Abstract
-
Background
- Sodium-glucose cotransporter-2 inhibitors (SGLT2i) have been shown to reduce organ dysfunction in renal and cardiovascular disease. There are limited data on the role of SGLT2i in acute organ dysfunction. We conducted a study to assess the effect of SGLT2i taken prior to intensive care unit (ICU) admission in diabetic patients admitted with septic shock.
-
Methods
- This retrospective cohort study used electronic medical records and included diabetic patients admitted to the ICU with septic shock. We compared diabetic patients on SGLT2i to those who were not on SGLT2i prior to admission. The primary outcome was in-hospital mortality, and secondary outcomes included hospital and ICU length of stay, use of renal replacement therapy, and 28- and 90-day mortality.
-
Results
- A total of 98 diabetic patients was included in the study, 36 in the SGLT2i group and 62 in the non-SGLT2i group. The Sequential Organ Failure Assessment and Acute Physiology and Chronic Health Evaluation III scores were similar in the groups. Inpatient mortality was significantly lower in the SGLT2i group (5.6% vs. 27.4%, P=0.008). There was no significant difference in secondary outcomes.
-
Conclusion
- Our study found that diabetic patients on SGLT2i prior to hospitalization who were admitted to the ICU with septic shock had lower inpatient mortality compared to patients not on SGLT2i.
-
Keywords: intensive care unit; mortality; septic shock, sodium-glucose cotransporter-2 inhibitor, type 2 diabetes mellitus
INTRODUCTION
Septic shock represents about two percent of all hospital admissions in the United States, with inpatient mortality rates around 29% [1]. Other than antimicrobial therapy, targeted therapies that reduce mortality in septic shock are limited [2,3]. A recent study dapagliflozin in patients with cardiometabolic risk factors hospitalised with COVID-19 (DARE-19) evaluated the use of sodium-glucose cotransporter-2 inhibitors (SGLT2i) in acutely ill patients. In 2021, this randomized controlled clinical trial investigated the use of the SGLT2i dapagliflozin in patients hospitalized with coronavirus disease-19 (COVID-19) [4]. As SGLT2i medications have become part of the mainstay therapy in heart failure and chronic kidney disease (CKD) in addition to diabetes, the authors theorized that SGLT2i may have potential organ-protective effects in acute illnesses such as COVID-19 [5-8]. Although the study did not find a significant difference in organ dysfunction or death, the medications were well tolerated [4]. Another study by Angé et al. [9] showed a potential mechanistic protective effect of SGLT2i in mouse models with capillary leak syndrome. The researchers demonstrated that canagliflozin acts by counteracting lipopolysaccharide-induced vascular leak in mice.
Although these protective effects have been observed in specific organ dysfunction, studies evaluating the use of SGLT2i in shock, simultaneously affecting multiple organ systems, are lacking. Our study aimed to evaluate whether SGLT2i medications were associated with improved outcomes in diabetic adults admitted to the intensive care unit (ICU) with septic shock.
MATERIALS AND METHODS
Setting and Population
We conducted a retrospective cohort study to compare outcomes in diabetic adult patients (18 years or older) on SGLT2i and admitted to the ICU for septic shock to those in diabetic adults who were not on SGLT2i at the time of admission. The Institutional Review Board of Mayo Clinic (ID 22-000810) approved the study on February 2, 2022. The requirement for written informed consent was waived for this minimal-risk study. Procedures were followed in accordance with the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1975.
