Abstract
- Rupture limited to the lobar bronchus from blunt trauma is especially rare, and the symptoms are light so diagnosis is difficult. In a patient who visited the hospital complaining of shortness of breath after falling down, atelectasis continued in the chest x-ray. Four days after visiting the hospital, a left upper lobar bronchial rupture was diagnosed through a bronchoscopy and 3 dimensional chest computerized tomography. When diagnosis is delayed in the case of a rupture limited to the lobar bronchus, bronchial obstruction can occur from the formation of granulation tissue, so regular monitoring is important. Therefore, when atelectasis continues after blunt trauma, it is important to differentially diagnose a lobar bronchial rupture through tests such as bronchoscopy.
-
Keywords: bronchoscopy; lung injury; pulmonary atelectasis
Tracheobronchial injury from blunt trauma was reported by Seuvre in 1873.[1] There is a growing trend for this kind of trauma due to the development of modern civilization and various injuries, but it is still very rare.[2,3] Most occur in the trachea and main bronchus and the symptoms are severe, so a quick diagnosis and treatment is possible. However, ruptures limited to the lobar bronchus are very rare and the symptoms are also not severe, so in many cases, it is difficult to diagnose. Hence, the authors are reporting the following case.
Case Report
A 70-year-old female patient visited the hospital emergency room after falling from a 2 m ladder and bumping her chest on the ground. At the time of the hospital visit, her vital signs were stable and the patient only complained of shortness of breath and pain in front of her chest. From the chest auscultation, the breath sound in both lungs had slightly decreased.
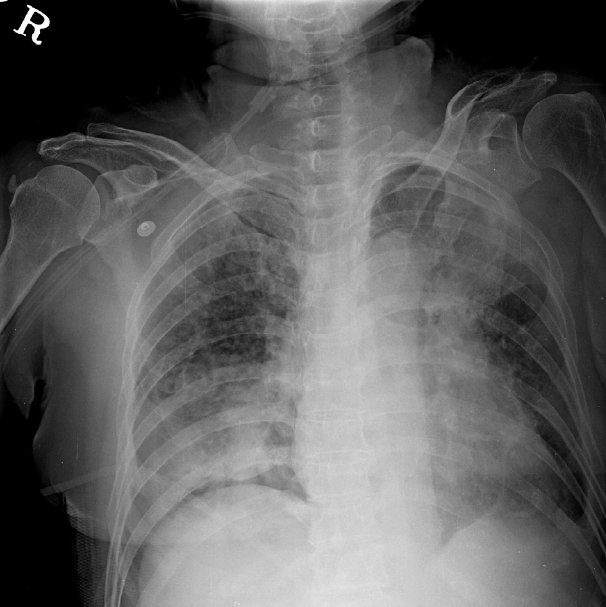
In the laboratory examination, Hemoglobin, 9.9 g/dL; Hematocrit, 31.3%; and white blood cells, 8,350 /µl. Liver function test and urinalysis were within normal range, and arterial blood gas analysis was as follows: pH, 7.3; PCO2, 36.7 mmHg; PO2, 55 mmHg; SaO2, 88%; and HCO3, 22.3 mmol/L. The acidosis and slight hypoxia were observed. In the chest x-ray (Fig. 1) and the chest computed tomography (CT), there was a right 4 – 10th left 3 – 8th rib fracture, right. Pneumothorax, multiple nodules in both lungs, and heterogeneous consolidation in the left upper, right middle, and right low lobe. A right chest tube was inserted to treat the right pneumothorax. Sputum assay was performed to differentiate active pulmonary tuberculosis, and antibiotics treatment was started under suspicion of pneumonia. The right pneumothorax improved 2 days after the chest tube insertion. However, despite the antibiotics treatment, the atelectasis of the left upper lobe had not improved in the chest x-ray performed on the 4th day after her initial hospital visit (Fig. 2); therefore, a bronchoscopy was performed to verify the cause and to administer a treatment.
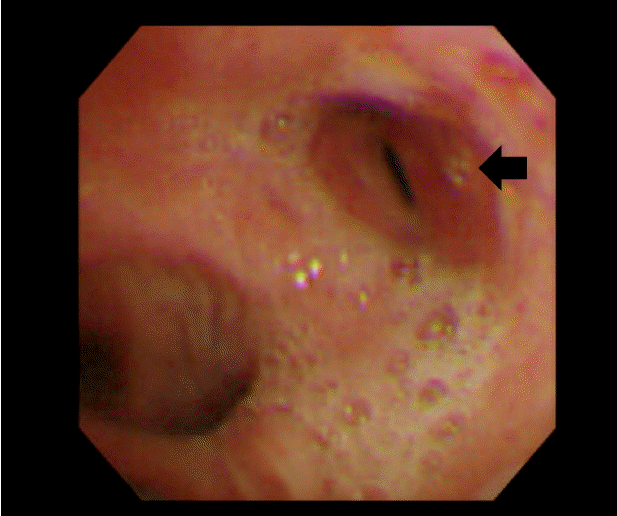
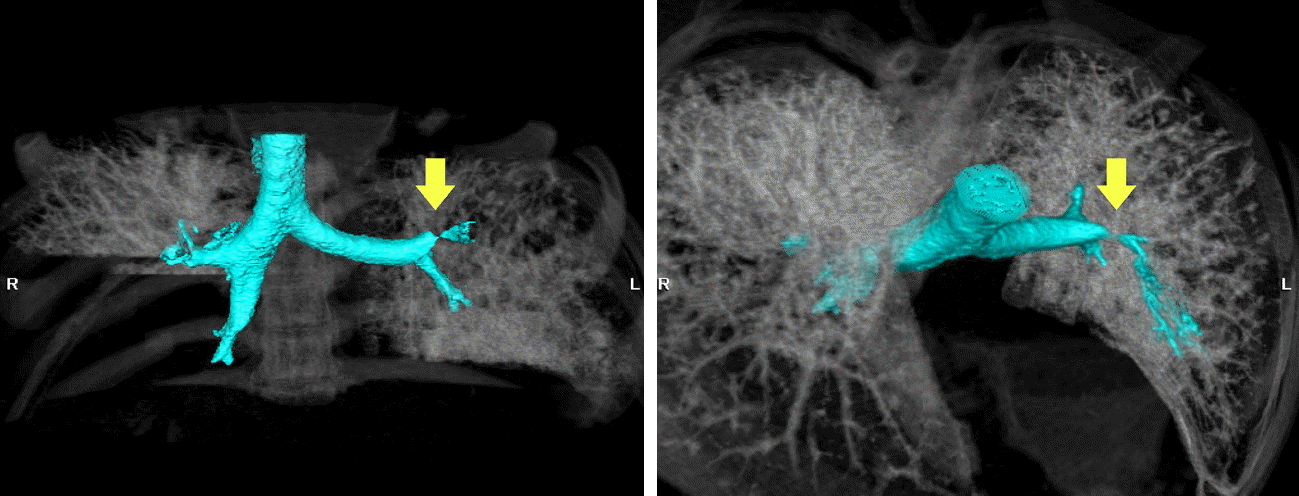
In the bronchoscopy test (Fig. 3), the left upper bronchus had become narrow in a pursed lip shape, and the bronchoscope could not be inserted further due to a narrow cavity. There was no observation of bleeding or secretion and any other granulation or scar tissue around the narrowed area. A left upper bronchial rupture was suspected, and no other abnormalities were discovered in other areas. A chest 3D CT with an airway reconstruction test was performed for a more accurate diagnosis. In the chest 3D CT with the airway reconstruction (Fig. 4), focal stenosis was observed in the left upper lobar bronchus thereby confirming a lobar bronchial rupture.
The patient showed minor symptoms from the lobar bronchial rupture, so follow-up monitoring was decided. If the symptoms became worse or the stenosis progressed in the follow-up bronchoscopy, stent insertion would be considered. On the other hand, tubercle bacillus was identified in the sputum assay so treatment for pulmonary tuberculosis was started, and the hypoxia and dyspnea symptoms improved so the patient was discharged from the hospital. We planned to follow up the patient at 4-month intervals, and chest x-ray which was took at the first visit showed persistent left upper lobe atelectasis.
Discussion
Tracheobronchial injury from blunt trauma is very rare. S. Bertelsen et al. conducted a trauma autopsy on 1,178 subjects for 5 years from 1961–1966, and tracheobronchial injury was found in 33 subjects so the incidence rate of tracheobronchial injury from blunt trauma was reported to be around 2.8%.[2,3] Riyad Karmy et al. stated that the percentage of tracheobronchial injury from blunt trauma is around 0.5%–2%.[4] When the frequency of tracheobronchial injury caused by blunt trauma is examined according to location, the reported percentage is cervical trachea 4%, distal thoracic trachea 22%, right main stem bronchus 27%, left proximal main stem bronchus 17%, complex injuries involving the trachea and mainstem bronchus 8%, and lobar bronchus 16%.[2,5] Therefore, there is very low possibility that rupture will occur in the left upper lobar bronchus from blunt trauma as was the case in this report. There are three possible scenarios for the mechanism of tracheobronchial injury from blunt trauma as follows. First, the chest wall is stretched horizontally due to the strong pressure in the front and back causing tension in the trachea and bronchus. The second scenario is due to a rapid increase in intratracheal pressure, and this occurs when pressure is applied to the chest with the glottis closed. The third scenario is due to the acceleration and rapid deceleration of the trachea structure.[2,6,7]
As this patient had a history of pulmonary tuberculosis, diagnosis of stenosis of trachea due to tuberculosis could be speculated. But most cases of endobronchial tuberculosis shows swelling, edema, ulcer, or fibrotic change of bronchial mucosa during bronchoscopy.[8] But our case didn’t show above findings, so possibility of endobronchial tuberculosis seems to be low.
