To the Editor:
Emergency intubation in critically ill patients is a common procedure and has a high risk of adverse events. A recent international multi-center study identified a 45% occurrence rate of major peri-intubation adverse events [1]. The physiologic extremes presented by critically ill patients, as well as situational challenges associated with managing an airway in the intensive care unit (ICU) rather than the operating room likely contribute to these high rates of adverse events [2]. Guidelines for airway management in the critically ill emphasize communication and planning to minimize the risk of adverse events [3]. At many institutions including ours, such high-risk intubations are performed by an anesthesia airway team that is separate from the primary team caring for the patient, increasing the importance of communication. In this quality improvement project, we sought to reduce the rates of peri-intubation adverse events by instituting a pre-intubation huddle designed to optimize communication between teams.
Critically ill patients older than 18 years who were intubated by the anesthesia airway team in our university hospital medical intensive care unit (MICU) were included. The anesthesia airway team is responsible for emergent airway management outside of the operating room and consists of a senior anesthesia resident or a nurse anesthetist with supervision by an attending anesthesiologist. Preintervention data and postintervention data were prospectively collected from intubations performed from February 1, 2021, to May 31, 2021, and from July 1, 2021, to August 30, 2021, respectively. An education and roll out period occurred from June 1, 2021, to June 30, 2021.
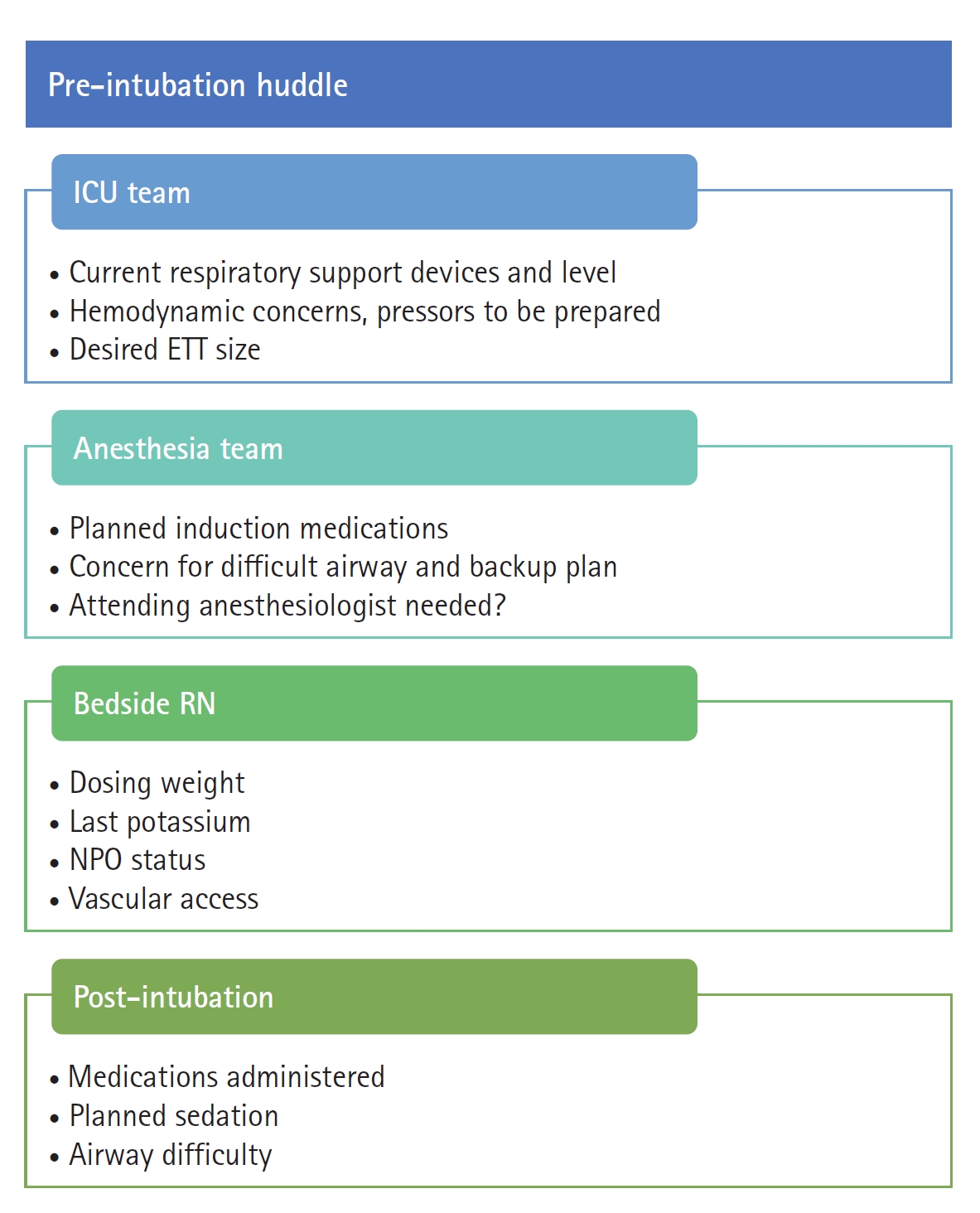
The study intervention was implementation of a pre-intubation team huddle involving representatives from the anesthesia airway team and the MICU team. The huddle was meant to last less than five minutes and to occur at bedside prior to the intubation procedure. The huddle included a checklist to prompt discussion of salient information (Figure 1). A resident, fellow, or advanced practice provider from the MICU team supervised by the attending intensivist presented the patient’s (1) current level of respiratory support; (2) important hemodynamic considerations including known cardiac disease, vasopressor requirements, and concerns for hemodynamic deterioration; and (3) the desired endotracheal tube size. The anesthesia airway team reviewed planned induction medications and concerns for airway difficulty including any additional personnel or equipment. The bedside nurse provided the patient’s weight, potassium, and nil per os status. The contents of the huddle were developed by a multidisciplinary team of intensivists, anesthesiologists, and pharmacists.
Patient demographics, vital signs, and weight; induction drugs; intubating clinician; involvement of an attending anesthesiologist; intubation indication and technique; requirement of new or increased doses of vasopressors; and peri-intubation adverse events were collected. Peri-intubation adverse events were defined as cardiac arrest, hypoxia with oxygen saturation less than 80%, and hemodynamic instability defined as at least one systolic blood pressure measurement less than 70 mm Hg. These definitions were chosen to align closely with those used in the INTUBE study [1]. Statistical analysis included two sample t-tests and a two-sample z-test for proportions (Minitab ver. 21).
Consecutive intubations performed by the anesthesia airway team in the pre- and postintervention periods were audited. In the preintervention period, data from 20 intubation patients were collected. No use of multi-disciplinary huddles or pre-intubation checklists was observed during this period. Demographic information and indications for intubation are shown in Table 1. Among the patients, six had hypotension, six had hypoxia, and two suffered peri-intubation cardiac arrest, an adverse event rate of 70%. Propofol was used for induction in 15 of the 20 intubations. No documentation of notification of an attending anesthesiologist was identified in any case.
Postintervention data were collected from 45 intubation patients, of whom 5 had hypotension, 7 had hypoxia, and 0 had peri-intubation cardiac arrest. The postintervention rate of composite peri-intubation adverse events was significantly reduced at 26.6% (P=0.004) (Table 1). Prompted by discussion between the two teams, an alternative induction agent to propofol was selected in 42% of cases, leading to a significant reduction in propofol use (P=0.007). Documentation of attending anesthesiologist involvement in the intubation procedure was present in 31% of cases. Postintervention adherence to the airway huddle was 93%. In either time, there were no patients intubated under awake conditions, and there were no instances of difficult airway, defined as three or more attempts at intubation or inability to intubate. No statistical differences were noted in patient age, sex, weight, or indication for intubation between groups.
Human factors are an important consideration in successfully managing an airway. Specific human factors involved in complex airway management include leadership, teamwork, situational awareness, decision-making, followership, and communication [4]. In this quality improvement project, our main goal was to reduce peri-intubation adverse events by encouraging better collaboration between the ICU and anesthesia airway teams. Postintervention, we believe that the teams communicated more effectively, discussed the plan during the pre-intubation huddle, and worked together at bedside. We hypothesize that improved communication facilitated better collaboration and anticipatory planning, optimizing some human and environmental factors.
Interestingly, significantly less propofol was used for induction in our postintervention group. Recent studies have found that propofol use for induction was independently associated with cardiovascular instability and collapse [5]. Based on these data, the significant reduction in the use of propofol postintervention may partially explain the reduction in post-intubation complications. Additionally, increased involvement of the attending anesthesiologist in the postintervention group may have prompted a more nuanced discussion of appropriate induction agents. By instituting a pre-intubation huddle to optimize planning and communication before an intubation in the ICU, we were able to achieve a significant reduction in peri-intubation adverse events.
NOTES
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
FUNDING
None.
-
ACKNOWLEDGMENTS
None.
-
AUTHOR CONTRIBUTIONS
Conceptualization: AMB, JLP, KMP. Methodology: KMP. Formal analysis: CAL. Data curation: JLP, ARB, JAL. Project administration: AMB. Writing–original draft: AMB. Writing–review & editing: JLP, ARB, JAL, CAL, KMP.
Figure 1.Pre-intubation huddle. ICU: intensive care unit; ETT: endotracheal tube; NPO: nil per os.
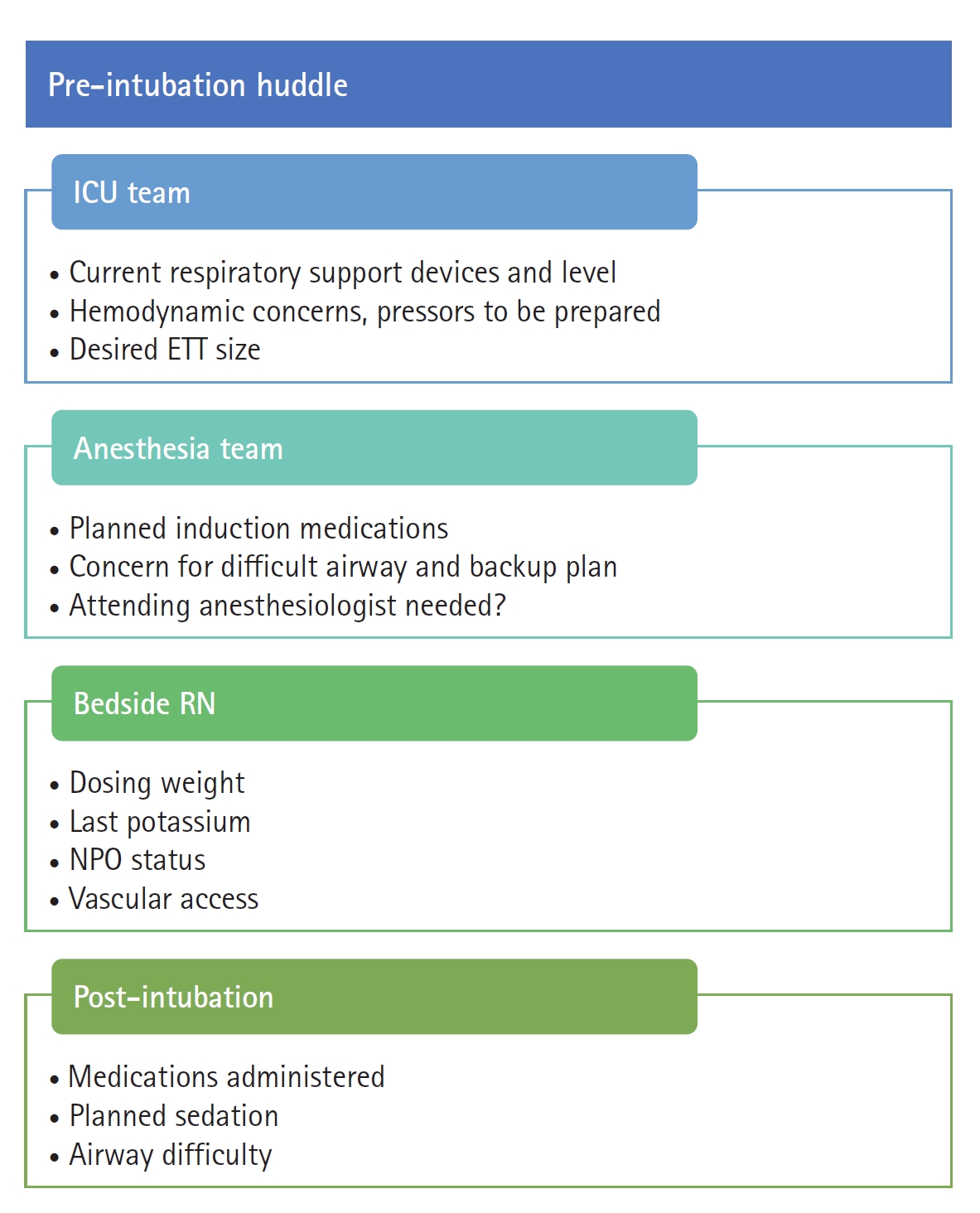
Table 1.Demographics and outcomes
|
Variable |
Preintervention (n=20) |
Postintervention (n=45) |
P-value |
|
Mean age (yr) |
57 |
62 |
0.143 |
|
Male |
10 (50) |
29 (64) |
0.370 |
|
Weight (kg) |
76.1 (69.0–93.9) |
79.7 (65.4–99.3) |
0.784 |
|
Indication for intubation |
|
|
|
|
Airway protection |
2 (10) |
11 (24) |
0.119 |
|
Cardiovascular instability |
5 (25) |
10 (22) |
0.809 |
|
Respiratory failure |
13 (65) |
24 (53) |
0.370 |
|
Induction agent |
|
|
|
|
Propofol |
15 (75) |
19 (42) |
0.007 |
|
Etomidate |
3 (15) |
21 (46) |
0.004 |
|
Midazolam |
4 (20) |
10 (22) |
0.838 |
|
Othera)
|
2 (10) |
7 (15) |
0.519 |
|
NMB agent |
|
|
|
|
Rocuronium |
19 (95) |
38 (84) |
0.147 |
|
Succinylcholine |
0 |
5 (11) |
0.018 |
|
None/otherb)
|
1 (5) |
2 (4) |
0.923 |
|
Adverse event |
14 (70) |
12 (26) |
0.004 |
|
Hypoxia (SpO2 <80%) |
6 (30) |
7 (15) |
0.196 |
|
Cardiac arrest |
2 (10) |
0 |
0.091 |
|
Hypotension (SBP <70 mm Hg) |
6 (30) |
5 (11) |
0.079 |
References
- 1. Russotto V, Myatra SN, Laffey JG, Tassistro E, Antolini L, Bauer P, et al. Intubation practices and adverse peri-intubation events in critically ill patients from 29 countries. JAMA 2021;325:1164-72.PubMedPMC
- 2. Myatra SN, Divatia JV, Brewster DJ. The physiologically difficult airway: an emerging concept. Curr Opin Anaesthesiol 2022;35:115-21.ArticlePubMed
- 3. Brindley PG, Beed M, Law JA, Hung O, Levitan R, Murphy MF, et al. Airway management outside the operating room: how to better prepare. Can J Anaesth 2017;64:530-9.ArticlePubMedPDF
- 4. Gleeson S, Groom P, Mercer S. Human factors in complex airway management. BJA Educ 2016;16:191-7.Article
- 5. Russotto V, Tassistro E, Myatra SN, Parotto M, Antolini L, Bauer P, et al. Peri-intubation cardiovascular collapse in patients who are critically ill: insights from the INTUBE study. Am J Respir Crit Care Med 2022;206:449-58.ArticlePubMed
Citations
Citations to this article as recorded by

 , Jenna L Potter2
, Jenna L Potter2 , Anna R Benson2
, Anna R Benson2 , Jared A Larson2, Christopher A Linke2, Kathryn M Pendleton3
, Jared A Larson2, Christopher A Linke2, Kathryn M Pendleton3





 KSCCM
KSCCM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite