Articles
- Page Path
- HOME > Acute Crit Care > Volume 35(3); 2020 > Article
-
Original Article
Nutrition Effectiveness of a multidisciplinary team for nutrition support in a trauma intensive care unit -
Eunsuk Oh1,2
 , Hongjin Shim1,3,4
, Hongjin Shim1,3,4 , Hyon Ju Yon1,5
, Hyon Ju Yon1,5 , Jin Sil Moon6
, Jin Sil Moon6 , Dae Ryong Kang6
, Dae Ryong Kang6 , Ji Young Jang7
, Ji Young Jang7
-
Acute and Critical Care 2020;35(3):142-148.
DOI: https://doi.org/10.4266/acc.2020.00318
Published online: August 19, 2020
1Nutrition Support Team, Wonju Severance Christian Hospital, Wonju, Korea
2Dapartment of Pharmacy, Wonju Severance Christian Hospital, Wonju, Korea
3Department of Surgery, Yonsei University Wonju College of Medicine, Wonju, Korea
4Trauma Center, Wonju Severance Christian Hospital, Wonju, Korea
5Department of Nutrition Services, Wonju Severance Christian Hospital, Wonju, Korea
6Department of Biostatistics, Yonsei University Wonju College of Medicine, Wonju, Korea
7Department of Surgery, National Health Insurance Service Ilsan Hospital, Goyang, Korea
- Corresponding author Ji Young Jang Department of Surgery, National Health Insurance Service Ilsan Hospital, 100 Ilsan-ro, Ilsandong-gu, Goyang 10444, Korea Tel: +82-31-900-0975 Fax: +82-31-900-0138 E-mail: drjangjiyoung@gmail.com
Copyright © 2020 The Korean Society of Critical Care Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background
- We evaluated clinical and nutritional outcomes according to multidisciplinary team involvement in nutrition support in a regional trauma intensive care unit (TICU).
-
Methods
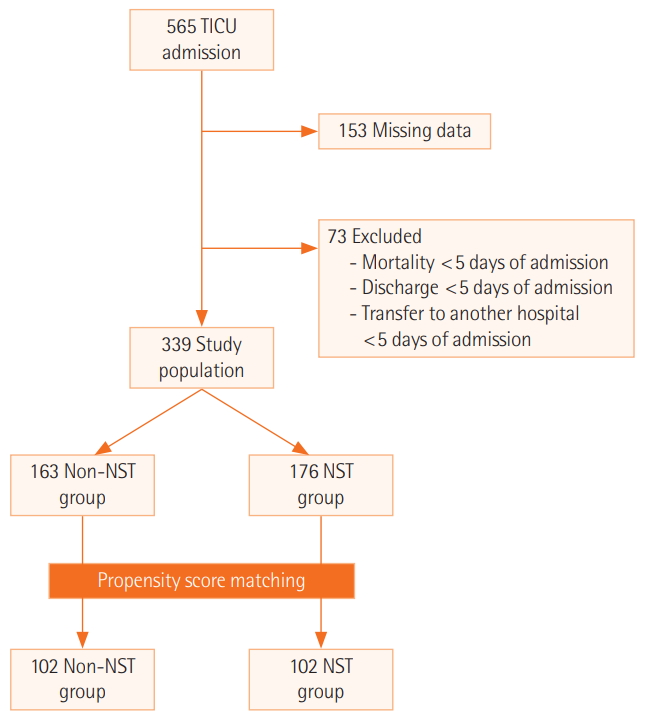
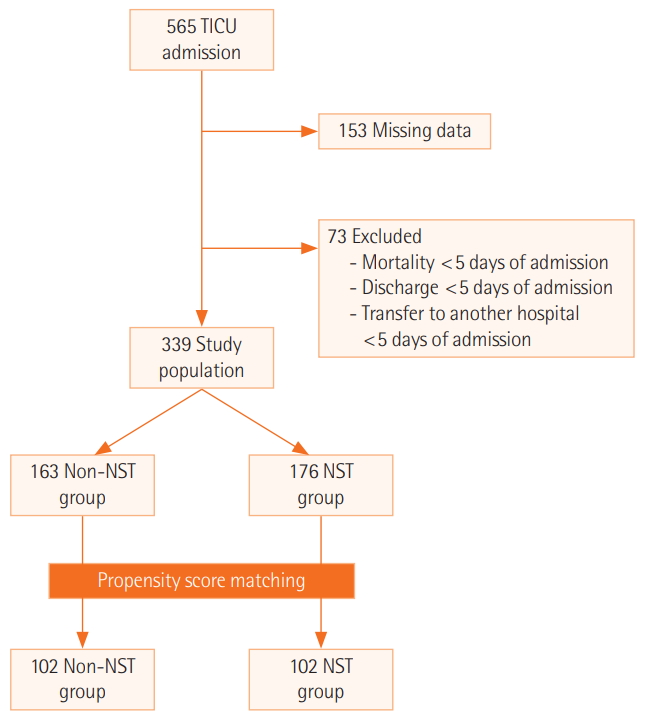
- We retrospectively compared the outcomes for 339 patients admitted to the TICU for >5 days depending on nutrition support team (NST) involvement (n=176) and non-NST involvement (n=163).
-
Results
- The mean age and injury severity score (ISS) were 57.3±16.7 years and 18.6±9.7, respectively. Fifty-three patients (15.6%) had shock on admission and 182 (53.7%) underwent surgery during TICU admission. Some patients were admitted to neurosurgery (46%), general surgery (35.4%), and other (18.6%) departments. There were significant differences in the ISS, Acute Physiology and Chronic Health Evaluation (APACHE) II score, shock on TICU admission, and initial laboratory results. After propensity score matching, the total delivered/required caloric ratio and total delivered/required protein ratio were significantly higher in the NST group than in the non-NST group (calorie: 80.4% vs. 66.7%, P=0.007; protein: 93.1% vs. 68.3%, P<0.001). The NST group had an adequate protein supply more frequently than the non-NST group (protein: 48.0% vs. 25.8%, P=0.002). There was no significant difference in survival, even after adjustment for risk factors using Cox proportional hazard analysis.
-
Conclusions
- The results of our study suggest that multidisciplinary team involvement in nutrition support in TICU patients may improve nutritional, but not clinical, outcomes.
INTRODUCTION
MATERIALS AND METHODS
RESULTS
DISCUSSION
KEY MESSAGES
-
CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
Conceptualization: EO, HS, JYJ. Data curation: EO, HJY, JYJ. Formal analysis: JSM, DRK, JYJ. Methodology: EO, HS, DRK, JYJ. Project administration: HS, JYJ. Visualization: JSM, JYJ. Writing–original draft: EO, JYJ. Writing–review & editing: all authors.
NOTES
| Variable | Total (n=339) | Non-NST (n=163) | NST (n=176) | P-value |
|---|---|---|---|---|
| Age (yr) | 57.3±16.7 | 56.3±16.9 | 58.2±16.4 | 0.297 |
| Male sex | 267 (78.8) | 38 (23.3) | 34 (19.3) | 0.369 |
| ISS | 18.6±9.7 | 16.2±9.1 | 20.8±9.6 | <0.001 |
| APACHE II score | 13.3±6.9 | 12.0±6.4 | 14.6±7.2 | <0.001 |
| Shock at the time of TICU admission | 53 (15.6) | 17 (10.4) | 36 (20.5) | 0.011 |
| Surgery during TICU admission | 182 (53.7) | 77 (47.2) | 105 (59.7) | 0.022 |
| Initial hemoglobin (g/dl) | 11.9±2.1 | 12.3±2.2 | 11.6±1.9 | 0.002 |
| Initial serum albumin (g/dl) | 3.4±0.7 | 3.5±0.6 | 3.3±0.7 | 0.041 |
| Admission department | 0.098 | |||
| Neurosurgery | 156 (46.0) | 67 (41.1) | 89 (50.6) | |
| General surgery | 120 (35.4) | 67 (41.1) | 53 (30.1) | |
| Other | 63 (18.6) | 29 (17.8) | 34 (19.3) | |
| Weight (kg) | 66.4±12.0 | 66.5±11.8 | 66.2±12.2 | 0.821 |
| Height (cm) | 166.9±8.8 | 166.6±8.8 | 167.0±8.9 | 0.702 |
| BMI (kg/m2) | 23.7±3.3 | 23.9±3.5 | 23.6±3.2 | 0.499 |
| Timing of nutrition start (day) | 2.4±1.8 | 2.4±1.6 | 2.3±2.1 | 0.796 |
| Initial nutrition route | <0.001 | |||
| PN | 279 (82.3) | 120 (73.6) | 159 (90.3) | |
| Oral | 44 (13.6) | 35 (21.5) | 11 (6.3) | |
| Tube feeding | 5 (1.5) | 1 (0.6) | 4 (2.3) | |
| Mixed | 11 (3.2) | 6 (3.7) | 4 (2.3) | |
| Calculated calorie requirement (kcal) | 1,516±202 | 1,534±205 | 1,501±200 | 0.143 |
| Calculated protein requirement (g) | 74.5±11.7 | 74.5±10.9 | 74.6±12.3 | 0.897 |
| Total delivered/required caloric ratio in TICU (%) | 80.4±38.7 | 64.1±36.3 | 93.8±35.5 | <0.001 |
| Total delivered/required protein ratio in TICU (%) | 88.8±51.0 | 65.5±49.5 | 108.1±43.7 | <0.001 |
| Adequate energy supply | 118 (36.9) | 39 (27.1) | 79 (44.9) | 0.001 |
| Adequate protein supply | 102 (31.8) | 36 (24.8) | 66 (37.5) | 0.015 |
| Duration of TICU admission (day) | 10.4±12.4 | 5.5±4.8 | 14.9±15.3 | <0.001 |
| Duration of hospitalization (day) | 24 (6–86)a | 22.6±15.7 | 34.5±20.8 | <0.001 |
| ICU mortality | 29 (8.6) | 6 (6.3) | 23 (21.5) | 0.002 |
| Overall mortality | 32 (9.4) | 7 (4.3) | 25 (14.2) | 0.002 |
Values are presented as mean±standard deviation or number (%).
NST: nutrition support team; ISS: injury severity score; APACHE: Acute Physiology and Chronic Health Evaluation; TICU: trauma intensive care unit; BMI: body mass index; PN: parenteral nutrition; ICU: intensive care unit.
a Median (range).
| Variable |
Overall mortality |
|
|---|---|---|
| HR (95% CI) | P-value | |
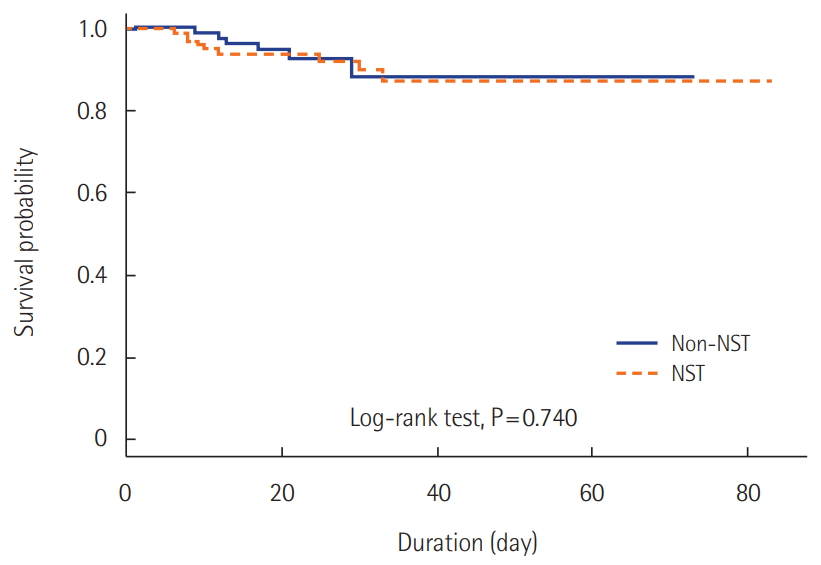
| Crude model | 1.19 (0.42–3.40) | 0.740 |
| Adjusted model | 2.11 (0.66–6.78) | 0.211 |
- 1. Edington J, Boorman J, Durrant ER, Perkins A, Giffin CV, James R, et al. Prevalence of malnutrition on admission to four hospitals in England. The Malnutrition Prevalence Group. Clin Nutr 2000;19:191-5.ArticlePubMed
- 2. Bruun LI, Bosaeus I, Bergstad I, Nygaard K. Prevalence of malnutrition in surgical patients: evaluation of nutritional support and documentation. Clin Nutr 1999;18:141-7.ArticlePubMed
- 3. Correia MI, Waitzberg DL. The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr 2003;22:235-9.ArticlePubMed
- 4. Mogensen KM, Robinson MK, Casey JD, Gunasekera NS, Moromizato T, Rawn JD, et al. Nutritional Status and mortality in the critically ill. Crit Care Med 2015;43:2605-15.ArticlePubMed
- 5. Alberda C, Gramlich L, Jones N, Jeejeebhoy K, Day AG, Dhaliwal R, et al. The relationship between nutritional intake and clinical outcomes in critically ill patients: results of an international multicenter observational study. Intensive Care Med 2009;35:1728-37.ArticlePubMedPDF
- 6. Lee JS, Kang JE, Park SH, Jin HK, Jang SM, Kim SA, et al. Nutrition and clinical outcomes of nutrition support in multidisciplinary team for critically ill patients. Nutr Clin Pract 2018;33:633-9.ArticlePubMed
- 7. Doig GS, Heighes PT, Simpson F, Sweetman EA. Early enteral nutrition reduces mortality in trauma patients requiring intensive care: a meta-analysis of randomised controlled trials. Injury 2011;42:50-6.ArticlePubMed
- 8. Dissanaike S, Pham T, Shalhub S, Warner K, Hennessy L, Moore EE, et al. Effect of immediate enteral feeding on trauma patients with an open abdomen: protection from nosocomial infections. J Am Coll Surg 2008;207:690-7.ArticlePubMed
- 9. Wang X, Dong Y, Han X, Qi XQ, Huang CG, Hou LJ. Nutritional support for patients sustaining traumatic brain injury: a systematic review and meta-analysis of prospective studies. PLoS One 2013;8:e58838.ArticlePubMedPMC
- 10. Wasiak J, Cleland H, Jeffery R. Early versus delayed enteral nutrition support for burn injuries. Cochrane Database Syst Rev 2006;(3):CD005489. ArticlePubMed
- 11. Wade CE, Kozar RA, Dyer CB, Bulger EM, Mourtzakis M, Heyland DK. Evaluation of nutrition deficits in adult and elderly trauma patients. JPEN J Parenter Enteral Nutr 2015;39:449-55.ArticlePubMed
- 12. Jang JY, Shim H, Kwon HY, Chung H, Jung PY, Kim S, et al. Improvement of outcomes in patients with pelvic fractures and hemodynamic instability after the establishment of a Korean regional trauma center. Eur J Trauma Emerg Surg 2019;45:107-13.ArticlePubMedPDF
- 13. Kudsk KA, Croce MA, Fabian TC, Minard G, Tolley EA, Poret HA, et al. Enteral versus parenteral feeding. Effects on septic morbidity after blunt and penetrating abdominal trauma. Ann Surg 1992;215:503-11.ArticlePubMedPMC
- 14. Moore FA, Feliciano DV, Andrassy RJ, McArdle AH, Booth FV, Morgenstein-Wagner TB, et al. Early enteral feeding, compared with parenteral, reduces postoperative septic complications: the results of a meta-analysis. Ann Surg 1992;216:172-83.ArticlePubMedPMC
- 15. Rhee P, Hadjizacharia P, Trankiem C, Chan L, Salim A, Brown C, et al. What happened to total parenteral nutrition? The disappearance of its use in a trauma intensive care unit. J Trauma 2007;63:1215-22.ArticlePubMed
- 16. Plurad D, Green D, Inaba K, Belzberg H, Demetriades D, Rhee P. A 6-year review of total parenteral nutrition use and association with late-onset acute respiratory distress syndrome among ventilated trauma victims. Injury 2009;40:511-5.ArticlePubMed
- 17. Lee SH, Jang JY, Kim HW, Jung MJ, Lee JG. Effects of early enteral nutrition on patients after emergency gastrointestinal surgery: a propensity score matching analysis. Medicine (Baltimore) 2014;93:e323.ArticlePubMedPMC
- 18. Jeong HS, Teong CH, Kim WJ, Lee AR. Attitudes of medical staff and factors related to nutritional support for patient care in a university hospital. J Clin Nutr 2014;6:37-41.ArticlePDF
- 19. Practice guidelines for preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures: an updated report by the American Society of Anesthesiologists task force on preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration. Anesthesiology 2017;126:376-93.PubMed
- 20. Smith I, Kranke P, Murat I, Smith A, O’Sullivan G, Søreide E, et al. Perioperative fasting in adults and children: guidelines from the European Society of Anaesthesiology. Eur J Anaesthesiol 2011;28:556-69.ArticlePubMed
- 21. DeChicco R, Neal T, Guardino JM. Developing an education program for nutrition support teams. Nutr Clin Pract 2010;25:481-9.ArticlePubMed
References
Figure & Data
References
Citations

- Impact of a multidisciplinary collaborative nutritional treatment model in patients who are critically ill with neurological disorders: A randomized controlled trial
Bao-Di Gu, Yun Wang, Rong Ding
Technology and Health Care.2024; 32(3): 1767. CrossRef - Implementation of a multidisciplinary nutritional support team and clinical outcomes in critically ill patients with COVID-19
In-Ae Song, Kyunghwa Lee, Sunghee Lee, Keonhee Kim, Tak Kyu Oh
Clinical Nutrition.2024; 43(2): 315. CrossRef - Nutrition support teams: Institution, evolution, and innovation
Albert Barrocas, Denise Baird Schwartz, Bruce R. Bistrian, Peggi Guenter, Charles Mueller, Ronni Chernoff, Jeanette M. Hasse
Nutrition in Clinical Practice.2023; 38(1): 10. CrossRef - Multidisciplinary Difficult Airway Team Characteristics, Airway Securement Success, and Clinical Outcomes: A Systematic Review
Vinciya Pandian, Talha U. Ghazi, Marielle Qiaoshu He, Ergest Isak, Abdulmalik Saleem, Lindsay R. Semler, Emily C. Capellari, Michael J. Brenner
Annals of Otology, Rhinology & Laryngology.2023; 132(8): 938. CrossRef - Nutrition Therapy by Nutrition Support Team: A Comparison of Multi-Chamber Bag and Customized Parenteral Nutrition in Hospitalized Patients
Seunghyun Cheon, Sang-Hyeon Oh, Jung-Tae Kim, Han-Gon Choi, Hyojung Park, Jee-Eun Chung
Nutrients.2023; 15(11): 2531. CrossRef - Consultation pattern changes of parenteral nutrition with a multidisciplinary nutrition support team in a recently opened hospital in Korea: a retrospective cohort study
Kyoung Won Yoon, Hyo Jin Kim, Yujeong Im, Seul Gi Nam, Joo Yeon Lee, Hyo Gee Lee, Joong-Min Park
Annals of Clinical Nutrition and Metabolism.2023; 15(2): 57. CrossRef - Lipid emulsion treatment of cardiotoxicity caused by calcium channel blocker and beta-blocker
Ju-Tae Sohn
The American Journal of Emergency Medicine.2022; 58: 331. CrossRef - Physician Compliance with Nutrition Support Team Recommendations: Effects on the Outcome of Treatment for Critically Ill Patients
Hyon-Ju Yon, Eun-Suk Oh, Ji Young Jang, Ji Yun Jang, Hongjin Shim
Journal of Acute Care Surgery.2022; 12(1): 1. CrossRef - Nutritional Status of Intensive Care Unit Patients According to the Referral to the Nutrition Support Team and Compliance with the Recommendations
Yunjin Sohn, Taisun Hyun
Korean Journal of Community Nutrition.2022; 27(2): 121. CrossRef - Lipid emulsion dosage used for resuscitation after drug toxicity
Ju-Tae Sohn
The American Journal of Emergency Medicine.2022; 59: 168. CrossRef - Intensive care management of traumatic brain injury: How can mnemonics help?
Biljana Damnjanović, Jovana Stanisavljević, Adi Hadžibegović, Ivan Rović, Đuro Šijan, Nemanja Jovanović, Sanja Ratković, Marija Milenković
Serbian Journal of Anesthesia and Intensive Therapy.2022; 44(5-6): 105. CrossRef - 救急・集中治療領域 重症患者における栄養管理
信人 中西, 穣治 小谷
The Japanese Journal of SURGICAL METABOLISM and NUTRITION.2022; 56(6): 229. CrossRef - Urinary Titin N-Fragment as a Biomarker of Muscle Atrophy, Intensive Care Unit-Acquired Weakness, and Possible Application for Post-Intensive Care Syndrome
Nobuto Nakanishi, Rie Tsutsumi, Kanako Hara, Masafumi Matsuo, Hiroshi Sakaue, Jun Oto
Journal of Clinical Medicine.2021; 10(4): 614. CrossRef - Lack of evidence for a nutritional support team in a trauma intensive care unit?
Jae Hwa Cho
Acute and Critical Care.2020; 35(3): 205. CrossRef
- Figure
- Related articles
-
- Corrigendum to: Development of a deep learning model for predicting critical events in a pediatric intensive care unit
- Development of a deep learning model for predicting critical events in a pediatric intensive care unit
- Radiomic analysis of abdominal organs during sepsis of digestive origin in a French intensive care unit
- Digital tomography in the diagnosis of a posterior pneumothorax in the intensive care unit

 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite