Abstract
- Scrub typhus is a mite-borne infectious disease caused by Orientia tsutsugamushi. Although early diagnosis and appropriate antibiotic therapy improve the prognosis for the majority of patients, life-threatening complications are not uncommon. Here, we present a case of successful veno-veno-type extracorporeal membrane oxygenation for scrub typhus-induced complications, including acute respiratory distress syndrome, myocarditis and multi-organ dysfunction. To our knowledge, this is the first case report of successful extracorporeal membrane oxygenation in complicated scrub typhus in Korea.
-
Keywords: extracorporeal membrane oxygenation; scrub typhus; tsutsugamushi
Scrub typhus is an acute bacterial infection caused by Orientia tsutsugamushi. It is transmitted to humans through the bite of infected chiggers and the larval stage of mites. The disease is endemic in regions of eastern Asia and the southwestern Pacific islands, and northern Australia.[1] It usually presents as an acute undifferentiated febrile illness and may involve multiple organs. Severe complications, such as acute respiratory distress syndrome (ARDS), hepatitis, renal failure, meningoencephalitis, and myocarditis with shock are typically the result of mis-diagnosis and delayed treatment, and lead to a prolonged recovery as well as increased mortality.[2,3] Here, we present the case of a 20-year-old woman with scrub typhus-induced complications, who was treated successfully with veno-veno type extracorporeal membrane oxygenation (ECMO).
Case Report
A 20-year-old female, with no previous medical history, was admitted to our hospital with progressive dyspnea on October 7, 2013. One week prior to admission, she had influenza-like symptoms such as fever and myalgia. Several days before admission, she experienced dyspnea and a productive cough; thus, she visited her local hospital and was treated for pneumonia. However, she was then referred to our emergency room because she developed worsening of her breathlessness. The patient, who lived in Seoul, was a college student. Approximately 1 month prior to the development of her symptoms, she had visited her Grandparents’ graves in the mountains of northern Gyeonggi province. On admission, she had a blood pressure of 56/35 mmHg, a pulse rate of 150 beats/min, a respiratory rate of 30 breaths/min, and a body temperature of 37.1°C. She was alert but in obvious distress from severe dyspnea. Physical examination revealed conjunctival suffusion, and her neck was found to be supple. Chest auscultation revealed bilateral crackles in the area of the lower lung field with no cardiac murmur. Her abdomen was soft, non-distended with normal active bowel sounds. The liver and spleen were not palpable. There was no skin rash, petechiae, or eschar. However, the patient reported that a rash had appeared over her trunk several days previously and had just disappeared before her admission to hospital. Chest radiography and computed tomography showed pneumonia and pulmonary edema (Fig. 1). Laboratory test results were as follows: white blood cell count, 24,190 cells/μL (segmented neutrophils, 83.7%); alkaline phosphatase, 185 U/L; aspartate aminotransferase, 164 U/L; alanine aminotransferase, 99 U/L; total and fraction bilirubin levels, normal. Cardiac enzyme and brain natriuretic peptide (BNP) levels were elevated (creatine kinase, 300 IU/L; creatine kinase-myocardial band, 31.5 ng/mL; troponin I, 5.16 ng/mL; BNP, 703 pg/mL). The patient was found to be negative for human immunodeficiency virus, hepatitis B, and hepatitis C. Blood, sputum, and urine specimens were sent for culture, together with urine and blood samples for detection of pneumococcal and legionella antigens. Arterial blood gas on 70% oxygen by non-rebreathing mask revealed a pH of 7.157, a partial pressure of carbon dioxide of 46.5 mmHg, a partial pressure of oxygen of 47.8 mmHg, and a bicarbonate level of 14.6 mmol/L. Mechanical ventilator support for ARDS was started, and the patient was then admitted to the medical intensive care unit. Despite maximal inotropic and ventilator support, the patient’s hemodynamic and ventilator parameters deteriorated further and were considered incompatible with survival. Therefore, 1 hour after admission, veno-veno type ECMO was established promptly by percutaneous technique. Rapid improvement of the patient’s hemodynamic and ventilatory parameters was obtained. Echocardiography was performed after ECMO insertion and this detected severe left ventricular (LV) systolic dysfunction, with a LV ejection fraction of 21% and preserved apical and basal wall motion. Therefore, myocarditis was suspected in addition to ARDS. Considering that the many causes of myocarditis include viral infections, various viral polymerase chain reaction tests were performed. During ECMO, mechanical ventilation was maintained at minimal settings, in controlled mode (minute volume, 5 L; positive end-expiratory pressure, 5 cmH2O; fraction of inspired oxygen, 0.3). On the third hospital day, the presence of scrub typhus was highly suspected based on positive findings with an indirect microimmunofluorescent antibody for O. tsutsugamushi (IgG and IgM antibody titer, 2560), and the fact that the patient had visited the mountains of the northern Gyeonggi province area in Korea in autumn. Other bacterial, fungal, and viral culture and serological tests were all negative. Antibiotic treatment was changed to oral doxycycline (100 mg bid), and intravenous levofloxacin (750 mg qd) was added empirically because of her atypical clinical manifestations. After an appropriate antibiotic course, the patient recovered dramatically. Chest radiography showed improvement in her pneumonia and pulmonary edema, and LV ejection fraction was improved to 56%. ECMO support was successfully discontinued on her seventh day in hospital, and she was weaned from ventilator support one day later. On the twelfth day of admission, the patient was discharged without any severe complications. As an outpatient, she has remained stable with normalized heart function for over 11 months.
Discussion
Scrub typhus is one of the most common infectious disease in the Asia-Pacific region and an estimated 1 million cases occur annually. The patients with scrub typhus typically become afebrile within 48 hours of starting therapy with appropriate antibiotics, which includes doxycycline, azithromycin, rifampin, or chloramphenicol. However, some cases progress to serious complications despite appropriate antibiotic therapy. Complications may include ARDS, acute renal failure, myocardiitis, or septic shock. Disease severity depends on geographic differences, serotypes or genotypes, patient immunity, load of pathogen, and the affected organs. A retrospective study reported that 11.1% of scrub typhus cases developed ARDS, and 25% of these patients were dead.[3]
This article reports the case of a college student who had visited her relatives’ houses and Grandparents’ graves in the mountains of northern Gyeonggi province. The patient was admitted to our hospital complaining of fever and respiratory distress. Chest radiographs showed changes compatible with ARDS, and elevation of liver and cardiac enzyme was noted. A final diagnosis of scrub typhus with ARDS and myocarditis following heart failure was made based on the patient’s history of exposure, symptoms, and serological test results.
The challenge The challenge of diagnosing scrub typhus is that the initial clinical symptoms are nonspecific and patients often present to the clinicians with the appearance of common cold. In addition, routine laboratory studies are not specific for scrub typhus at all. Regarding the typical clinical manifestations of scrub typhus, following clinical symptoms have been suggested: fever, headache, eschar, rash and lymphadenopathy. According to one report, 83% of cases show 1 to 3 clinical symptoms and 10% show 4 to 5 symptoms.[6] Eschar and lymphadenopathy were not found in the current patient. A purpuric rash, which is very unusual, appeared in her lower extremities 3 days after admission. Clinicians must have a high degree of suspicion and knowledge of the various clinical manifestations of scrub typhus, which allows early diagnosis and prompt treatment and it may help reduce the possibility of serious complications and mortality.[7,8] In addition, the healthcare provider needs to keep scrub typhus in mind as a possible diagnosis when handling cases with a history of travel to endemic areas or exposure in rural areas.[9,10] Despite their widespread use, all of the currently available serological tests for scrub typhus are limited by a lack of specificity and sensitivity.[11] It is agreed that a ≥ 4-fold increase in antibody titer between two consecutive samples is diagnostic for this disease.[12] We could not check the antibody tier in a second serum sample in the current case because the patient and her parents refused further investigations. However, a high antibody tier was detected in a single acute serum sample in this patient.
ECMO not only improves systemic tissue oxygenation when the lungs are severely diseased or damaged, but also relieves the ventilation burden from the lungs, allowing the pulmonary system to rest or recover. Considering the rapid response to antibiotic treatment in scrub typhus than in other infectious causes of ARDS, ECMO could be used as an important “bridge to recovery” from ARDS in patients with scrub typhus refractory to conventional modalities. In our patient, ECMO was was tried without hesitation, because potentially reversible respiratory and heart failure were suspected, and she eventually recovered on her seventh day. Future studies should be conducted to investigate the influence of patient age on the clinical effects on ECMO as well as its long-term effectiveness.
NOTES
-
No potential conflict of interest relevant to this article was reported.
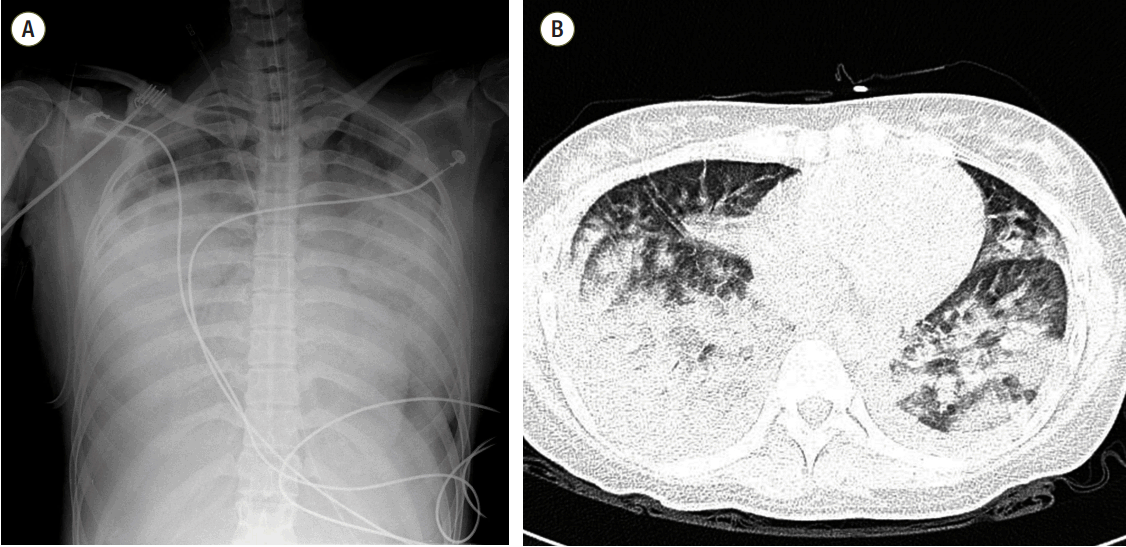
Fig. 1.(A) Chest radiograph showing pneumonia and pulmonary edema. (B) Chest computed tomography showing bilateral pulmonary infiltrates.
References
- 1. Kelly DJ, Fuerst PA, Ching WM, Richards AL. Scrub typhus: the geographic distribution of phenotypic and genotypic variants of Orientia tsutsugamushi. Clin Infect Dis 2009;48 Suppl 3:S203-30.ArticlePubMed
- 2. Tseng BY, Yang HH, Liou JH, Chen LK, Hsu YH. Immunohistochemical study of scrub typhus: a report of two cases. Kaohsiung J Med Sci 2008;24:92-8.ArticlePubMed
- 3. Wang CC, Liu SF, Liu JW, Chung YH, Su MC, Lin MC. Acute respiratory distress syndrome in scrub typhus. Am J Trop Med Hyg 2007;76:1148-52.ArticlePubMed
- 4. Sonthayanon P, Chierakul W, Wuthiekanun V, Phimda K, Pukrittayakamee S, Day NP, et al. Association of high Orientia tsutsugamushi DNA loads with disease of greater severity in adults with scrub typhus. J Clin Microbiol 2009;47:430-4.ArticlePubMedPMC
- 5. Lee CS, Hwang JH, Lee HB, Kwon KS. Risk factors leading to fatal outcome in scrub typhus patients. Am J Trop Med Hyg 2009;81:484-8.ArticlePubMed
- 6. Lee YS, Wang PH, Tseng SJ, Ko CF, Teng HJ. Epidemiology of scrub typhus in eastern Taiwan, 2000-2004. Jpn J Infect Dis 2006;59:235-8.PubMed
- 7. Moriuchi M, Tamura A, Moriuchi H. In vitro reactivation of human immunodeficiency virus-1 upon stimulation with scrub typhus rickettsial infection. Am J Trop Med Hyg 2003;68:557-61.ArticlePubMed
- 8. Tsay RW, Chang FY. Serious complications in scrub typhus. J Microbiol Immunol Infect 1998;31:240-4.PubMed
- 9. Hendershot EF, Sexton DJ. Scrub typhus and rickettsial diseases in international travelers: a review. Curr Infect Dis Rep 2009;11:66-72.ArticlePubMed
- 10. Watt G, Parola P. Scrub typhus and tropical rickettsioses. Curr Opin Infect Dis 2003;16:429-36.Article
- 11. Kelly DJ, Wong PW, Gan E, Lewis GE Jr. Comparative evaluation of the indirect immunoperoxidase test for the serodiagnosis of rickettsial disease. Am J Trop Med Hyg 1988;38:400-6.ArticlePubMed
- 12. Blacksell SD, Bryant NJ, Paris DH, Doust JA, Sakoda Y, Day NP. Scrub typhus serologic testing with the indirect immunofluorescence method as a diagnostic gold standard: a lack of consensus leads to a lot of confusion. Clin Infect Dis 2007;44:391-401.ArticlePubMed
Citations
Citations to this article as recorded by

 , Jinwoo Lee, M.D.
, Jinwoo Lee, M.D.






 KSCCM
KSCCM
 PubReader
PubReader ePub Link
ePub Link Cite
Cite