The clinical features of tracheobronchial injury from blunt trauma were divided into two groups by Kirsh et al., and the criteria are damage to the mediastinum and pleura. When the mediastinum and pleura are damaged, severe dyspnea, pneumothorax, mediastinum emphysema, subcutaneous emphysema, productive cough, and even shock can appear in serious cases, while patients with no damage to mediastinum and pleura have nearly no symptoms.[3,7,9] Trachea or main bronchial ruptures are commonly accompanied by damage in the mediastinum or pleura and there are severe symptoms so diagnostic measures such as a bronchoscopy and treatment are relatively prompt. However, bronchial ruptures limited to the lobar bronchus commonly are not accompanied by damage to the mediastinum or pleura, so there are no symptoms or the symptoms are slight. The incidence rate is also very rare so it can be overlooked without any particular treatment in contrast to trachea or main bronchial ruptures. Such overlooked lobar bronchial ruptures can lead to bronchial obstruction as the granulation tissue grows in the ruptured area over a certain length of time, and there can be complications such as lung parenchymal necrosis or infection below the ruptured bronchus.[2,9,10] Therefore, a quick and accurate diagnosis is important in cases of bronchial ruptures limited to the lobar bronchus occurring after blunt trauma.
Even in this case presented here, bronchial rupture was not suspected at first with just the vital signs and symptoms exhibited by the patient. However, when the patient was hospitalized for multiple ruptures, the follow-up chest x-rays showed that atelectasis had continued, and the subsequent bronchoscopy showed a left upper lobar bronchus rupture so the diagnosis was confirmed through a 3D chest CT.
The treatment options for bronchial injury are a surgery, stent insertion and conservative management. For severe injuries, early surgeries are reported to have good long term outcomes. But surgery itself may have serious complications such as a post-operative infection, longer intensive care unit stay, and anastomotic dehiscence, and the patient may suffer long term adverse outcomes, including airway stenosis, phonation problems from injuries to the larynx, and recurrent laryngeal nerves.[2,4,11] A bronchial stent placement is a minimally invasive alternative to surgery, avoiding unwarranted thoracotomies and providing better quality of life. But stent placement also has complication such as bleeding, bronchial rupture, stent displacement, granuloma formation, and mucus impaction.[12,13] For the bronchial injury, the bronchus may be filled with fibro-granulation tissue as time passes and it can cause an airway stenosis or a complete bronchial obstruction. It can also result in recurrent pneumonia. These complications can occur varying times, from 2 weeks to 20 years, and median time took is 6 months. So it is important to follow up carefully for a long time.[11,14]
In conclusion, a rupture limited to the lobar bronchus occurring after blunt trauma can be overlooked due to difficulty in the diagnosis, and because the appropriate treatment is not performed, the symptoms can worsen and complications can occur. Therefore, in patients with blunt trauma to the chest, a more careful observation is needed even though the symptoms may not be severe, and when atelectasis is continually observed in the chest x-ray despite treatment, further tests like a bronchoscopy or 3D CT may be necessary.
NOTES
-
No potential conflict of interest relevant to this article was reported.
Fig. 1.Chest X-ray on admission shows consolidation of left upper and right low lobe.
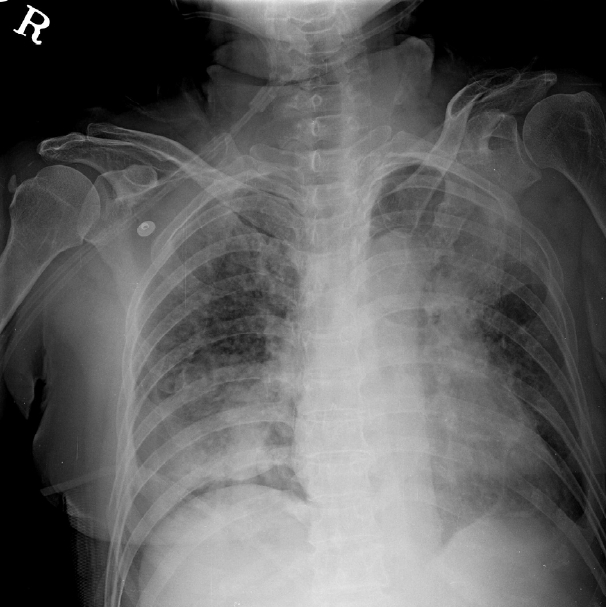
Fig. 2.Chest X-ray on 4th hospital day shows persistent left upper lobe atelectasis.
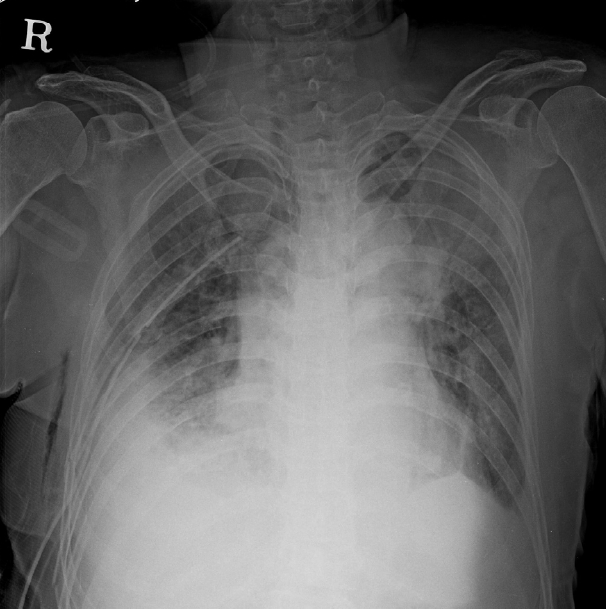
Fig. 3.Bronchoscopy shows stenosis of the left upper bronchus orifice (black arrow).

Fig. 4.Chest 3D computed tomography with airway reconstruction shows obstruction of left upper bronchus (yellow arrow).
References
- 1). Seuvre M. Crushing injury from the wheel of an omnibus: rupture of right bronchus. Bull Soc Anat Paris 1873;48:680.
- 2). Kiser AC, O'Brien SM, Detterbeck FC. Blunt tracheobronchial injuries: treatment and outcomes. Ann Thorac Surg 2001;71:2059-65.ArticlePubMed
- 3). Bertelsen S, Howitz P. Injuries of trachea and bronchi. Thorax 1972;27:188-94.ArticlePubMedPMC
- 4). Karmy-Jones R, Wood DE. Traumatic injury to the trachea and bronchus. Thorac Surg Clin 2007;17:35-46.ArticlePubMed
- 5). Symbas PN, Justicz AG, Ricketts RR. Rupture of the airways from blunt trauma: treatment of complex injuries. Ann Thorac Surg 1992;54:177-83.ArticlePubMed
- 6). Kirsh MM, Orringer MB, Behrendt DM, Sloan H. Management of tracheobronchial disruption secondary to nonpenetrating trauma. Ann Thorac Surg 1976;22:93-101.ArticlePubMed
- 7). Amauchi W, Birolini D, Branco PD, de Oliveira MR. Injuries to the tracheobronchial tree in closed trauma. Thorax 1983;38:923-8.ArticlePubMedPMC
- 8). Chung HS, Lee JH. Bronchoscopic assessment of the evolution of endobronchial tuberculosis. Chest 2000;117:385-92.ArticlePubMed
- 9). Ayed AK, Al-Shawaf E. Diagnosis and treatment of traumatic intrathoracic major bronchial disruption. Injury 2004;35:494-9.ArticlePubMed
- 10). Taskinen SO, Salo JA, Halttunen PE, Sovijäarvi AR. Tracheobronchial rupture due to blunt chest trauma: a follow-up study. Ann Thorac Surg 1989;48:846-9.ArticlePubMed
- 11). Prokakis C, Koletsis EN, Dedeilias P, Fligou F, Filos K, Dougenis D. Airway trauma: a review on epidemiology, mechanisms of injury, diagnosis and treatment. J Cardiothorac Surg 2014;9:117. ArticlePubMedPMCPDF
- 12). Kirsner KM, Sarkiss M, Brydges GJ. Treatment of tracheal and bronchial tumors and tracheal and bronchial stent placement. AANA J 2010;78:413-9.PubMed
- 13). Liu YH, Wu YC, Hsieh MJ, Ko PJ. Straight bronchial stent placement across the right upper lobe bronchus: a simple alternative for the management of airway obstruction around the carina and right main bronchus. J Thorac Cardiovasc Surg 2011;141:303-5.ArticlePubMed
- 14). Glazer ES, Meyerson SL. Delayed presentation and treatment of tracheobronchial injuries due to blunt trauma. J Surg Educ 2008;65:302-8.ArticlePubMed
Citations
Citations to this article as recorded by








 KSCCM
KSCCM



 PubReader
PubReader ePub Link
ePub Link Cite
Cite