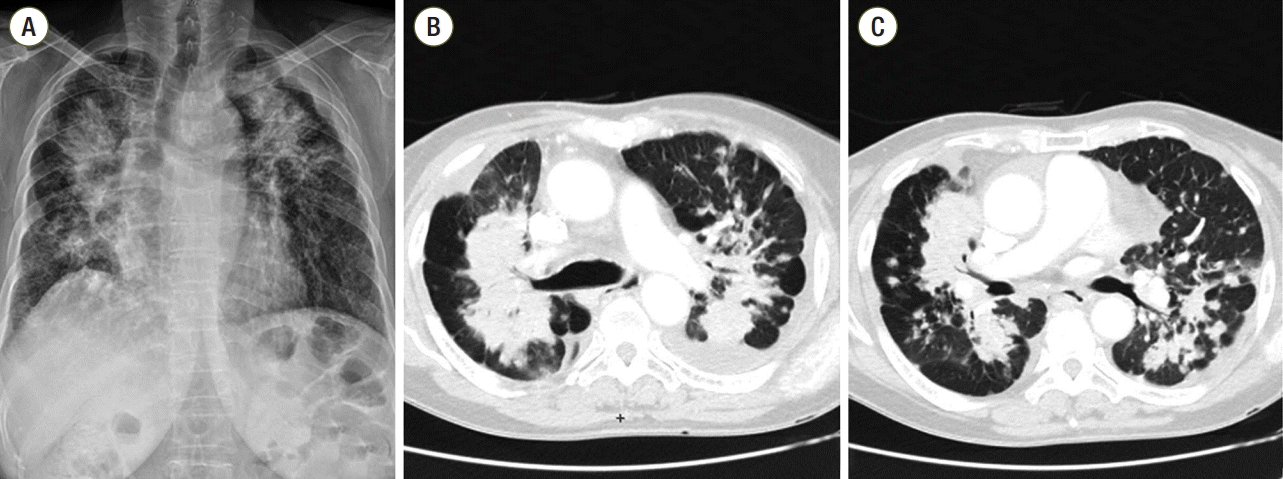
A 70-year-old female never-smoker complained of a nonproductive cough, progressive dyspnea, and headache. She visited another hospital in June 2013. At that time, computed tomography (CT) of the chest revealed a 1.7-cm lobulated nodule in the right middle lobe with multiple small nodules scattered throughout both lungs. However, she refused to have the disease evaluated and was lost to follow-up. Her symptoms deteriorated, and she visited our chest clinic in June 2014 for diagnosis and treatment. Chest radiographs and a CT scan revealed interval progression of the primary mass and extensive lung-to-lung metastases forming a confluent mass in both lungs (Fig. 1A, B and C). Further investigation with positron emission tomography–CT and magnetic resonance imaging of the brain revealed multiple metastases in the liver, bone, and brain. Although a bronchoscopic biopsy was performed, the result was not diagnostic. Because the pneumothorax had developed after the bronchoscopic biopsy, a chest tube was inserted. While evaluations were in progress, her chest radiography findings and oxygenation status gradually worsened. Because the extensive pretreated malignancy caused her respiratory distress, she required urgent evaluation and treatment. Therefore, we performed endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) for a histologic diagnosis despite she had hypoxemia. Because her respiratory distress was aggravated during EBUS-TBNA, transesophageal fine needle aspiration of a subcarinal lymph node using the EBUS scope was performed.[11]
The following day, her respiratory distress worsened; her vital signs showed a blood pressure of 125/75 mmHg, a heart rate of 99 beats per minute, a respiratory rate of 30 cycles per minute, and a body temperature of 36.0°C. Her arterial blood gas analysis revealed the following: pH, 7.214; PaCO2, 83.3 mmHg; PaO2, 63.3 mmHg; HCO3-, 32.9 mmol/L; and SaO2, 85.9%. She was transferred to the ICU for mechanical ventilation. Empirical antibiotics were initiated. Because the rapidly progressive lung cancer was also responsible for respiratory failure and adenocarcinoma was highly suggested by clinical information (never-smoker, Asian, and female), we decided to administer empirical erlotinib (150 mg/day) via a Levin tube. She required a high fraction of inspired oxygen for more than 10 days. Tracheostomy was performed on day 10 of endotracheal intubation. Because her final blood and sputum culture results showed no isolated pathogenic organisms, the antibiotics were stopped. Additionally, there was no evidence for the cause of the respiratory failure, extensive malignancy was considered as the main cause of respiratory failure. Therefore, while the patient was under mechanical ventilation support, erlotinib treatment was continued. Although the EUS-guided biopsy revealed metastatic carcinoma, we were unable to identify the pathologic subtype. Later, the peptide nucleic acid-clamp method confirmed the presence of a deletion in exon 19 of the EGFR gene. She gradually improved and was transferred to a general ward with a mobile ventilator on day 30 of treatment. On day 65 of treatment, she was successfully weaned off the ventilator. Follow-up chest radiography and CT performed on day 90 (Fig. 2A, B and C) and month 9 of treatment (Fig. 3A, B and C), showed a dramatic decrease in the extent of the primary mass and multiple metastatic lesions in the lung. Chest radiography and CT performed at month 18 of treatment showed a slightly increased extent of the disease (Fig. 4A, B and C). However, her symptoms were stable, and she was continuing to take erlotinib at the time of this writing.
Discussion
Patients with newly diagnosed cancer may require ICU admission and immediate chemotherapy to treat acute life-threatening organ failure caused by the cancer. Because immediate treatment of the malignancy is the only way to ensure recovery, these patients must receive immediate anticancer therapy as well as life-sustaining therapies.[12]
We have reported a case of newly diagnosed lung cancer causing respiratory failure. Because the patient’s clinical situation was too serious to wait for the results of pathology and gene mutation analysis, we initiated empirical treatment with an oral EGFR TKI based on clinical information including ethnic origin, sex, and smoking history, and the treatment outcome was very successful. After initiation of treatment, we confirmed the EGFR mutation.
As in this case, a previous report of empirical erlotinib treatment in a patient who presented with respiratory failure secondary to lung adenocarcinoma with a high likelihood of having an EGFR mutation suggested a “shoot first, ask later” strategy.[13] The authors suggested that if a critically ill cancer patient has a chance of recovery, clinicians should not give up and should consider empirical anti-tumor treatment based on the clinical information. This strategy should be limited to patients who cannot wait for EGFR mutation analysis results.
Although we also performed empirical treatment before the diagnostic confirmation, due to our patient’s critical clinical situation, we suggest a more reasonable strategy for these patients. If physicians encounter a lung cancer patient with respiratory failure but with a high probability of harboring the EGFR mutation or the echinoderm microtubule-associated protein-like 4/the anaplastic lymphoma kinase rearrangement, physicians may not be reluctant to provide life support therapy including ventilator support and extracorporeal membrane oxygenation support. When the patient becomes stable, diagnostic test including portable bronchoscopy and biopsy can be performed for pathologic diagnosis or genotyping. Thereafter, the treatment could be individualized for that diagnosis.
However, admitting patients with advanced cancer to the ICU may arouse ethical controversy. In several situations, intensive care for patients with advanced cancer does not ensure the quality of life that they deserve. Therefore, prior to ICU care, we should select appropriate candidates who would benefit from aggressive treatment and provide opportunities to decide their end-of life care with the patient and their families.
We previously described three critically ill patients with advanced lung cancer who required mechanical ventilation for respiratory failure and were successfully treated with ALK inhibitors.[14] While our patient required 62 days to be weaned off the mechanical ventilator, it took 17 to 42 days to wean the patients off the ventilator in previous cases. Although a considerable time was needed in both cases, all patients were successfully treated. These cases suggest that physicians require a new perspective on the use of a molecular targeted agent in the ICU and treatment for lung cancer patients with respiratory failure caused by pretreated lung cancer.
In conclusion, our case shows that respiratory failure induced by extensive lung adenocarcinoma can be successfully reversed by a targeted therapy. Our case suggests that there is a population of patients with newly diagnosed primary lung cancer who are likely to benefit from targeted therapy, although they initially require ICU support.
NOTES
-
No potential conflict of interest relevant to this article was reported.
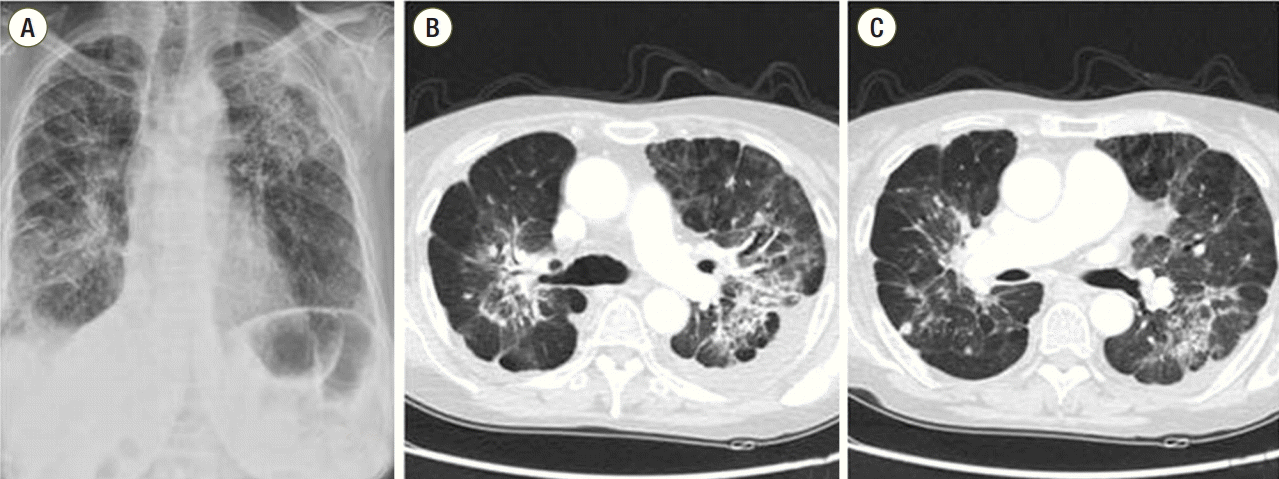
Fig. 1.Chest radiograph (A) and computed tomography scans (B, C) revealed a 3-cm primary mass in the right middle lobe with extensive lung-to-lung metastases forming a confluent mass in both lungs.

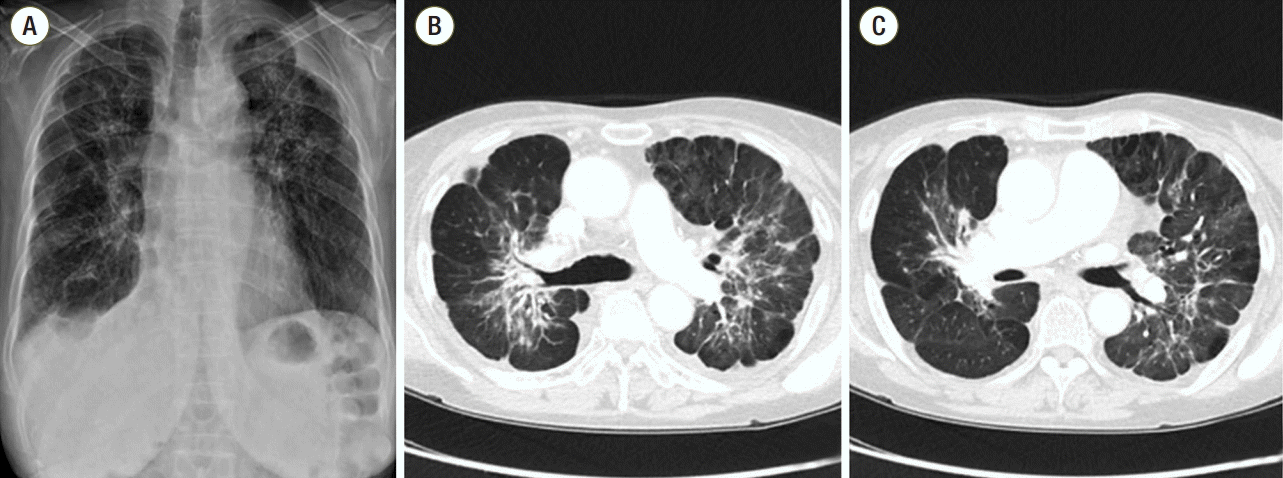
Fig. 2.Chest radiograph (A) and computed tomography scans (B, C) revealed a dramatic decrease in the extent of the primary mass and multiple metastatic lesions in both lungs after 3 months of erlotinib treatment.
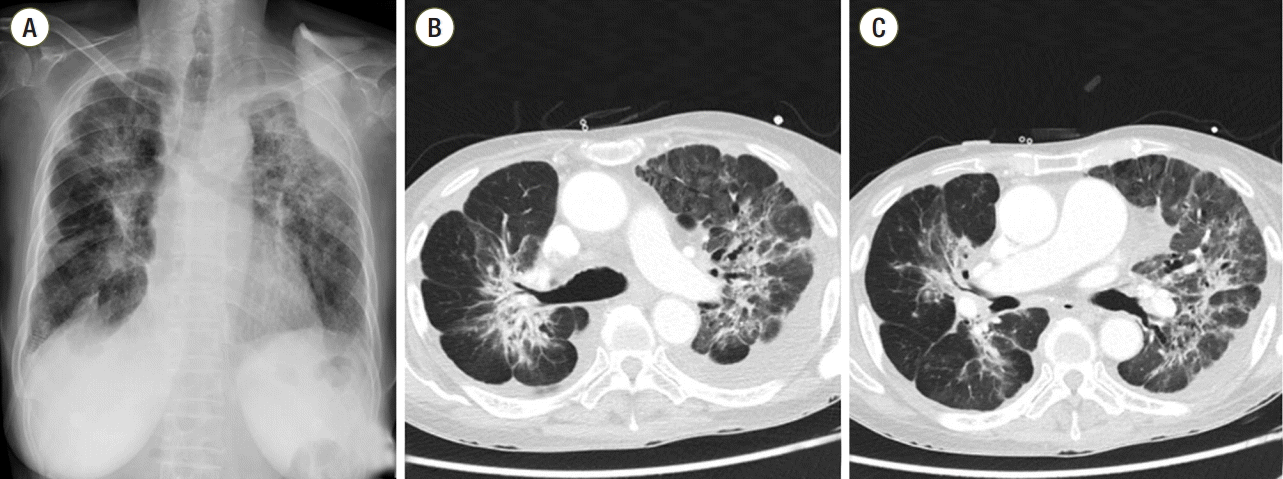
Fig. 3.Chest radiograph (A) and computed tomography scans (B, C) showed an interval decrease in the extent of lung-to-lung metastases in both hemithoraces after 9 months of erlotinib treatment.
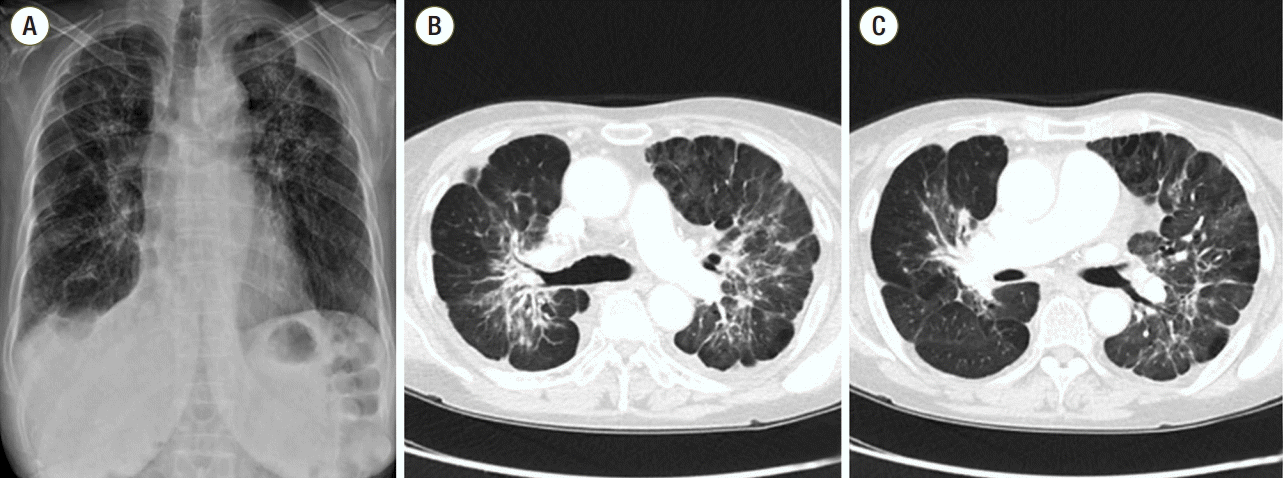
Fig. 4.Chest radiograph (A) and computed tomography scans (B, C) performed after 18 months of treatment showed a slight increase in the extent of the disease.
References
- 1. Siegel RL, Miller KD, Jemal A. Cancer statistics, 2015. CA Cancer J Clin 2015;65:5-29.ArticlePubMed
- 2. Adam AK, Soubani AO. Outcome and prognostic factors of lung cancer patients admitted to the medical intensive care unit. Eur Respir J 2008;31:47-53.ArticlePubMed
- 3. Lin YC, Tsai YH, Huang CC, Hsu KH, Wang SW, Tsao TC, et al. Outcome of lung cancer patients with acute respiratory failure requiring mechanical ventilation. Respir Med 2004;98:43-51.ArticlePubMed
- 4. Soubani AO, Ruckdeschel JC. The outcome of medical intensive care for lung cancer patients: the case for optimism. J Thorac Oncol 2011;6:633-8.ArticlePubMed
- 5. Azoulay E, Soares M, Darmon M, Benoit D, Pastores S, Afessa B. Intensive care of the cancer patient: recent achievements and remaining challenges. Ann Intensive Care 2011;1:5. ArticlePubMedPMC
- 6. Cataldo VD, Gibbons DL, Pérez-Soler R, Quintás-Cardama A. Treatment of non-small-cell lung cancer with erlotinib or gefitinib. N Engl J Med 2011;364:947-55.ArticlePubMed
- 7. Kim ES, Hirsh V, Mok T, Socinski MA, Gervais R, Wu YL, et al. Gefitinib versus docetaxel in previously treated non-small-cell lung cancer (INTEREST): a randomised phase III trial. Lancet 2008;372:1809-18.ArticlePubMed
- 8. Mok TS, Wu YL, Thongprasert S, Yang CH, Chu DT, Saijo N, et al. Gefitinib or carboplatin-paclitaxel in pulmonary adenocarcinoma. N Engl J Med 2009;361:947-57.ArticlePubMed
- 9. Li C, Fang R, Sun Y, Han X, Li F, Gao B, et al. Spectrum of oncogenic driver mutations in lung adenocarcinomas from East Asian never smokers. PLoS One 2011;6:e28204.ArticlePubMedPMC
- 10. Sun Y, Ren Y, Fang Z, Li C, Fang R, Gao B, et al. Lung adenocarcinoma from East Asian never-smokers is a disease largely defined by targetable oncogenic mutant kinases. J Clin Oncol 2010;28:4616-20.ArticlePubMedPMC
- 11. Kim S, Lee J, Hong ME, Do IG, Kang SY, Ha SY, et al. High-throughput sequencing and copy number variation detection using formalin fixed embedded tissue in metastatic gastric cancer. PLoS One 2014;9:e111693.ArticlePubMedPMC
- 12. Darmon M, Thiery G, Ciroldi M, de Miranda S, Galicier L, Raffoux E, et al. Intensive care in patients with newly diagnosed malignancies and a need for cancer chemotherapy. Crit Care Med 2005;33:2488-93.ArticlePubMed
- 13. Bosch-Barrera J, Sais E, Lorencio C, Porta R, Izquierdo A, Menéndez JA, et al. Successful empirical erlotinib treatment of a mechanically ventilated patient newly diagnosed with metastatic lung adenocarcinoma. Lung Cancer 2014;86:102-4.ArticlePubMed
- 14. Ahn HK, Jeon K, Yoo H, Han B, Lee SJ, Park H, et al. Successful treatment with crizotinib in mechanically ventilated patients with ALK positive non-small-cell lung cancer. J Thorac Oncol 2013;8:250-3.ArticlePubMed
Citations
Citations to this article as recorded by

- Lazarus effect in a patient initially empirically treated with osimertinib for EGFR L858R mutant non-small cell lung cancer with leptomeningeal disease: a case report
Shreya Bhatia, Manuel G. Cortez, Spencer Lessans, Wade T. Iams
Oncotarget.2024; 15(1): 27. CrossRef - Lung cancer with superior vena cava syndrome diagnosed by intravascular biopsy using EBUS-TBNA
Daegeun Lee, Seong Mi Moon, Dongwuk Kim, Juwon Kim, Haseong Chang, Bumhee Yang, Suk Hyeon Jeong, Kyung Jong Lee
Respiratory Medicine Case Reports.2016; 19: 177. CrossRef














 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite