Abstract
- The etiopathogenesis of hydranencephaly remains unclear; however, exposure to toxic substances during pregnancy likely increases hydranencephaly risk. Head computed tomography (CT) was performed in a neonate 9 hours post-delivery because the anterior fontanelle was large and there were clinical signs of encephalopathy. Head CT revealed a lack of both cerebral hemispheres and significant cystic enlargement, while the cerebellar hemispheres and pons were found to have developed normally. History-taking revealed that the mother worked in the automotive industry, specifically in the car paint cleaning business and was exposed to toluene during the pregnancy. The patient was diagnosed with hydranencephaly, central diabetes insipidus and central hypothyroidism. Due to the increased head circumference and tense anterior fontanelle, a ventriculoperitoneal shunt was placed. Toluene exposure during pregnancy should be considered among the causes of hydranencephaly. Furthermore, central diabetes insipidus and central hypothyroidism may develop in such cases.
-
Keywords: hydranencephaly, hypothyroidism; newborn, toluene
Hydranencephaly (HE) is a rare congenital neurological disorder that usually occurs in the second trimester of gestation as a result of the destruction of the cerebral hemispheres. The cerebral hemispheres are commonly replaced by a membranous sac filled with cerebrospinal fluid (CSF) [1]. The etiopathogenesis of HE remains unclear, but most researchers think that HE is associated with brain damage due to the involvement of bilateral internal carotid arteries in the early antenatal period [2]. Other associated conditions are intrauterine infections, rare genetic syndromes, and exposure to toxic substances during pregnancy [3]. This brain malformation often results in fetal loss and therefore is rarely seen postnatally. The incidence of HE also remains unclear. Toluene is an industrial chemical produced during petroleum distillation that is widely used as a solvent. Here, we present the case of a newborn who was born with HE from a mother with occupational exposure to toluene. Toxic exposure started before pregnancy and continued throughout the pregnancy. The neonate also developed central diabetes insipidus (CDI) and central hypothyroidism as a result of the HE.
CASE REPORT
Written informed consent for the study and publication of the photographs was obtained from the patient’s family.
A female neonate was born as the fourth pregnancy of a 22-year-old mother who had no prenatal care. The delivery was spontaneous at home at term with a weight of 3,300 g and the neonate cried spontaneously at birth. She was brought to our institution 9 hours after birth due to respiratory distress. On physical examination, weight was 3,300 g (25–50 percentile), height 50 cm (50–75 percentile), and head circumference was 34 cm (50–75 percentile). Vital signs showed arterial blood pressure, 54/32(24) mm Hg; heart rate, 186 beats/minute; and oxygen saturation, 80%. The patient was in poor condition and was intubated. The anterior fontanelle was open and large. Newborn reflexes were weak. Moro and rooting reflexes were absent. There was biting when the suck reflex was tested.
Given the large anterior fontanelle and signs of encephalopathy, head computed tomography (CT) and cranial magnetic resonance imaging were performed on the day of admission. Both cerebral hemispheres were absent on neuroimaging. There was cystic enlargement bilaterally with intact cerebellar hemispheres and pons (Figure 1). Echocardiography and abdominal ultrasonography were both normal. The patient’s 7th-day TORCH serology was negative. There was no growth in CSF culture. CSF polymerase chain reaction for Toxoplasma gondii was negative. Chromosome analysis revealed that the patient was 46XX.
The mother stated that she did not know she was pregnant until approximately 24 weeks of gestation, and that she had not received antenatal care. She had been working in the auto industry for 8 hours a day on average before and throughout the pregnancy until delivery, including cleaning cars with paint thinner. On postnatal day 21, the neonate’s urine output was polyuric (10 ml/kg/hr) with blood osmolarity of 353 mmol/kg, serum sodium 172 mEq/L, urine osmolarity 400 mOSM/kg. Tandem metabolic screening with urine and blood amino acids was normal. Thyroid stimulating hormone was 100 µU/mL and free T4 was 0.04 ng/dl. In addition to HE, CDI was diagnosed due to hypernatremia, polyuria, high serum osmolarity and low urine osmolarity, and oral desmopressin (5 µg/day) and L-thyroxine 12 µg/kg/day were started for central hypothyroidism.
On postnatal day 32, the neonate was taken off the mechanical ventilator and given oxygen using a hood. Full oral feeds were also started as the suck reflex was active. Oxygen therapy was discontinued on postnatal day 42. Neurosurgery was consulted because of an increase in head circumference of 2 cm over 3 days on postnatal day 65. The patient also developed tachypnea and an increased oxygen need on day 51 of life. The patient’s weekly head circumference is shown in Figure 2. Head CT continued to show a lack of cerebral tissue bilaterally with cystic enlargement. The cerebellar hemispheres and pons remained normal. Phenobarbital treatment was started due to pedaling and convulsive movements of the arms, leading to suspicion of neonatal seizures. Due to the increase in the patient’s head circumference and anterior fontanelle tension, a ventriculoperitoneal shunt was placed by the neurosurgeon (Figure 3). The patient required a tracheostomy and percutaneous endoscopic gastrostomy because she could not be extubated on postnatal day 222. The patient was transferred to a center with a pediatric intensive care unit.
DISCUSSION
HE is a very rare brain anomaly that typically occurs in isolation and usually results in intrauterine death. The most common causes of HE are occlusion of the supra-clinoid segment of the bilateral internal carotid arteries or an extreme state of leukomalacia caused by the fusion of multiple cystic spaces [4]. HE may also occur due to local destruction of brain tissue caused by intrauterine infections [5]. Exposure to toxic substances during pregnancy may also cause HE, and this may be due to fetal hypoxia, consequent cavitation, and resorption of necrotized tissue. The mother was exposed to toluene during the entire pregnancy. Toluene is a widely used organic solvent containing aliphatic, aromatic, and halogenated hydrocarbons, and is ubiquitous in our environment. The teratogenic effects of toluene abuse are more common than occupational exposure to toluene [6]. Neonatal abstinence syndrome may occur as a result of exposure to toluene during pregnancy. The consequences of toluene exposure are often premature birth, intrauterine growth retardation, and low birth weight for gestational age [7]. While the children of mothers who were exposed to toluene occupationally were reported to be neurodevelopmentally normal at the age of 4 years, neurodevelopmental delays and language disorders were found in 80% of infants whose mothers abused toluene as a substance [7]. In this case, maternal toluene exposure was not intermittent and high in level like in substance abuse, but instead was a constant and low-level occupational exposure.
This may explain why the expected signs of embryopathy were not observed. Demir et al. [8] performed animal studies investigating the histopathological effects of toluene on the brain, and showed that toluene causes focal vacuolar degeneration, gliosis and perivascular demyelination, necrosis, excessive enlargement of the brain vessels, and severe degeneration in cell structure, as well as abnormal malformations in the nuclei of oligodendrocyte cells. Filley et al. [9] reported that myelin formation in the central nervous system was significantly affected in women exposed to inhaled toluene during pregnancy. Pavone et al. [4] reported fetal schizencephaly as a result of heavy occupational exposure to toluene during pregnancy. As far as we know, no prior cases of HE due to toluene exposure during pregnancy have been reported. The case presented herein also exhibited development of CDI and central hypothyroidism. CDI is known to occur mostly in midline congenital malformations such as holoprosencephaly and septo-optic dysplasia, but its relationship with HE is less well understood. Omar et al. [10] reported seven cases of HE between 4 days and 4 years of age. They found macrocephaly, growth retardation, convulsive seizures, central hypothyroidism, hypocortisolemia, and panhypopituitarism in these cases. In our case, CDI and central hypothyroidism were observed. In conclusion, HE may develop as a result of occupational exposure to toluene in women of reproductive age. CDI may also occur in neonates with HE.
NOTES
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
AUTHOR CONTRIBUTIONS
Conceptualization: BA, EB. Data curation: BA, EB. Formal analysis: EB, SA. Methodology: BA, EB. Project administration: BA, BG. Visualization: BA, EB. Writing–original draft: BA, BG. Writing–review & editing: EB, BA.
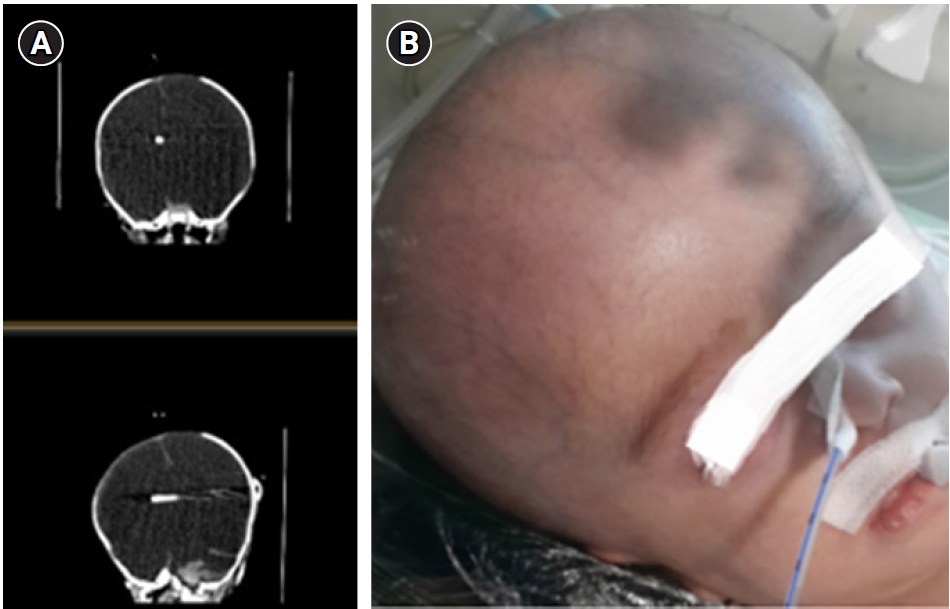
Figure 1.Cranial computed tomography (A) and cranial magnetic resonance imaging (B) taken due to head circumference on the 1 postnatal day.
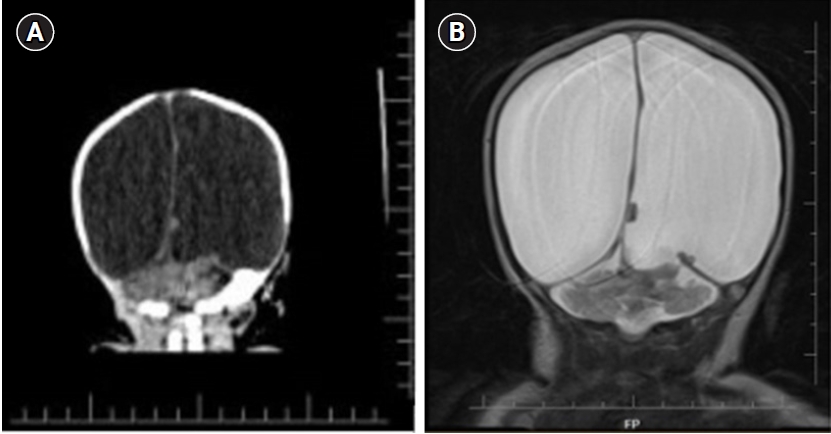
Figure 2.Head circumference of the patient by week. 8 wk, first ventriculoperitoneal shunt insertion; 22 wk, ventriculoperitoneal shunt revision.
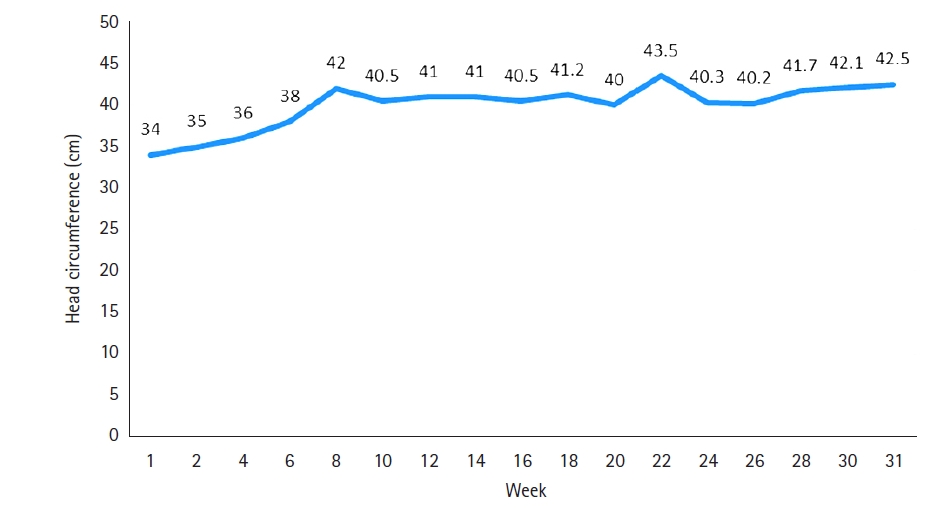
Figure 3.Cranial computed tomography (A) and clinical (B) image of the patient after ventriculoperitoneal shunt insertion.
References
- 1. Khalid M, Khalid S, Zaheer S, Redhu N. Hydranencephaly: a rare cause of an enlarging head size in an infant. N Am J Med Sci 2012;4:520-2.ArticlePubMedPMC
- 2. Quek YW, Su PH, Tsao TF, Chen JY, Ng YY, Hu JM, et al. Hydranencephaly associated with interruption of bilateral internal carotid arteries. Pediatr Neonatol 2008;49:43-7.ArticlePubMed
- 3. Sandoval JI, De Jesus O. Hydranencephaly. In: StatPearls [Internet]. Treasure Island (FL), StatPearls Publishing. 2022.
- 4. Pavone P, Praticò AD, Vitaliti G, Ruggieri M, Rizzo R, Parano E, et al. Hydranencephaly: cerebral spinal fluid instead of cerebral mantles. Ital J Pediatr 2014;40:79. ArticlePubMedPMCPDF
- 5. Plantaz D, Joannard A, Pasquier B, Bost M, Beaudoing A. Hydranencephaly and congenital toxoplasmosis: apropos of 4 cases. Pediatrie 1987;42:161-5.PubMed
- 6. Hannigan JH, Bowen SE. Reproductive toxicology and teratology of abused toluene. Syst Biol Reprod Med 2010;56:184-200.ArticlePubMed
- 7. Laslo-Baker D, Barrera M, Knittel-Keren D, Kozer E, Wolpin J, Khattak S, et al. Child neurodevelopmental outcome and maternal occupational exposure to solvents. Arch Pediatr Adolesc Med 2004;158:956-61.ArticlePubMed
- 8. Demır M, Cicek M, Eser N, Yoldaş A, Sısman T. Effects of acute toluene toxicity on different regions of rabbit brain. Anal Cell Pathol (Amst) 2017;2017:2805370. PubMedPMC
- 9. Filley CM, Halliday W, Kleinschmidt-DeMasters BK. The effects of toluene on the central nervous system. J Neuropathol Exp Neurol 2004;63:1-12.ArticlePubMed
- 10. Omar AT 2nd, Khu KJO. Hydranencephaly complicated by central diabetes insipidus: report of two cases and systematic review of literature. Childs Nerv Syst 2019;35:1165-71.ArticlePubMedPDF
Citations
Citations to this article as recorded by

- Potential Effects of Low-Level Toluene Exposure on the Nervous System of Mothers and Infants
So Yeon Yu, Seung Hwan Kim, Jeong Hyeop Choo, Sehun Jang, Jihyun Kim, Kangmo Ahn, Seung Yong Hwang
International Journal of Molecular Sciences.2024; 25(11): 6215. CrossRef
 , Edin Botan2
, Edin Botan2 , Bülent Gülensoy3
, Bülent Gülensoy3 , Seda Akyol4
, Seda Akyol4









 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite