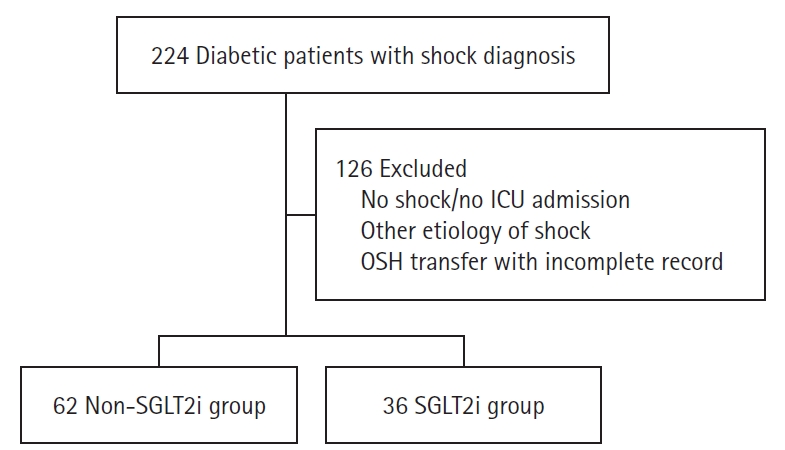
An electronic medical record review identified the study cohort using International Classification of Diseases codes, 10th and 9th revisions (ICD-10 and ICD-9) such as R65.21 (severe sepsis with septic shock) and 785.52 (septic shock), respectively. The patient pool was narrowed to those who had been diagnosed with type 2 diabetes mellitus. The medication lists of the diabetic patients with septic shock were reviewed to identify those prescribed SGLT2i. The SGLT2i group included only patients prescribed SGLT2i as part of their outpatient medication list within 48 hours of admission to ICU for septic shock. Other exclusion criteria were other etiologies of shock, post-surgical patients admitted in the immediate postoperative period to the ICU, and patients transferred from an outside facility and insufficient records (Figure 1).
Data Collection
The electronic medical record collected baseline data about demographics, clinical characteristics, use of anti-hyperglycemic agents and other preadmission medications, hemoglobin A1c within 12 months of admission, source of infection, and type of vasopressor used. The Acute Physiology and Chronic Health Evaluation (APACHE) III and Sequential Organ Failure Assessment (SOFA) scores were recorded as well as the types of SGLT2i used. The primary outcome of the study was in-hospital mortality, and secondary outcomes included hospital and ICU length of stay, use of renal replacement therapy, and 28- and 90-day mortality.
Data Analysis Strategy
The study used R software version 4.1.2 (R Foundation for Statistical Computing) to conduct analyses. Continuous variables were examined with histograms and summarized using median and interquartile range. Categorical variables were described using frequencies and proportions. Due to the non-normal distribution of the variables, differences between SGLT2i patients and non-SGLT2i were obtained using median and chi-square tests. A value of P <0.05 determined statistical significance for all tests.
RESULTS
Baseline Characteristics
A total of 98 diabetic patients admitted to the ICU with septic shock was included in the study. Sixty-two patients (63.3%) were not on SGLT2i, and 36 (36.7%) were on therapy with an SGLT2i prior to hospital admission. The dates of hospitalization ranged between years 2014 and 2022.
Most of the demographics, baseline characteristics, and medication use were similar between the two groups (Table 1). The median ages of SGLT2i and non-SGLT2i cohorts were 68 and 70 years, respectively. There were more male patients in the SGLT2i group, 72.2% versus 58.1% of females, but this difference was not significant. Body mass index was similar in the two groups. Because of the small sample size of individuals with ethnicity other than White (n=8), the study combined all other groups into a single category, with no difference in ethnicities between the SGLT2i and non-SGLT2i groups. Glucagon-like peptide-1 agonists, metformin, and angiotensin-converting enzyme inhibitors were more frequently used in the SGLT2i group. Patients in the SGLT2i group had higher median hemoglobin A1c (7.8 vs. 7, P=0.026). There was also a difference in the sources of infection between the two groups. Close to half of the patients in non-SGLT2i group had a gastrointestinal source of infection compared to only 16.7% of the SGLT2i group. A large portion (30.6%) of the patients in the SLGT2i group had other sources of infection such as bacteremia, followed by those with a pulmonary origin. There was a difference between the two groups in the presence of CKD and coronary artery disease (CAD). CKD was more common in the non-SGLT2i group (38.7% vs. 11.1%, P=0.004), while CAD was more common in the SGLT2i group (33.3% vs. 14.5%, P=0.029). Illness severity scores of SOFA and APACHE III were similar between the two groups. Phenylephrine was more frequently used in the SLGT2i group (16.7 % vs. 3.2%, P=0.019). The types and numbers of SGLT2i users are shown in Table 2.
Outcomes
The primary outcome of in-hospital mortality was significantly lower in the SGLT2i group compared to the non-SGLT2i group (5.6% vs. 27.4%, P=0.008). The difference at 28 and 90 days was not significant. There was no difference between the two groups in either hospital or ICU length of stay. Additionally, there was no difference in renal replacement therapy rates between the two cohorts. Table 3 summarizes the study outcomes.
DISCUSSION
Our retrospective cohort study evaluating the role of SGLT2i in ICU outcomes of diabetic patients admitted for septic shock found an association between diabetic patients taking SGLT2i and lower in-hospital mortality compared to diabetic patients not on SGLT2i. The lack of hospital mortality reduction at 28 and 90 days could be related to study withdrawal or discontinuation of SGLT2i at the time of admission.
Although the study cohort was small, these findings are consistent with the known organ protective effect and mortality reduction seen with SGLT2i in patients with CKD and heart failure [5-8]. Although there were some differences in baseline characteristics such as CKD and CAD, the APACHE III and SOFA scores were similar in the groups, suggesting that they were equal in their illness severity at the time of admission to the ICU.
One of the only clinical trials to test the hypothesis of an impact of SGLT2i on reducing organ dysfunction and mortality in acutely ill patients is the DARE-19 trial [4]. This double-blind, randomized, placebo-controlled 1:1 trial analyzed the impact of dapagliflozin on patients admitted to the hospital with COVID-19. The primary outcomes included a composite of time to new or worsening organ dysfunction (respiratory, cardiovascular, and renal decompensation) and death from any cause. Treatment with SGLT2i did not significantly reduce organ dysfunction in this study. The mortality rates were lower in the SGLT2i group (6.6% vs. 8.6%; hazard ratio, 0.77; 95% confidence interval, 0.52–1.16), but the difference was not statistically significant. Though the authors anticipated higher rates of organ dysfunction and death, they believe that the improvements in COVID-19 treatment played a role in the lower-than-expected events.
Possible mechanistic explanations for the benefit of SGLT2i in shock include improved energy metabolism and reduced inflammation through interleukin (IL)-1β andIL-6 [9-11]. Angé et al. [9] also identified a potential mechanism by which SGLT2i may reduce capillary leakage. Lipopolysaccharide O55:B5 (LPS) was injected into mice pretreated with a clinically relevant dose of canagliflozin. The study demonstrated that canagliflozin reduced LPS-induced myocardial edema and prevented albuminemia. The mechanism they identified was canagliflozin activation of the AMP-activated protein kinase (AMPK) pathway resulting in the reinforcement of inter-endothelial junctions [9]. They tested this hypothesis further with the treatment of human mammary epithelial cells with plasma from both healthy volunteers and septic shock patients. Canagliflozin showed preservation of vascular endothelial cadherin integrity [9]. Several other potential beneficial mechanisms of SGLT2i have been identified. For example, in human endothelial cells, canagliflozin has been shown to reduce pro-inflammatory cytokines IL-1β-mediated secretion of IL-6 and monocyte chemoattractant protein-1 [11]. These mediators are well known to play a role in the pathophysiology of sepsis [12].
Renal impairment in septic shock is an important consideration when discussing initiation of SGLT2i. Several studies have evaluated the use of SGLT2i after a certain reduction in estimated glomerular filtration rate (eGFR). The Dapagliflozin in Patients with Chronic Kidney Disease (DAPA-CKD) trial evaluated the effects of dapagliflozin in patients with CKD with and without diabetes. The trial included 4,304 participants, 624 with eGFR <30. The primary composite outcome was sustained decline in eGFR of at least 50%, end-stage renal disease, and death from renal or cardiovascular events. The results were persistent regardless of eGFR, with significantly lower rates of primary outcomes in patients treated with dapagliflozin [6,13]. A more recent trial published by the EMPA-Kidney Collaborative Group evaluated the effect of empagliflozin on the progression of CKD. A total of 6,609 patients was enrolled, with 2,282 (34.5%) having eGFR <30. Like the DAPA-CKD trial, progression of CKD and death from cardiovascular causes occurred at significantly lower rates (13.1% vs. 16.9%) in the empagliflozin group compared to the placebo group. These benefits were consistent regardless of eGFR [8]. The evidence for patients with eGFR < 25 is limited, and current trials are enrolling patients to evaluate the safety and efficacy of canagliflozin and dapagliflozin in patients with CKD stages 4 and 5. Current Kidney Disease Improving Global Outcomes (KDIGO) guidelines recommend use of SGTL2i in patients with eGFR >20 until dialysis or transplant [14].
