Articles
- Page Path
- HOME > Acute Crit Care > Volume 35(4); 2020 > Article
-
Original Article
Epidemiology Postextubation respiratory events in patients admitted to the intensive care unit: a prospective pilot study using overnight respiratory polygraphy -
Ye Jin Lee1
 , Jinwoo Lee2,3
, Jinwoo Lee2,3 , Sang-Min Lee2,3
, Sang-Min Lee2,3 , Jaeyoung Cho2
, Jaeyoung Cho2
-
Acute and Critical Care 2020;35(4):271-278.
DOI: https://doi.org/10.4266/acc.2020.00479
Published online: November 12, 2020
1Division of Pulmonary, Allergy and Critical Care Medicine, Department of Internal Medicine, Kangdong Sacred Heart Hospital, Seoul, Korea
2Division of Pulmonary and Critical Care Medicine, Department of Internal Medicine, Seoul National University Hospital, Seoul, Korea
3Department of Internal Medicine, Seoul National University College of Medicine, Seoul, Korea
- Corresponding author Jaeyoung Cho Division of Pulmonary and Critical Care Medicine, Department of Internal Medicine, Seoul National University Hospital, 101 Daehak-ro, Jongno-gu, Seoul 03080, Korea Tel: +82-2-2072-2503 Fax: +82-2-762-9662 E-mail: apricot6@snu.ac.kr
Copyright © 2020 The Korean Society of Critical Care Medicine
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
-
Background
- Before the main trial in which respiratory polygraphy will be used to evaluate postextubation sleep apnea in critically ill patients, we performed a prospective pilot study to ensure that any issues with the conduct of the trial would be identified.
-
Methods
- In the present study, 13 adult patients who had received mechanical ventilation for ≥24 hours were prospectively recruited. Among the patients, 10 successfully completed respiratory polygraphy on the first or second night after extubation. Data regarding the types and doses of corticosteroids, analgesics, sedatives, and muscle relaxants as well as the methods of oxygen delivery were recorded.
-
Results
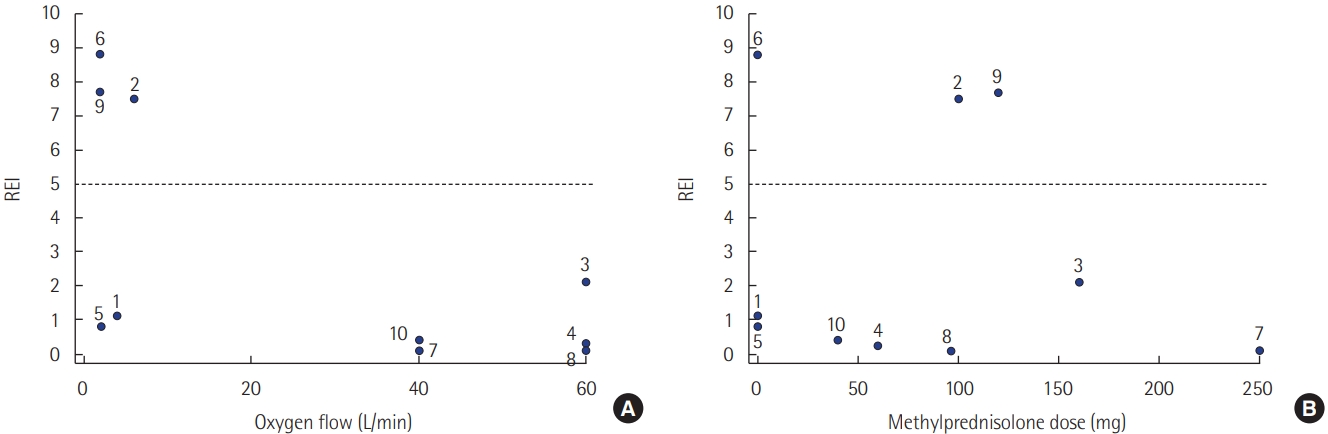
- During the night of respiratory polygraphy, all 10 patients received supplemental oxygen (low-flow oxygen, n=5; high-flow oxygen, n=5), and seven patients received intravenous corticosteroids. Three of the 10 patients had a respiratory event index (REI) ≥5/hr. All respiratory events were obstructive episodes. None of the patients receiving high-flow oxygen therapy had an REI ≥5/hr. Two of the seven patients who received corticosteroids and one of the other three patients who did not receive this medication had an REI ≥5/hr. Although low- or high-flow oxygen therapy was provided, all patients had episodes of oxygen saturation (SpO2) <90%. Two of the three patients with an REI ≥5/hr underwent in-laboratory polysomnography. The patients’ Apnea-Hypopnea Index and REI obtained via polysomnography and respiratory polygraphy, respectively, were similar.
-
Conclusions
- In a future trial to evaluate postextubation sleep apnea in critically ill patients, pre-stratification based on the use of corticosteroids and high-flow oxygen therapy should be considered.
INTRODUCTION
MATERIALS AND METHODS
RESULTS
DISCUSSION
KEY MESSAGES
-
CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
Conceptualization: JL, JC. Data curation: YJL. Formal analysis: YJL. Methodology: YJL, SML, JL. Project administration: SML, JL. Visualization: YJL. Writing–original draft: YJL. Writing–review and editing: JC, SML, JL.
NOTES
SUPPLEMENTARY MATERIALS
Supplementary Table 1.
| Patient no. | Age (yr) | Sex | BMI (kg/m2) |
Symptom |
Neck circumference (cm) | STOP-Bang score | Comorbidity | APACHE II score | Duration of mechanical ventilation (day) | Reason for mechanical ventilation | In-hospital outcome | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| EDS | Nonrestorative sleep | Fatigue | Insomnia | Snoring | Witnessed apnea | |||||||||||
| 1a | 77 | M | 21.7 | - | - | - | - | - | - | - | - | HTN, DM, multiple myeloma | 35 | 7 | Sepsis | Died 14 days after ICU discharge |
| 2 | 56 | F | 21.7 | No | Yes | Yes | No | Yes | No | 37.0 | 2 | DM, post-lung TPL | 21 | 2 | Pneumonia | Survived |
| 3 | 58 | M | 26.2 | No | Yes | Yes | No | No | No | 39.0 | 3 | Sarcoma | 22 | 8 | Pneumonia | Survived |
| 4 | 80 | M | 27.4 | No | No | No | No | No | No | 42.0 | 3 | DM, CHF, CVD, AF, lung cancer | 13 | 6 | Pneumonia | Survived |
| 5 | 67 | M | 20.8 | No | No | Yes | Yes | No | No | 38.5 | 3 | CHF, AF, COPD, LC | 25 | 6 | CHF | Survived |
| 6 | 83 | M | 14.3 | No | No | No | No | No | No | 38.0 | 2 | NTM-PD | 18 | 4 | Pneumonia | Died 237 days after ICU discharge |
| 7 | 70 | M | 28.7 | No | Yes | Yes | No | Yes | Yes | 43.0 | 6 | Post-lung TPL | 15 | 3 | Post-lung TPL | Survived |
| 8 | 75 | M | 25.5 | No | No | No | No | No | No | 45.0 | 3 | IPF, vasculitis | 35 | 8 | Pneumonia | Died 13 days after ICU discharge |
| 9 | 69 | F | 24.9 | Yes | Yes | Yes | Yes | Yes | Yes | 40.0 | 5 | OSA, asthma | 20 | 5 | Acute exacerbation of asthma | Survived |
| 10 | 74 | M | 22.5 | Yes | Yes | Yes | No | No | No | 38.0 | 3 | Asthma, COPD, CKD, leiomyosarcoma | 30 | 3 | Pneumonia | Died 19 days after ICU discharge |
BMI: body mass index; EDS: excessive daytime sleepiness; STOP-Bang: snoring, tiredness, observed apnea, high blood pressure, body mass index, age, neck circumference, and gender; APACHE: Acute Physiology and Chronic Health Evaluation; HTN: hypertension; DM: diabetes mellitus; ICU: intensive care unit; TPL: transplantation; CHF: congestive heart failure; CVD: cardiovascular disease; AF: atrial fibrillation; COPD: chronic obstructive pulmonary disease; LC: liver cirrhosis; NTM-PD: nontuberculous mycobacterial pulmonary disease; IPF: idiopathic pulmonary fibrosis; OSA: obstructive sleep apnea; CKD: chronic kidney disease.
a Patient 1 had missing data regarding symptoms, neck circumference, and STOP-Bang score.
| Variable | All patients (n=10) | Patient with an REI <5/hr (n=7) | Patient with an REI ≥5/hr (n=3) |
|---|---|---|---|
| Age (yr) | 72 (67–77) | 74 (67–77) | 69 (56–83) |
| Male sex | 8 (80) | 7 (100) | 1 (33) |
| BMI (kg/m2) | 23.7 (21.7–26.2) | 25.5 (21.7–27.4) | 21.7 (14.3–24.9) |
| Neck circumference (cm)a | 39 (38–42) | 41 (39–43) | 38 (37–40) |
| STOP-Bang score ≥3a | 7 (70) | 6 (86) | 1 (33) |
| Charlson comorbidity index | 5 (3–8) | 6 (5–8) | 2 (0–3) |
| Hypertension | 1 (10) | 1 (14) | 0 |
| Diabetes | 3 (30) | 2 (29) | 1 (33) |
| Congestive heart failure | 2 (20) | 2 (29) | 0 |
| COPD | 2 (20) | 2 (29) | 0 |
| APACHE II score | 22 (18–30) | 25 (15–35) | 20 (18–21) |
| SOFA score | 6 (5–10) | 9 (4–10) | 5 (5–7) |
| SAPS II | 48 (32–66) | 54 (32–68) | 46 (30–50) |
| Failure during the first intubation attempt | 4 (40) | 3 (43) | 1 (33) |
| Internal diameter of the endotracheal tubes (mm) | 7.5 (7.5–7.5) | 7.5 (7.5–7.5) | 7.5 (7.0–7.5) |
| Duration of mechanical ventilation (day) | 6 (3–7) | 6 (3–8) | 4 (2–5) |
| Reason for mechanical ventilation | |||
| Pneumonia | 6 (60) | 4 (57) | 2 (67) |
| Acute exacerbation of asthma | 1 (10) | 0 | 1 (33) |
| Heart failure | 1 (10) | 1 (14) | 0 |
| Sepsis | 1 (10) | 1 (14) | 0 |
| Post-lung transplantation | 1 (10) | 1 (14) | 0 |
| Total drug equivalent dose administered 48 hours prior to extubation | |||
| Remifentanyl (mg) | 7.4 (4.2–10.6) | 9.6 (4.2–22.1) | 4.8 (1.8–9.6) |
| Propofol (mg) | 0 (0–1,344) | 0 (0–1,728) | 0 (0–1,344) |
| Dexmedetomidine (mg) | 1.1 (0.04–3.0) | 0.8 (0.04–3.6) | 1.5 (0–3.0) |
| Methylprednisolone (mg) | 78 (0–120) | 60 (0–160) | 100 (0–120) |
| Method of oxygen delivery during the night of respiratory polygraphy | |||
| Low-flow oxygen therapy via nasal prong | 5 (50) | 2 (29) | 3 (100) |
| High-flow nasal cannula | 5 (50) | 5 (71) | 0 |
| FiO2 | 0.4 (0.3–0.5) | 0.4 (0.4–0.6) | 0.3 (0.3–0.4) |
| Flow (L/min) | 23 (2–60) | 40 (4–60) | 2 (2–6) |
Values are presented as median (interquartile range) or number (%).
REI: respiratory event index; BMI: body mass index; STOP-Bang: snoring, tiredness, observed apnea, high blood pressure, body mass index, age, neck circumference, and gender; COPD: chronic obstructive pulmonary disease; APACHE: Acute Physiology and Chronic Health Evaluation; SOFA: Sequential Organ Failure Assessment; SAPS: Simplified Acute Physiology Score; FiO2: fraction of inspired oxygen.
a Patient 1 had missing data regarding neck circumference and STOP-Bang score.
| Patient no. |
Total drug equivalent dose administered 48 hours prior to extubation |
Method of oxygen delivery during the night of respiratory polygraphy |
REI (/hr) | Mean SpO2 (%) | Lowest SpO2 (%) | Time spent (%) with SpO2 <90% | ODI (/hr) | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Remifentanyl (mg) | Propofol (mg) | Dexmedetomidine (mg) | Methylprednisolone (mg)a | Device | Flow rate (L/min) | FiO2 of HFNC | ||||||
| 1 | 5.3 | 0 | 2.9 | 0 | Low-flow via nasal prong | 4 | – | 1.1 | 92 | 83 | 5.9 | 3.5 |
| 2 | 1.8 | 0 | 3.0 | 100 | Low-flow via nasal prong | 6 | – | 7.5 | 97 | 74 | 1.0 | 8.1 |
| 3 | 10.6 | 0 | 0.7 | 160 | HFNC | 60 | 0.6 | 2.1 | 93 | 85 | 1.5 | 2.0 |
| 4 | 9.6 | 0 | 2.0 | 60 | HFNC | 60 | 0.4 | 0.3 | 93 | 86 | 4.4 | 0.3 |
| 5 | 2.0 | 0 | 0.04 | 0 | Low-flow via nasal prong | 2 | – | 0.8 | 98 | 86 | 0.2 | 1.8 |
| 6 | 4.8 | 0 | 1.5 | 0 | Low-flow via nasal prong | 2 | – | 8.8 | 97 | 87 | 0.3 | 5.0 |
| 7 | 22.1 | 4,722 | 0.8 | 250 | HFNC | 40 | 0.4 | 0.1 | 93 | 87 | 1.8 | 0.1 |
| 8 | 26.4 | 0 | 3.6 | 96 | HFNC | 60 | 0.5 | 0.1 | 94 | 88 | 0.2 | 0.3 |
| 9 | 9.6 | 1,344 | 0 | 120 | Low-flow via nasal prong | 2 | – | 7.7 | 92 | 75 | 13.3 | 14.7 |
| 10 | 4.2 | 1,728 | 0 | 40 | HFNC | 40 | 0.6 | 0.4 | 90.8 | 82 | 19.4 | 1.5 |
FiO2: fraction of inspired oxygen; HFNC: high-flow nasal cannula; REI: respiratory event index; SpO2: oxygen saturation; ODI: oxygen desaturation index.
a Six of the seven patients who were treated with corticosteroids received methylprednisolone intravenously. Patient 10 received 50 mg hydrocortisone intravenously four times for 48 hours prior to extubation. Five of the seven patients who received corticosteroids were treated with long-term corticosteroid therapy. The remaining two patients, patients 4 and 10, were treated with corticosteroids for 15 days and 2 days, respectively.
- 1. Senaratna CV, Perret JL, Lodge CJ, Lowe AJ, Campbell BE, Matheson MC, et al. Prevalence of obstructive sleep apnea in the general population: a systematic review. Sleep Med Rev 2017;34:70-81.ArticlePubMed
- 2. Kryger MH, Roth T, Dement WC. Principles and practice of sleep medicine. Philadelphia, Elsevier. 2016.
- 3. Leger D, Bayon V, Laaban JP, Philip P. Impact of sleep apnea on economics. Sleep Med Rev 2012;16:455-62.ArticlePubMed
- 4. Young T, Finn L, Peppard PE, Szklo-Coxe M, Austin D, Nieto FJ, et al. Sleep disordered breathing and mortality: eighteen-year follow-up of the Wisconsin sleep cohort. Sleep 2008;31:1071-8.PubMedPMC
- 5. Jean RE, Gibson CD, Jean RA, Ochieng P. Obstructive sleep apnea and acute respiratory failure: an analysis of mortality risk in patients with pneumonia requiring invasive mechanical ventilation. J Crit Care 2015;30:778-83.ArticlePubMed
- 6. Bolona E, Hahn PY, Afessa B. Intensive care unit and hospital mortality in patients with obstructive sleep apnea. J Crit Care 2015;30:178-80.ArticlePubMed
- 7. Thille AW, Córdoba-Izquierdo A, Maitre B, Boyer L, Brochard L, Drouot X. High prevalence of sleep apnea syndrome in patients admitted to ICU for acute hypercapnic respiratory failure: a preliminary study. Intensive Care Med 2018;44:267-9.ArticlePubMed
- 8. Timm FP, Zaremba S, Grabitz SD, Farhan HN, Zaremba S, Siliski E, et al. Effects of opioids given to facilitate mechanical ventilation on sleep apnea after extubation in the intensive care unit. Sleep 2018;41.Article
- 9. Bergeron C, Kimoff J, Hamid Q. Obstructive sleep apnea syndrome and inflammation. J Allergy Clin Immunol 2005;116:1393-6.ArticlePubMed
- 10. Vicente E, Marin JM, Carrizo SJ, Osuna CS, González R, Marin-Oto M, et al. Upper airway and systemic inflammation in obstructive sleep apnoea. Eur Respir J 2016;48:1108-17.ArticlePubMed
- 11. Ogna A, Forni Ogna V, Mihalache A, Pruijm M, Halabi G, Phan O, et al. Obstructive sleep apnea severity and overnight body fluid shift before and after hemodialysis. Clin J Am Soc Nephrol 2015;10:1002-10.ArticlePubMedPMC
- 12. Montandon G, Qin W, Liu H, Ren J, Greer JJ, Horner RL. Pre-Botzinger complex neurokinin-1 receptor-expressing neurons mediate opioid-induced respiratory depression. J Neurosci 2011;31:1292-301.ArticlePubMedPMC
- 13. Jordan AS, McSharry DG, Malhotra A. Adult obstructive sleep apnoea. Lancet 2014;383:736-47.ArticlePubMed
- 14. Berry RB, Brooks R, Gamaldo C, Harding SM, Lloyd RM, Quan SF, et al. AASM scoring manual updates for 2017 (version 2.4). J Clin Sleep Med 2017;13:665-6.ArticlePubMedPMC
- 15. Chishti A, Batchelor AM, Bullock RE, Fulton B, Gascoigne AD, Baudouin SV. Sleep-related breathing disorders following discharge from intensive care. Intensive Care Med 2000;26:426-33.ArticlePubMed
- 16. Chung F, Liao P, Elsaid H, Shapiro CM, Kang W. Factors associated with postoperative exacerbation of sleep-disordered breathing. Anesthesiology 2014;120:299-311.ArticlePubMed
- 17. Tan HL, Gozal D, Ramirez HM, Bandla HP, Kheirandish-Gozal L. Overnight polysomnography versus respiratory polygraphy in the diagnosis of pediatric obstructive sleep apnea. Sleep 2014;37:255-60.ArticlePubMedPMC
- 18. Bianchi MT, Goparaju B. Potential underestimation of sleep apnea severity by at-home kits: rescoring in-laboratory polysomnography without sleep staging. J Clin Sleep Med 2017;13:551-5.ArticlePubMedPMC
- 19. Kuriyama A, Umakoshi N, Sun R. Prophylactic corticosteroids for prevention of postextubation stridor and reintubation in adults: a systematic review and meta-analysis. Chest 2017;151:1002-10.ArticlePubMed
- 20. Prajapat B, Sandhya AS, Chaudhry D, Esquinas AM. Opioids in intensive care unit (ICU): causal agent for sleep apnea, unmasking the undiagnosed sleep apnea or both in the ICU. Sleep 2018;41:zsy081. Article
- 21. McGinley B, Halbower A, Schwartz AR, Smith PL, Patil SP, Schneider H. Effect of a high-flow open nasal cannula system on obstructive sleep apnea in children. Pediatrics 2009;124:179-88.ArticlePubMedPMC
- 22. McGinley BM, Patil SP, Kirkness JP, Smith PL, Schwartz AR, Schneider H. A nasal cannula can be used to treat obstructive sleep apnea. Am J Respir Crit Care Med 2007;176:194-200.ArticlePubMedPMC
- 23. Joseph L, Goldberg S, Shitrit M, Picard E. High-flow nasal cannula therapy for obstructive sleep apnea in children. J Clin Sleep Med 2015;11:1007-10.ArticlePubMedPMC
- 24. Hawkins S, Huston S, Campbell K, Halbower A. High-flow, heated, humidified air via nasal cannula treats CPAP-intolerant children with obstructive sleep apnea. J Clin Sleep Med 2017;13:981-9.ArticlePubMedPMC
- 25. Amaddeo A, Khirani S, Frapin A, Teng T, Griffon L, Fauroux B. High-flow nasal cannula for children not compliant with continuous positive airway pressure. Sleep Med 2019;63:24-8.ArticlePubMed
- 26. Nishimura M. High-flow nasal cannula oxygen therapy in adults. J Intensive Care 2015;3:15. ArticlePubMedPMCPDF
- 27. Pisani MA, Friese RS, Gehlbach BK, Schwab RJ, Weinhouse GL, Jones SF. Sleep in the intensive care unit. Am J Respir Crit Care Med 2015;191:731-8.ArticlePubMedPMC
- 28. Corral J, Sánchez-Quiroga MÁ, Carmona-Bernal C, Sánchez-Armengol Á, de la Torre AS, Durán-Cantolla J, et al. Conventional polysomnography is not necessary for the management of most patients with suspected obstructive sleep apnea: noninferiority, randomized controlled trial. Am J Respir Crit Care Med 2017;196:1181-90.ArticlePubMed
References
Figure & Data
References
Citations

- Sleep assessment in critically ill adults: A systematic review and meta-analysis
Ellaha Kakar, Matthijs Priester, Pascale Wessels, Arjen J.C. Slooter, M. Louter, M. van der Jagt
Journal of Critical Care.2022; 71: 154102. CrossRef

 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite


