Abstract
- Extracorporeal membrane oxygenation (ECMO) has been used successfully in critically ill patients with traumatic lung injury and offers an additional treatment modality. ECMO is mainly used as a bridge treatment to delayed surgical management; however, only a few case reports have presented the successful application of ECMO as intraoperative support during the surgical repair of traumatic bronchial injury. A 38-year-old man visited our hospital after a blunt chest trauma. His chest imaging showed hemopneumothorax in the left hemithorax and a finding suspicious for left main bronchus rupture. Bronchoscopy was performed and confirmed a tear in the left main bronchus and a congenital tracheal bronchus. We decided to provide venovenous ECMO support during surgery for bronchial repair. We successfully performed main bronchial repair in this traumatic patient with a congenital tracheal bronchus. We suggest that venovenous ECMO offers a good option for the treatment of bronchial rupture when adequate ventilation is not possible.
-
Keywords: blunt injury; extracorporeal membrane oxygenation; lung injury; trauma
Extracorporeal membrane oxygenation (ECMO) can provide temporary replacement for damaged lung with sufficient ventilation and oxygenation allowing time for the recovery. Despite the risks of systemic anticoagulation and of consumptive coagulopathy in trauma cases, ECMO has been used successfully in critically ill patients with traumatic lung injury and can offer an additional treatment modality.[1] ECMO is mainly used as a bridge treatment to delayed surgical management;[2] however, only a few case reports have been presented the successful application of ECMO as an intraoperative support during the surgical repair of traumatic bronchial injury.[3] We demonstrate a case of a successful main bronchial repair with venovenous ECMO support for an adult traumatic patient with a congenital tracheal bronchus.
Case Report
A previously healthy 38-year-old man visited the hospital emergency department after falling from a 1.5-m ladder and bumping his chest on the ground. At the time of the emergency department visit, his vital signs were as follows: blood pressure, 126/74 mmHg; pulse rate, 102 beats/min; respiration rate, 30 breaths/min; and body temperature, 36.0°C. He had decreased breath sound in the left lung at auscultation. The arterial blood gas analysis showed the following results: pH 7.30; PaCO2, 50 mmHg; PaO2, 42 mmHg; and HCO3, 24.6 mM. His chest radiograph (Fig. 1) and chest computed tomography (Fig. 2A and B) showed hemopneumothorax in the left hemithorax, fracture in the left sixth rib, and multifocal ground glass opacity and nodules in both lungs. A chest tube was inserted into his left pleural space, and he was admitted to the surgical intensive care unit (ICU).
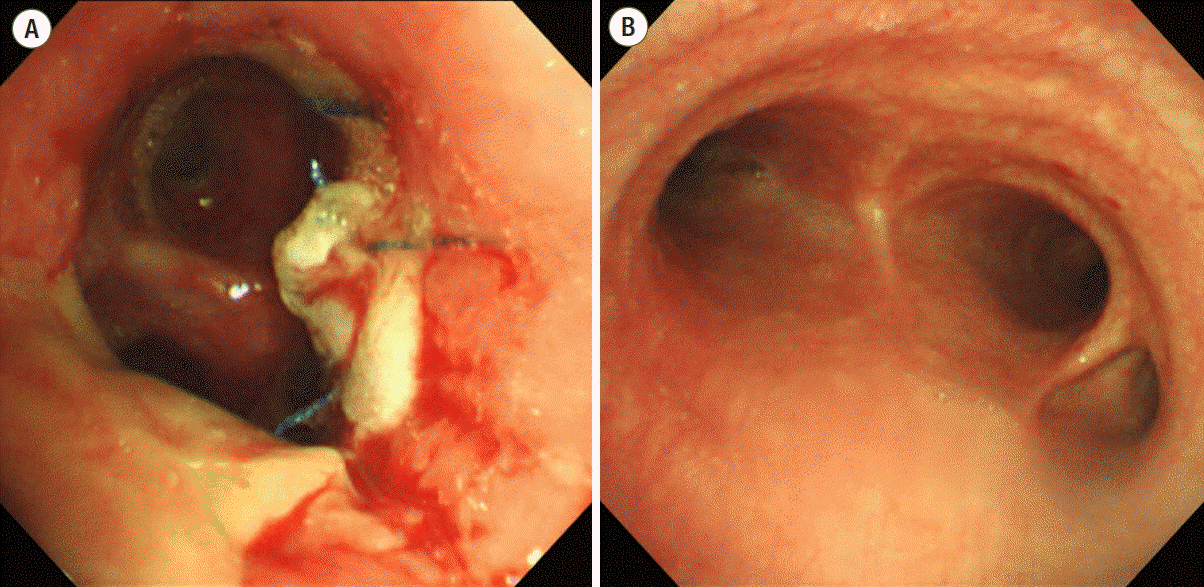
Bronchoscopy was performed to check for bronchial injury, and a tear in the left main bronchus was confirmed (Fig. 4B). A congenital anomaly of the right upper bronchus which originates from the lateral tracheal wall was found incidentally in the distal tracheal examination.
The patient developed progressive hypoxemia and hypercarpnia after a bronchoscopic evaluation. Despite immediate intubation and positive ventilation with 100% FiO2, the preoperative arterial blood gas analysis showed the following results: pH 7.18; PaCO2, 60 mmHg; PaO2, 66 mmHg; and HCO3, 22.4 mM. Moreover, the patient had a congenital anomaly which might not be suitable for the one lung ventilation. We could not expect sufficient oxygenation and ventilation through one lung ventilation in this patient, so we decided to apply the venovenous ECMO for the respiratory support during the surgical repair of the bronchial injury.
After the induction of general anesthesia, the right and left femoral veins were cannulated (21-Fr and 17-Fr Medtronic Biomedicus Cannula®, respectively; Medtronic, Minneapolis, MN, USA) by using Seldinger’s technique, and then venovenous ECMO was implemented. A left posterolateral thoracotomy was performed with entry into the left side of the chest through the fifth intercostal space. No pleural adhesion or hematoma was seen, and the soft tissue and pleura were separated from the left main bronchus to verify the main lesion. Exploration of this area revealed a detachment of the left main bronchus from the lower 3 cm to the carina, and a longitudinal opening at the proximal portion of the left main bronchus (Fig. 3). After the complete repair of the rupture of the left main bronchus, the left lung was inflated and a water test confirmed the absence of an air leak. A drain tube was inserted, and the thoracotomy incision was closed in layers. The patient was returned to the ICU with intubation and low-volume pressure control ventilation, and remained supported with ECMO.
His vital signs were stable and his lung function was rapidly restored in the immediate postoperative phase. The patient was gradually weaned from ECMO and decannulated after postoperative day 3. He underwent a bronchoscopy postoperatively. The left main bronchus anastomosis site was intact on bronchoscopy (Fig. 4A). He recovered without any event and was discharged. He remained well at 1 month after the surgery.
Discussion
Extracorporeal lung support devices are a life-saving treatment option for severe thoracic trauma patients.[4,5] ECMO may offer an additional treatment modality in adult patients with severe traumatic lung injury or acute respiratory failure who do not respond to maximal conventional ventilatory support.[1] ECMO is mainly used as a bridge treatment to delayed surgical management.[2]
Mechanical ventilation under general anesthesia itself used to provide sufficient oxygeneation and ventilation during the surgical management of bronchial rupture. But in the case, the patient developed progressive hypoxemia and hypercarpnia despite the mechanical ventilation. Additionally, the atypical origin of the right upper-lobe bronchus may complicate one-lung ventilation during thoracic surgery.[6]
Venovenous ECMO allows adequate oxygenation and ventilation, and reduces the risk of acute lung injury.[7] His vital signs were stable and his lung function was rapidly restored in the immediate postoperative phase. We decided to extubate and wean him from ECMO promptly to avoid the associated risks of prolonged ECMO support. The surgical repair of bronchial injury and weaning from ECMO were successfully done.
We report a case of a successful main bronchial repair by providing venovenous ECMO support for an adult traumatic patient with a congenital tracheal bronchus. A few case reports have presented the successful application of ECMO in the emergency repair of traumatic airway injury. As shown in this report, venovenous ECMO offers a good option for the treatment of bronchial rupture when adequate ventilation is not possible.
NOTES
-
No potential conflict of interest relevant to this article was reported.
Fig. 1.Chest radiograph taken in the emergency department showing pneumothorax in the left lung.
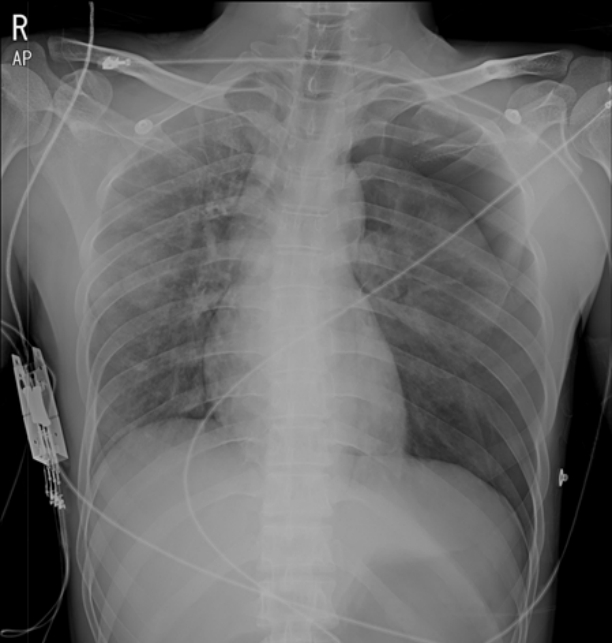
Fig. 2.Transverse (A and B) chest computed tomography images showing hemopneumothorax in the left hemithorax, fracture in the left sixth rib, and multifocal ground glass opacity and nodules in both lungs.

Fig. 3.Intraoperative photograph of the detachment of the left main bronchus from the lower 3 cm to the carina and a longitudinal opening at the proximal portion of the left main bronchus.
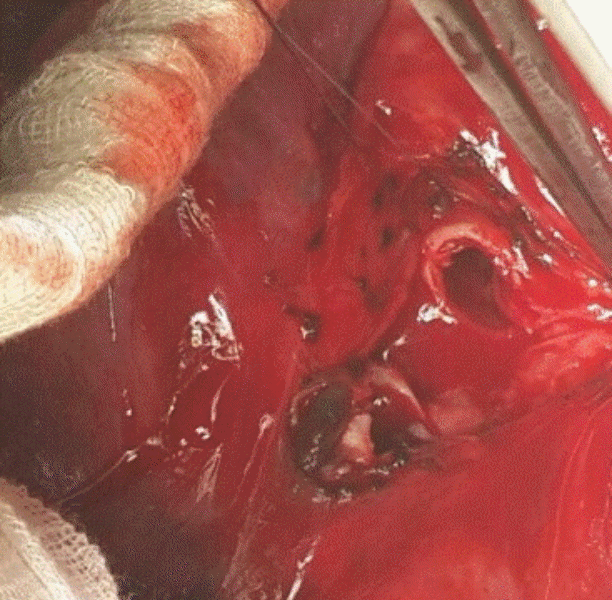
Fig. 4.Bronchoscopy images showing an intact left main bronchus anastomosis site (A) and the origin of the right upper bronchus at the lateral tracheal wall (B).
References
- 1. Cordell-Smith JA, Roberts N, Peek GJ, Firmin RK. Traumatic lung injury treated by extracorporeal membrane oxygenation (ECMO). Injury 2006;37:29-32.ArticlePubMed
- 2. Sian K, McAllister B, Brady P. The use of extracorporeal membrane oxygenation therapy in the delayed surgical repair of a tracheal injury. Ann Thorac Surg 2014;97:338-40.ArticlePubMed
- 3. Liu C, Lin Y, Du B, Liu L. Extracorporeal membrane oxygenation as a support for emergency bronchial reconstruction in a traumatic patient with severe hypoxaemia. Interact Cardiovasc Thorac Surg 2014;19:699-701.ArticlePubMed
- 4. Ried M, Bein T, Philipp A, Müller T, Graf B, Schmid C, et al. Extracorporeal lung support in trauma patients with severe chest injury and acute lung failure: a 10-year institutional experience. Crit Care 2013;17:R110. ArticlePubMedPMC
- 5. Korvenoja P, Pitkänen O, Berg E, Berg L. Veno-venous extracorporeal membrane oxygenation in surgery for bronchial repair. Ann Thorac Surg 2008;86:1348-9.ArticlePubMed
- 6. Peragallo RA, Swenson JD. Congenital tracheal bronchus: the inability to isolate the right lung with a univent bronchial blocker tube. Anesth Analg 2000;91:300-1.ArticlePubMed
- 7. Ventetuolo CE, Muratore CS. Extracorporeal life support in critically ill adults. Am J Respir Crit Care Med 2014;190:497-508.ArticlePubMedPMC
Citations
Citations to this article as recorded by










 KSCCM
KSCCM

 PubReader
PubReader ePub Link
ePub Link Cite
Cite