The safety profile of SGLT2i has been extensively studied. Fournier’s gangrene was initially of concern as a serious complication of SGLT2i use. However, a more recent meta-analysis of 42,415 patients on SGLT2i found no difference in rates of Fournier’s gangrene, cellulitis, or erysipelas [15]. The early concerns for increased rates of urinary tract infections have also been evaluated, revealing no association [6,8,13].
SGLT2i are associated with euglycemic diabetic ketoacidosis (DKA) in patients with type 1 diabetes mellitus, at rates of 4%–6% [13]. However, the rates of DKA are much lower in patients with type 2 diabetes mellitus and have occurred at similarly low rates in recent CKD studies [6,8,13]. In the DARE-19 trial, DKA occurred only in two patients receiving dapagliflozin and was reported as non-severe, resolving after medication discontinuation [4].
We acknowledge the limitations of this retrospective analysis. Due to the small sample size and the small number of events (e.g., deaths), regression analysis could not be performed to account for some of the baseline differences (CAD and CKD). SGLT2i are typically discontinued on admission, and the half-life of most ranges between eight to 16 hours [16]. Therefore, the impact of SGLT2i on outcomes may be blunted in our study. However, the cellular signaling and downstream effects could potentially persist and could be a theoretical explanation for the decreased inpatient mortality. Inherent limitations of a retrospective analysis such as limitations of medical records, lack of ability for stringent patient selection, and inability to randomize, all apply to our study. However, SOFA and APACHE III scores were used to assess patient illness severity and were similar in the two cohorts.
We found a significant association of lower in-hospital mortality in septic shock in diabetic patients taking a SGLT2i at the time of ICU admission. Although there were several limitations to this retrospective study, our findings suggest that SGLT2i could provide a beneficial effect in this patient population. Larger studies are needed to confirm this association and to understand the beneficial effects of these drugs in septic shock patients.
KEY MESSAGES
▪ Our study found an association between sodium-glucose cotransporter-2 inhibitors (SGLT2i) use prior to admission and reduced inpatient mortality in diabetic patients with septic shock.
▪ Large prospective studies are needed to assess the potential mortality benefit of SGLT2i use in septic shock.
NOTES
-
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
-
FUNDING
None.
-
ACKNOWLEDGMENTS
None.
-
AUTHOR CONTRIBUTIONS
Conceptualization: NA, RCC. Methodology: NA, RCC. Formal analysis: NA, CIY, RCC. Data curation: NA, AAA, SG, SB. Visualization: NA, RCC. Project administration: NA, RCC. Writing–original draft: all authors. Writing–review & editing: all authors.
Figure 1.Flowchart for patient selection. ICU: intensive care unit; OSH: outside hospital; SGLT2i: sodium-glucose cotransporter-2 inhibitors.

Table 1.Patient demographics and baseline characteristics
|
Variable |
SGLT2i (n=36) |
Non-SGLT2i (n=62) |
P-value |
|
Age (yr) |
68 (62–72) |
70 (58–78) |
0.140a)
|
|
Sex |
|
|
0.161b)
|
|
Male |
26 (72.2) |
36 (58.1) |
|
|
Female |
10 (27.8) |
26 (41.9) |
|
|
Race |
|
|
0.417b)
|
|
White |
32 (88.9) |
58 (93.5) |
|
|
Other |
4 (11.1) |
4 (6.5) |
|
|
BMI (kg/m2) |
29.9 (16.5–51.3) |
29.5 (19.1–51.3) |
0.677a)
|
|
Comorbid condition |
|
|
|
|
CAD |
12 (33.3) |
9 (14.5) |
0.029b)
|
|
CKD |
4 (11.1) |
24 (38.7) |
0.004b)
|
|
Hypertension |
30 (83.3) |
44 (71.0) |
0.170b)
|
|
Infection source |
|
|
0.004b)
|
|
Gastrointestinal |
6 (16.7) |
29 (46.8) |
|
|
Pulmonary |
8 (22.2) |
14 (22.6) |
|
|
Otherc)
|
11 (30.6) |
5 (8.1) |
|
|
Urinary |
7 (19.4) |
8 (12.9) |
|
|
Unknown |
2 (5.6) |
6 (9.7) |
|
|
Cutaneous |
2 (5.6) |
0 |
|
|
Medication |
|
|
|
|
ACEi |
23 (63.9) |
25 (40.3) |
0.024b)
|
|
β-Blocker |
17 (47.2) |
31 (50.0) |
0.791b)
|
|
Statin |
25 (69.4) |
35 (56.5) |
0.203b)
|
|
Insulin |
16 (44.4) |
22 (35.5) |
0.380b)
|
|
Metformin |
19 (52.8) |
11 (17.7) |
<0.001b)
|
|
Sulfonylureas |
7 (19.4) |
10 (16.1) |
0.676b)
|
|
GLP-1 agonist |
9 (25.0) |
2 (3.2) |
<0.001b)
|
|
Thiazolidinedione |
2 (5.6) |
1 (1.6) |
0.275b)
|
|
DPP-4 |
3 (8.3) |
1 (1.6) |
0.105b)
|
|
Aspirin |
12 (33.3) |
21 (33.9) |
0.957b)
|
|
Hemoglobin A1cd)
|
7.8 |
7 |
0.026a)
|
|
SOFA score |
9.5 (7.8–11.0) |
9.0 (7.0–11.0) |
0.214a)
|
|
APACHE III score |
75.5 (65.0–94.5) |
73.5 (60.3–102.0) |
0.878a)
|
|
Vasopressor |
|
|
|
|
Norepinephrine |
35 (97.2) |
58 (93.5) |
0.426b)
|
|
Vasopressin |
14 (38.9) |
23 (37.1) |
0.860b)
|
|
Phenylephrine |
6 (16.7) |
2 (3.2) |
0.019b)
|
|
Epinephrine |
3 (8.3) |
1 (1.6) |
0.105b)
|
|
Dopamine |
0 |
2 (3.2) |
0.276b)
|
Table 2.Types of SGLT2i taken by the cohort
|
SGLT2i type |
Patient (n=36) |
|
Empagliflozin |
23 (63.9) |
|
Dapagliflozin |
8 (22.2) |
|
Canagliflozin |
5 (13.9) |
Table 3.Study outcomes
|
Variable |
SGLT2i (n=36) |
Non-SGLT2i (n=62) |
P-value |
|
Hospital length of stay |
7.5 (4.8–12.3) |
9.2 (4.8–12.0) |
0.40a)
|
|
ICU length of stay |
2.8 (2.1–4.0) |
2.9 (1.7–5.3) |
0.40a)
|
|
Inpatient mortality |
2 (5.6) |
17 (27.4) |
0.008b)
|
|
28-Day mortality |
7 (19.4) |
22 (35.5) |
0.094b)
|
|
90-Day mortality |
13 (36.1) |
25 (40.3) |
0.680b)
|
|
RRT |
4 (11.1) |
13 (21.0) |
0.214b)
|
References
- 1. Angus DC, Linde-Zwirble WT, Lidicker J, Clermont G, Carcillo J, Pinsky MR. Epidemiology of severe sepsis in the United States: analysis of incidence, outcome, and associated costs of care. Crit Care Med 2001;29:1303-10.ArticlePubMed
- 2. Evans L, Rhodes A, Alhazzani W, Antonelli M, Coopersmith CM, French C, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Intensive Care Med 2021;47:1181-247.PubMedPMC
- 3. Venkatesh B, Finfer S, Cohen J, Rajbhandari D, Arabi Y, Bellomo R, et al. Adjunctive glucocorticoid therapy in patients with septic shock. N Engl J Med 2018;378:797-808.ArticlePubMed
- 4. Kosiborod MN, Esterline R, Furtado RH, Oscarsson J, Gasparyan SB, Koch GG, et al. Dapagliflozin in patients with cardiometabolic risk factors hospitalised with COVID-19 (DARE-19): a randomised, double-blind, placebo-controlled, phase 3 trial. Lancet Diabetes Endocrinol 2021;9:586-94.ArticlePubMedPMC
- 5. Packer M, Anker SD, Butler J, Filippatos G, Pocock SJ, Carson P, et al. Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med 2020;383:1413-24.PubMed
- 6. Heerspink HJ, Stefánsson BV, Correa-Rotter R, Chertow GM, Greene T, Hou FF, et al. Dapagliflozin in patients with chronic kidney disease. N Engl J Med 2020;383:1436-46.ArticlePubMed
- 7. Anker SD, Butler J, Filippatos G, Ferreira JP, Bocchi E, Böhm M, et al. Empagliflozin in heart failure with a preserved ejection fraction. N Engl J Med 2021;385:1451-61.PubMed
- 8. The EMPA-KIDNEY Collaborative Group; Herrington WG, Staplin N, Wanner C, Green JB, Hauske SJ, et al. Empagliflozin in patients with chronic kidney disease. N Engl J Med 2023;388:117-27.ArticlePubMed
- 9. Angé M, De Poortere J, Ginion A, Battault S, Dechamps M, Muccioli GG, et al. Canagliflozin protects against sepsis capillary leak syndrome by activating endothelial α1AMPK. Sci Rep 2021;11:13700. PubMedPMC
- 10. Lopaschuk GD, Verma S. cardiovascular benefits of sodium glucose co-transporter 2 (SGLT2) inhibitors: a state-of-the-art review. JACC Basic Transl Sci 2020;5:632-44.PubMedPMC
- 11. Mancini SJ, Boyd D, Katwan OJ, Strembitska A, Almabrouk TA, Kennedy S, et al. Canagliflozin inhibits interleukin-1β-stimulated cytokine and chemokine secretion in vascular endothelial cells by AMP-activated protein kinase-dependent and -independent mechanisms. Sci Rep 2018;8:5276. ArticlePubMedPMCPDF
- 12. Huang J, Liu K, Zhu S, Xie M, Kang R, Cao L, et al. AMPK regulates immunometabolism in sepsis. Brain Behav Immun 2018;72:89-100.ArticlePubMed
- 13. Yau K, Dharia A, Alrowiyti I, Cherney DZ. Prescribing SGLT2 inhibitors in patients with CKD: expanding indications and practical considerations. Kidney Int Rep 2022;7:1463-76.ArticlePubMedPMC
- 14. Kidney Disease: Improving Global Outcomes (KDIGO) Diabetes Work Group. KDIGO 2022 clinical practice guideline for diabetes management in chronic kidney disease. Kidney Int 2022;102(5S):S1-127.ArticlePubMed
- 15. Silverii GA, Dicembrini I, Monami M, Mannucci E. Fournier’s gangrene and sodium-glucose co-transporter-2 inhibitors: a meta-analysis of randomized controlled trials. Diabetes Obes Metab 2020;22:272-5.ArticlePubMedPDF
- 16. Beitelshees AL, Leslie BR, Taylor SI. Sodium-glucose cotransporter 2 inhibitors: a case study in translational research. Diabetes 2019;68:1109-20.ArticlePubMedPMCPDF
Citations
Citations to this article as recorded by

 , Abdelmohaymin A. Abdalla2
, Abdelmohaymin A. Abdalla2 , Simran Gupta1
, Simran Gupta1 , Shubhang Bhatt1
, Shubhang Bhatt1 , Claire I. Yee3
, Claire I. Yee3 , Rodrigo Cartin-Ceba2
, Rodrigo Cartin-Ceba2






 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite